The World Health Organization (WHO) has taken a significant step in its ongoing battle against antimicrobial resistance (AMR) by publishing specific Target Product Profiles (TPPs) for three priority bacterial infections. This strategic move aims to galvanize research and development efforts, directing innovation towards creating urgently needed antibiotics to counter the growing threat of drug-resistant bacteria. Dr. Yvan Hutin, Director of Antimicrobial Resistance at the WHO, emphasized the critical need for scientific advancements to keep pace with the relentless evolution of these pathogens, stating, "The scientific community has developed and approved new antibiotics in recent years. This is good, but unfortunately not sufficient to catch up with evolving drug-resistance bacteria, especially against those of greatest concern."
Global Health Priorities Defined: Three Pillars of Innovation
The newly released TPPs provide a detailed developmental framework, outlining the desired characteristics of antibacterial agents for three global health priorities: severe multidrug-resistant (MDR) gram-negative infections, severe gram-positive infections in immunosuppressed and critically ill patients, and bacterial meningitis. These profiles are directly aligned with the WHO’s bacterial priority pathogen list, a crucial tool for identifying the most dangerous and hardest-to-treat infections.
The aim of these TPPs is to foster robust collaboration between public and private sector partners. By clearly defining the scientific and clinical needs, the WHO intends to incentivize investment, de-risk the often lengthy and expensive research and development process, and ultimately accelerate the availability of new antibiotics for infections that pose a substantial healthcare burden worldwide.
Addressing Critical Threats: From Bloodstreams to Brains
The focus on these three areas reflects their significant impact on global health. Severe multidrug-resistant gram-negative infections, often referred to as "superbugs," are notoriously difficult to treat and can lead to life-threatening conditions such as sepsis, pneumonia, and urinary tract infections. Gram-positive infections in vulnerable populations, including those who are immunocompromised or critically ill, also present a severe challenge, with existing treatments becoming less effective.
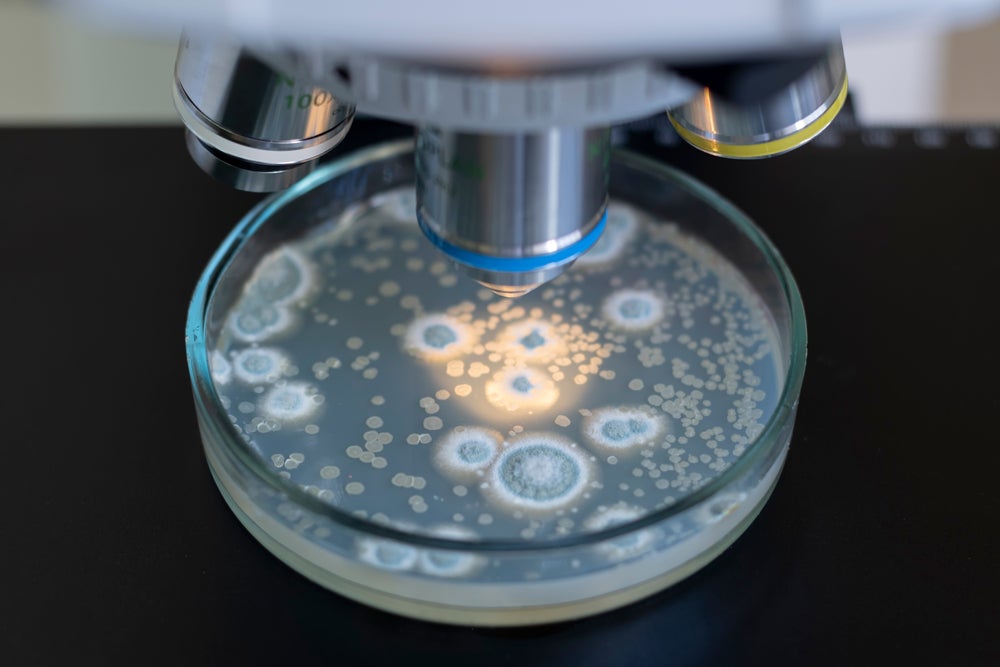
Bacterial meningitis, a severe inflammation of the membranes surrounding the brain and spinal cord, remains a particularly dangerous disease. Despite advances in medical care, approximately one in six individuals affected by bacterial meningitis succumbs to the infection, with many survivors facing long-term neurological damage. The WHO’s prioritization of these infections underscores the urgent need for novel therapeutic interventions that can overcome existing resistance mechanisms and offer effective treatment options.
