The landscape of obesity treatment, a market projected to reach a staggering $1 trillion, is undergoing a profound transformation. While Glucagon-Like Peptide-1 (GLP-1) receptor agonists have heralded a new era in weight management, their initial portrayal as a universal panacea is increasingly being challenged by scientific scrutiny and real-world patient experiences. As Mark Bagnall, CEO of Phenomix Sciences, astutely observes, "I remember when we decided the internet was going to cure everything, and it didn’t…it came with a certain set of problems." GLP-1s, he contends, are experiencing a similar moment of reckoning, pushing the industry towards a more nuanced, individualized approach: precision medicine.
The Rise and Rethink of GLP-1s: A Market Transformed
The advent of GLP-1 medications has undeniably been transformative for millions. By 2025, over 30 million Americans were reportedly utilizing these therapies for weight loss, marking a monumental shift in how obesity is medically addressed. This surge in demand has propelled pharmaceutical giants to unprecedented valuations, with Eli Lilly becoming the first pharmaceutical company to surpass a $1 trillion market capitalization, largely fueled by its groundbreaking obesity medications. The aggressive marketing surrounding these drugs often painted a picture of a definitive solution, a "silver bullet" for a complex chronic disease.
However, amidst the commercial success, a chorus of scientists and medical professionals began sounding an alarm, cautioning against overconfidence in a "one treatment for all" narrative. While effective for many, GLP-1s are not universally beneficial, nor are they without their drawbacks. A survey conducted by Phenomix Sciences revealed a significant disparity between market perception and patient reality: only 33% of patients truly viewed GLP-1s as a definitive solution, indicating a gap between expectation and experience. This growing awareness of individual variability in response and tolerability is now driving a fundamental re-evaluation of obesity care.
Insiders Hedge Their Bets: The Expanding Drug Pipeline
The pharmaceutical industry itself, often a bellwether for future trends, is already demonstrating a proactive shift away from a singular focus on GLP-1s. Bagnall highlights this strategic diversification: "If you want one piece of evidence that drug companies don’t think GLP-1s are the panaceas… There are 200 new drugs in development. Some are different versions of GLP-1s, some are not GLP-1s at all. The drug companies are telling us we’re going to need a lot of different solutions."
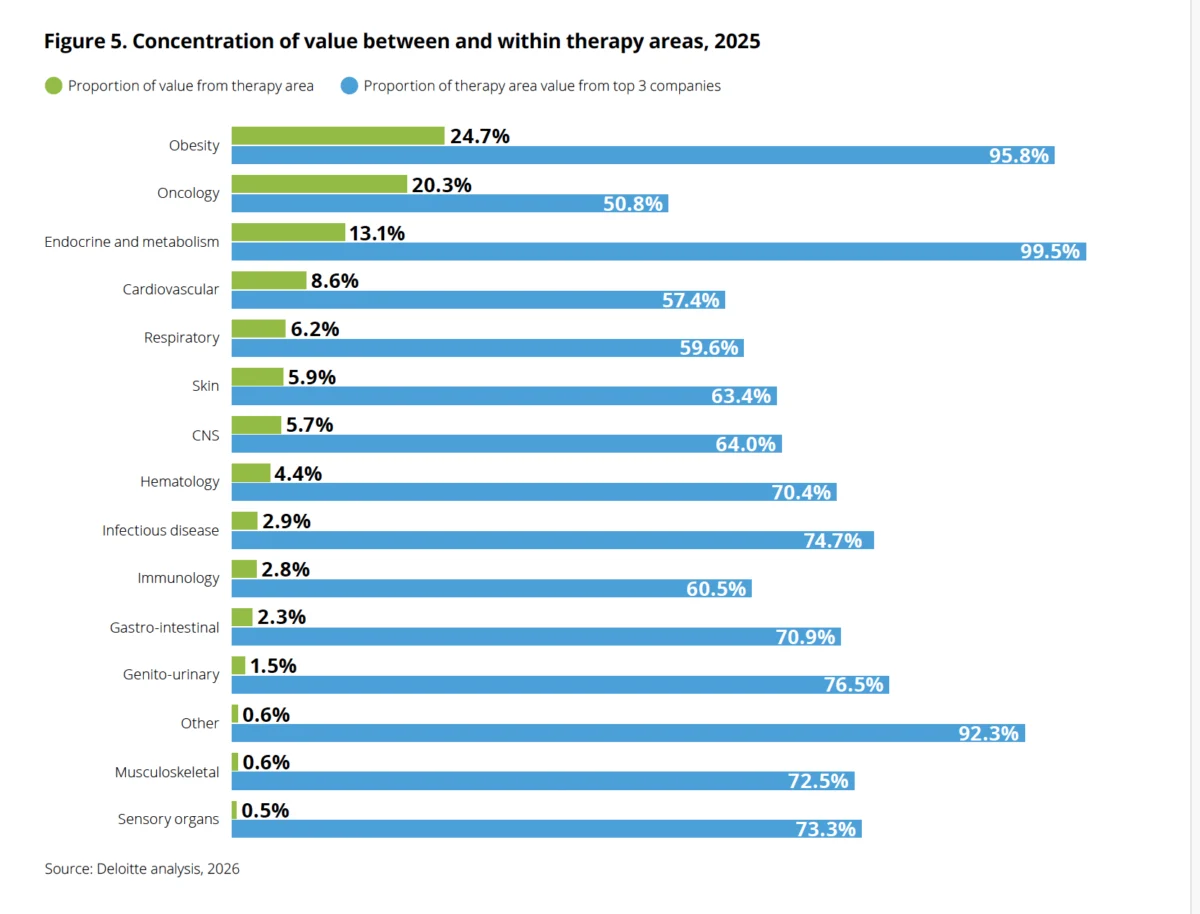
This robust research and development pipeline underscores a clear industry consensus: the future of obesity treatment is poly-pharmacological and personalized. According to TD Cowen, by 2025, there were already over 160 obesity drugs in various stages of development, exploring 68 distinct mechanisms of action. This broad investigative scope, far exceeding mere GLP-1 derivatives, signals a recognition that obesity is a heterogeneous disease requiring a diverse arsenal of therapeutic interventions. This mirrors the evolution seen in other complex diseases like cancer, where a multi-faceted approach involving various drug classes and targeted therapies has become the standard of care.
