A groundbreaking study led by Harvard University stem cell biologists has unveiled a potential pathway to achieve scarless skin regeneration, reactivating an embryonic healing mechanism that typically deactivates shortly after birth. Published on March 20 in the esteemed journal Cell, these new findings, primarily demonstrated in mice, suggest a revolutionary approach to wound healing, promising a future where damaged skin could fully restore its original structure and function without the tell-tale signs of scarring. The implications of this research are profound, offering a glimmer of hope for millions worldwide who suffer from the physical and psychological burdens of scars resulting from injuries, burns, or surgical procedures.
Unlocking Nature’s Blueprint for Perfect Healing
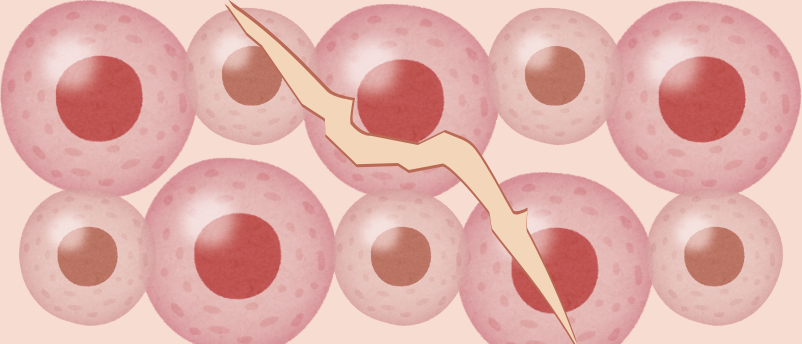
For decades, the medical community has recognized the stark difference between how a developing embryo heals and how an adult organism repairs tissue. While embryonic wounds can mend flawlessly, restoring all cellular components and leaving no trace of injury, adult skin healing typically results in a fibrous scar. This scar tissue, primarily composed of dense collagen deposited by fibroblasts, provides structural integrity but lacks the complex array of specialized cells found in healthy skin, such as hair follicles, sweat glands, vascular networks, and nerves. This fundamental alteration means that scarred skin, despite being "healed," remains functionally compromised and aesthetically distinct from its original state.
The Harvard research, spearheaded by Professor Ya-Chieh Hsu, a principal faculty member at the Harvard Stem Cell Institute, challenges the long-held notion that complete skin regeneration is an entirely new process that must be painstakingly engineered. Instead, Hsu and her team propose that the inherent regenerative potential already exists within the body, merely "held in check" by a post-natal mechanism. "Essentially, we found a way to make the wound healing outcome a lot better by learning how embryos do this so well," explained Professor Hsu. "I’m excited because we pushed the needle in a really important direction. When we have a wound, most skin cell types cannot regenerate, and we get a scar. But now I think we’ve found a way to change that, so that many cell types can regenerate, and we don’t get a scar." This perspective shifts the paradigm from building regeneration from scratch to simply removing an inhibitory "brake."
The Critical Window: An Eight-Day Transformation
The meticulous investigation, a culmination of five years of dedicated research by lead author Hannah Tam, a graduate of the Harvard Kenneth C. Griffin Graduate School of Arts and Sciences, centered on identifying the precise moment and molecular mechanisms behind the loss of regenerative capacity. Tam’s arduous work involved performing microsurgery on tiny mouse embryos and newborns under a dissection microscope, a delicate task requiring immense skill and precision.
To track the healing process, Tam utilized a biopsy punch tool to create standardized wounds, carefully observing how the skin regenerated at various time points in both embryonic and postnatal mice. One of the initial challenges was the remarkable efficiency of embryonic healing; the wounds would disappear so completely that they became indistinguishable from unwounded skin, necessitating the use of fluorescent beads and henna ink to mark the injury sites for subsequent analysis.
The researchers discovered a dramatic and rapid decline in the skin’s regenerative ability within a narrow, critical window: from three days before birth to five days after birth – a mere eight-day span. Wounds inflicted three days before birth exhibited complete regeneration, restoring diverse cell types and closely mimicking unwounded skin. In stark contrast, wounds sustained just five days after birth resulted in typical scarring, characterized by epithelial cell coverage, dense collagen deposition, abnormally concentrated nerve fibers, and an influx of immune cells. Crucially, most other specialized skin cell types failed to regrow in these postnatal wounds. This rapid transition highlighted a profound developmental switch governing regenerative potential.
The "Hyperinnervation" Breakthrough: Identifying the Molecular Brake
The next crucial step was to pinpoint the underlying molecular drivers responsible for this postnatal shift. The team meticulously analyzed the differences in gene expression and cellular composition between regenerative embryonic wounds and scarring postnatal wounds. Their breakthrough came with the discovery of "hyperinnervation" in postnatal wound sites – an excessive density of nerve fibers accumulating in the injured area.
Further investigation revealed that fibroblasts, a type of cell crucial for wound healing and scar formation, played a pivotal role. In postnatal wounds, these fibroblasts upregulated the gene Cxcl12. This gene, a chemokine, acts as a potent recruiter of nerves, drawing an abnormal abundance of nerve fibers to the wound site. This "hyperinnervation," the study found, actively impairs the regeneration of other essential skin cell types, essentially acting as the "brake" that prevents complete, scarless healing.