The Stark Reality: A Widening Gap in Innovation
The WHO’s latest antibacterial report, "Antibacterial 2025," reveals a concerning landscape. While approximately 90 new antibacterial agents are currently in preclinical or clinical development across various infectious diseases, a stark reality emerges when examining their targets. The report indicates that only a small fraction of these candidates are specifically designed to combat the WHO’s priority pathogens. Furthermore, an even smaller number are considered truly "innovative," meaning they represent novel mechanisms of action or target previously unaddressed resistance pathways.
This scarcity of innovative treatments for priority pathogens highlights a critical bottleneck in the global fight against AMR. The WHO’s initiative through the TPPs seeks to directly address this gap by providing clear scientific targets and encouraging the development of agents that offer a genuine advantage over existing therapies. Dr. Hutin’s statement, "We need a reliable pipeline with new antibacterial agents that are innovative, affordable and accessible to all those who need them," encapsulates the dual challenge of scientific advancement and equitable access.
The Growing Health Burden of Antimicrobial Resistance
Antimicrobial Resistance (AMR) is a naturally occurring phenomenon where microorganisms, including bacteria, viruses, fungi, and parasites, evolve to withstand the medicines designed to kill them. When bacteria develop resistance, antibiotics become ineffective, turning previously manageable infections into life-threatening conditions.
The statistics paint a grim picture of AMR’s current and projected impact. In 2023, an alarming one in six laboratory-confirmed bacterial infections globally were caused by bacteria resistant to antibiotics. The most recent comprehensive data available, from 2019, indicates that bacterial AMR was directly responsible for 1.27 million global deaths. Projections are even more dire, with estimates suggesting that AMR could cause ten million deaths annually by 2050 if decisive action, including the development of more advanced antibiotics and improved stewardship practices, is not taken. This escalating mortality rate poses a significant threat to global health security and economic stability.
A Coordinated Global Response: Challenges and Commitments
Recognizing the gravity of the AMR crisis, the WHO has been actively advocating for a strengthened and coordinated global response. In October 2025, the organization issued a call to its member states, donors, and partners to bolster efforts against AMR, requesting $85 million every two years to support these initiatives.
However, the global health landscape is subject to geopolitical shifts that can impact funding and collaborative efforts. The United States’ decision to officially exit the WHO, a culmination of domestic policy shifts, raises concerns about the future of global health initiatives. While the specific impact on AMR funding remains unclear, experts widely believe that such withdrawals can hamper the agency’s capacity to address critical public health issues. Historically, the US has been the WHO’s largest donor, making its departure a significant concern for the continuity of vital health programs.
Despite these challenges, several regions and nations have demonstrated their commitment to combating AMR through independent campaigns and substantial investments. The United Kingdom, for instance, pledged £210 million (approximately $267.7 million) to bolster antibiotic-resistant bacteria surveillance across Asia and Africa. This significant investment supports The Fleming Fund’s global AMR surveillance program, aiming to detect dangerous superbugs before they can spread and impact domestic health systems. Similarly, in September 2025, the European Union launched a €253 million initiative to combat AMR, underscoring a regional commitment to tackling this pervasive threat.
The Road Ahead: Bridging the Innovation Gap
The WHO’s new Target Product Profiles represent a critical step in a multi-faceted strategy to combat AMR. By providing clear guidance and fostering collaboration, the organization aims to reignite innovation in antibiotic development. The success of this initiative will depend on sustained commitment from governments, pharmaceutical companies, research institutions, and international organizations.
The challenge of AMR is complex, requiring not only the development of new drugs but also a global shift towards responsible antibiotic use in human and animal health, improved infection prevention and control measures, and enhanced surveillance systems. The WHO’s TPPs are a vital component of this broader strategy, aiming to ensure that the scientific community is not only aware of the evolving threat but also equipped and incentivized to develop the solutions needed to protect global health for generations to come. The future hinges on bridging the gap between evolving bacterial resistance and the pace of scientific innovation, ensuring that effective treatments remain available when patients need them most.










Leave a Reply