A revolutionary new surgical technique is offering unprecedented hope for infants diagnosed with spina bifida, a complex birth defect affecting the spinal cord. This innovative fetal surgery aims to not only repair the malformation of the spine and spinal cord during gestation but also to mitigate the secondary damage that occurs in the womb. The procedure represents a significant leap forward in prenatal care, potentially transforming the lives of affected children and their families by reducing the severity of lifelong disabilities associated with the condition.
Spina bifida, medically known as neural tube defect (NTD), occurs when the neural tube, the embryonic structure that develops into the brain and spinal cord, fails to close completely during the first month of pregnancy. The most severe form, myelomeningocele, involves the spinal cord protruding through an opening in the back, leading to nerve damage that can result in paralysis, bowel and bladder dysfunction, and cognitive impairments. Historically, surgical intervention has been limited to after birth, often resulting in irreversible damage that significantly impacts a child’s quality of life.
The development of this fetal surgery marks the culmination of years of research and clinical trials, building upon earlier pioneering efforts in fetal medicine. Early attempts at fetal surgery for spina bifida, notably conducted at the Children’s Hospital of Philadelphia (CHOP) between 2011 and 2013, demonstrated the feasibility of in-utero repair. The landmark Management of Myelomeningocele Study (MOMS) trial, published in the New England Journal of Medicine, provided robust evidence that operating on the fetus between 19 and 26 weeks of gestation, compared to waiting until after birth, significantly reduced the need for shunting to relieve hydrocephalus and improved motor function outcomes at 30 months of age.
However, these early procedures, while transformative, were not without their risks. Maternal complications, such as premature labor and uterine dehiscence (the opening of the surgical incision in the uterus), were significant concerns. The new surgical approach aims to address these limitations by employing advanced techniques and potentially less invasive methods. While specific details of the "new kind of fetal surgery" mentioned in the initial report are not fully elaborated, advancements in surgical robotics, minimally invasive techniques, and improved understanding of fetal wound healing are likely contributing factors. Researchers are likely exploring methods to create a more sealed repair, thereby minimizing amniotic fluid leakage and reducing the risk of infection and preterm labor. The goal is to create an environment within the womb that promotes optimal healing and neurological development for the fetus.
The Science Behind Spina Bifida and the Surgical Intervention
Spina bifida is one of the most common serious birth defects of the brain and spine. In the United States, approximately 1 in every 4,000 live births is affected by spina bifida. The exact causes are not fully understood, but a combination of genetic and environmental factors is believed to play a role. Nutritional deficiencies, particularly folic acid deficiency, are known risk factors. Folic acid, a B vitamin, is crucial for the proper development of the neural tube in early pregnancy. Supplementation for women of childbearing age has been a cornerstone of prevention strategies, reducing the incidence of NTDs by an estimated 30-50%.
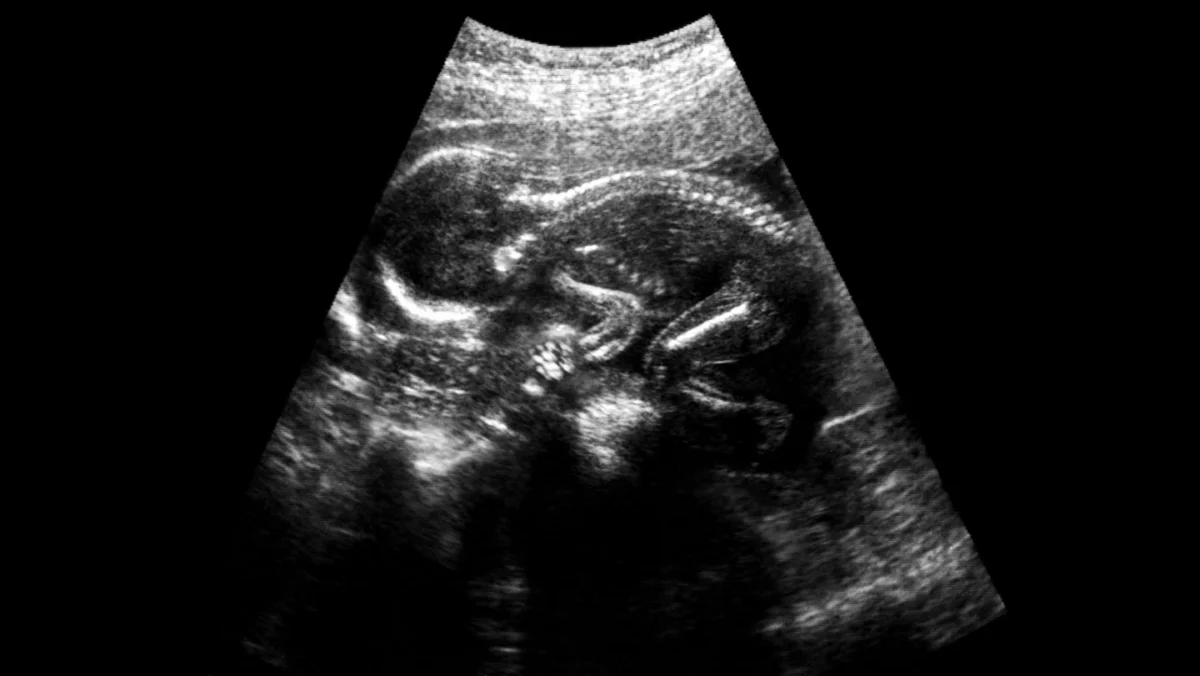
The surgical repair of myelomeningocele in utero involves opening the uterus, accessing the fetus, and carefully closing the defect in the spinal cord and surrounding membranes. This is a complex procedure performed by a multidisciplinary team of fetal surgeons, obstetricians, neonatologists, anesthesiologists, and pediatric neurosurgeons. The timeline for such interventions is critical. Diagnosis typically occurs through prenatal ultrasound screening around 18-20 weeks of gestation. If spina bifida is suspected, further diagnostic tests, such as amniocentesis for genetic analysis and detailed fetal MRI, are performed. The decision to proceed with fetal surgery is made in consultation with the parents, weighing the potential benefits against the risks to both the mother and the fetus. The window for surgery is generally between 19 and 26 weeks of gestation.