The researchers then conducted a series of elegant experiments to confirm their hypothesis. When they experimentally depleted Cxcl12 in wounds of postnatal mice, the hyperinnervation was significantly curtailed. Remarkably, this intervention allowed the skin to regrow diverse cell types, mirroring the regenerative capacity observed in embryonic healing. Further validating this mechanism, blocking local nerve signaling using botulinum toxin A (Botox), known for its ability to temporarily paralyze nerves, produced similar positive effects, leading to enhanced regeneration and reduced scarring.
Hannah Tam recounted a period of frustration during her research, where the team initially focused on the role of immune cells in regeneration, hitting a "wall" until they identified the critical role of fibroblast-nerve interaction. "The surprising part is that we identify a block," Tam stated, now a postdoc at Scripps Research. "And this block is through fibroblast-nerve interaction. The relationship between those two different cell types has not been the focus in wound-healing studies. I feel that this is very helpful to the field, because now we can really consider these two as actual communicators." This discovery not only provides a specific target for intervention but also opens up a new avenue for understanding the complex interplay between different cell types during wound repair.
Broader Context: The Quest for Regenerative Medicine
The challenge of scarless wound healing is a cornerstone of regenerative medicine, a field dedicated to replacing or regenerating human cells, tissues, or organs to restore or establish normal function. Current wound care primarily focuses on preventing infection, promoting closure, and minimizing scar tissue through various methods, including pressure garments, silicone sheets, steroid injections, and laser therapies. However, none of these fully restore the original skin architecture. Scars, particularly hypertrophic scars and keloids, can be disfiguring, painful, itchy, and restrictive, significantly impacting a patient’s quality of life and mental well-being. According to the World Health Organization, millions suffer from burn injuries annually, and chronic wounds, such as diabetic ulcers, affect an estimated 6.5 million people in the U.S. alone, costing billions in healthcare expenditures. The development of therapies that could prevent scarring altogether would represent a monumental leap forward, not just cosmetically, but also functionally, by preserving sensory function, flexibility, and thermoregulation.
This Harvard study aligns with other cutting-edge research in regenerative biology, which is exploring various strategies, from stem cell therapies and gene editing to biomaterial scaffolds and organoid cultures, to coax the body into repairing itself more effectively. The principle uncovered by Hsu’s team—that regeneration might be "set free" rather than "built anew"—offers a potentially simpler and more elegant solution compared to complex gene-editing or stem-cell transplantation strategies. It suggests that by understanding and manipulating endogenous inhibitory pathways, the body’s innate capacity for self-repair can be reawakened.
Implications for Human Therapies and Future Directions
The direct translation of these mouse findings to human patients represents the next critical phase of research. While the principles of embryonic development and wound healing share commonalities across species, significant differences exist. Identifying the human equivalent of the Cxcl12-mediated hyperinnervation "brake" and developing safe and effective ways to modulate it will be paramount.
The potential applications for human therapy are vast. Imagine a world where severe burn victims could heal without the painful, disfiguring, and often debilitating scars that currently necessitate extensive reconstructive surgeries and lifelong care. Surgical incisions could close flawlessly, minimizing cosmetic concerns and functional limitations. Chronic wounds, which often fail to heal due to a complex interplay of factors, might benefit from therapies that promote more complete tissue regeneration. Even common injuries and aesthetic procedures could see improved outcomes, leading to a significant enhancement in patient quality of life.
Professor Hsu expressed cautious optimism: "I didn’t think that we’d have to retract a brake, which actually is good news — it’s a lot easier. It gives me hope that this might be applicable to improving wound healing in humans." The research team’s immediate next steps will likely involve further mechanistic studies to fully elucidate the downstream effects of Cxcl12 and hyperinnervation, as well as exploring potential pharmacological inhibitors or genetic interventions that could safely target this pathway in human models. Developing topical agents or systemic treatments that can temporarily block nerve signaling or Cxcl12 expression at wound sites, without adverse side effects, would be a major focus.
The scientific community has reacted with enthusiasm to these findings. "This study marks a significant step forward in our understanding of regenerative biology," commented a leading dermatologist, who was not involved in the study. "The identification of a specific ‘brake’ rather than the need to activate a complex cascade of ‘on’ switches makes this approach particularly exciting and potentially more tractable for clinical translation. It fundamentally changes how we might approach scar prevention."
A Future Without Scars?
While clinical trials in humans are still years away, the Harvard study provides a compelling proof-of-concept. It underscores the incredible potential residing within our own biology, waiting to be unlocked. By precisely identifying and manipulating the molecular "brakes" that halt regenerative processes, scientists are moving closer to a future where healing is not merely about repair, but about true regeneration – a return to the pristine state of uninjured tissue. The journey from mouse models to human therapeutics is long and complex, but the path illuminated by this research offers a powerful new direction in the quest for scarless healing, promising to transform lives and redefine our understanding of the body’s remarkable capacity for self-renewal.












Leave a Reply