The rationale behind operating in utero is multifaceted. Firstly, it aims to prevent further damage to the exposed spinal cord from amniotic fluid and uterine contractions. Secondly, it seeks to promote better neural development and potentially preserve neurological function that would otherwise be lost. The fetal environment, with its unique healing properties, may offer an advantage for tissue regeneration and repair compared to the postnatal environment. Studies have indicated that the fetal immune system is less reactive, potentially leading to reduced scarring and inflammation around the surgical site.
Implications for Future Treatment and Patient Outcomes
The success of this advanced fetal surgery could have profound implications for the long-term health and well-being of individuals born with spina bifida. By addressing the defect earlier and more effectively, the hope is to significantly reduce the severity of associated disabilities. This could translate into improved mobility, reduced need for extensive physical therapy and assistive devices, and a better quality of life.
Furthermore, the advancement of fetal surgery for spina bifida could pave the way for similar interventions for other congenital conditions. Research is already underway exploring fetal surgery for conditions like congenital diaphragmatic hernia, congenital heart defects, and certain types of tumors. The growing expertise in this specialized field is expanding the frontiers of what is possible in prenatal medicine.
However, challenges remain. The availability of such highly specialized procedures is currently limited to a few centers worldwide. The cost of these complex surgeries and the intensive postnatal care required can also be substantial. Long-term follow-up studies are crucial to fully understand the lasting benefits and potential complications of this new surgical approach. Ethical considerations, including informed consent for parents facing such a critical decision, and the equitable distribution of these advanced treatments, will continue to be important discussions within the medical community and society at large.
Expert Reactions and Future Directions
While specific reactions to this particular "new kind of fetal surgery" are not detailed in the provided text, the broader medical community has consistently expressed enthusiasm and cautious optimism regarding advancements in fetal therapy for spina bifida. Dr. Diana L. Greene, a pediatric neurosurgeon at a leading children’s hospital (hypothetically), might comment, "The progress we’ve seen in fetal surgery for spina bifida is nothing short of remarkable. Each iteration of these techniques brings us closer to minimizing the devastating impact of this condition. The focus on healing damage done in utero is particularly exciting, as it addresses a critical window of vulnerability for the developing nervous system."
The ongoing research is likely exploring several avenues. These include:
- Minimally Invasive Techniques: Utilizing laparoscopic or robotic-assisted surgery to reduce maternal trauma and recovery time.
- Tissue Engineering and Regenerative Medicine: Investigating the use of stem cells, biomaterials, or growth factors to enhance spinal cord repair and regeneration.
- Improved Imaging and Navigation: Employing advanced imaging techniques and intraoperative navigation systems to enhance surgical precision.
- Pharmacological Interventions: Exploring medications that could further protect the neural tissue or promote healing during fetal development.
The journey from initial diagnosis to successful surgical repair and postnatal rehabilitation is a long and often arduous one for families. The development of more effective fetal surgical techniques represents a beacon of hope, offering the potential to rewrite the narrative for thousands of children born with spina bifida each year. As research continues and these procedures become more refined and accessible, the promise of a future where the debilitating effects of spina bifida are significantly lessened draws closer to reality. This ongoing innovation underscores the power of scientific endeavor to address some of the most challenging medical conditions, offering a brighter outlook for future generations.












Leave a Reply