Even global health authorities, while acknowledging the utility of GLP-1s, frame them as part of a larger, comprehensive strategy. The World Health Organization (WHO), in a significant move in December 2025, issued a conditional recommendation for GLP-1 therapies, explicitly stating their role as part of a holistic approach that must include healthy diets, regular physical activity, and sustained support from health professionals. The Director-General of the WHO emphasized this critical point, stating unequivocally that "medication alone won’t solve this global health crisis." This official stance further validates the growing sentiment that a singular drug, however potent, cannot address the multifaceted nature of obesity.

The Unavoidable Reality: Side Effects and Patient Despair
Beyond efficacy, the issue of side effects has emerged as a significant concern, contributing to the re-evaluation of GLP-1s as a universal solution. While often transient, gastrointestinal effects such as nausea, vomiting, diarrhea, and constipation are commonly reported. More alarmingly, studies have highlighted a risk of muscle and bone density loss, a critical concern particularly for older or more vulnerable patient populations.
An October 2024 review from the American Heart Association cited two studies that revealed a troubling statistic: less than half of the weight lost with GLP-1 medications originated from fat, with a substantial portion coming from lean muscle mass. This finding has profound implications for long-term health. Bagnall articulates the severity of this issue: "You have to be really thoughtful, because there is a general health benefit to muscle mass – but at some point, if you’re already weak and older, now we go into a whole other category of issues: falls, broken bones."
The financial and emotional toll on patients is also considerable. The Phenomix survey indicated that only 45% of patients were fully aware of the risks associated with GLP-1s, and a concerning 17% were entirely unaware. Patients are often bearing significant out-of-pocket expenses, not only for the medications themselves but also for managing side effects, which can amount to an additional $1,000 or more. For some, side effects can be permanent, leading to the discontinuation of the medication, leaving patients feeling disillusioned and defeated. "They’ve been told there’s a silver bullet. And then six months later, nothing happened," Bagnall recounts. "I think where you really feel despair as a patient is when the thing that has been promised to you as the answer to your problems fails."
This variability in side effect profiles and tolerability strongly suggests an underlying biological basis, potentially rooted in genetic differences. This recognition forms the cornerstone of Phenomix Sciences’ mission, as they actively pursue genetic tests to identify patients most likely to benefit from GLP-1s and, crucially, those who may be intolerant, thus sparing them from adverse experiences.
Precision Medicine: The Tailored Solution
The evolving understanding of obesity, coupled with the limitations of a one-size-fits-all approach, is propelling precision medicine to the forefront of the obesity market. This paradigm shift, where treatments are tailored to an individual’s unique biological makeup, promises to revolutionize care.
Phenomix Sciences’ philosophy is deeply rooted in groundbreaking Mayo Clinic research that identified four distinct obesity subtypes, or "phenotypes": "hungry brain," "hungry gut," "emotional hunger," and "slow burn." These phenotypes are not merely descriptive labels but are scientifically defined based on different aspects of the gut-brain axis and how it regulates hunger and satiety signals. Understanding these underlying biological mechanisms allows for a far more targeted therapeutic approach.
Crucially, patients with different phenotypes respond disparately to various treatments. For instance, individuals categorized with a "hungry brain" phenotype often demonstrate favorable responses to medications like phentermine or extended-release topiramate. Conversely, those experiencing "emotional hunger" may achieve better outcomes with drugs such as Contrave. Predictably, patients exhibiting the "hungry gut" phenotype are often the ones who respond most effectively to GLP-1 receptor agonists. This targeted approach has already shown remarkable results. While older drugs like Qsymia might demonstrate an average weight loss of around 10% across a general population, in specifically identified "hungry brain patients," they can achieve up to 17% weight loss, a figure comparable to the efficacy seen with GLP-1s. This illustrates the immense potential of precision medicine to optimize existing therapies by matching them to the right patient.

The role of genetics in this individualized response is paramount. Bagnall emphasizes that genetics can account for a substantial 70% to 80% of a patient’s response to obesity drugs. This profound genetic influence underscores the necessity of diagnostic tools that can elucidate these individual differences. Phenomix Sciences is actively developing a cutting-edge test specifically designed to identify "super intolerant" patients – those who are genetically predisposed to experiencing severe and potentially permanent nausea or vomiting when taking GLP-1s. Such a diagnostic tool could prevent immense suffering and wasted resources by ensuring that patients do not embark on a treatment path that will inevitably lead to severe side effects and discontinuation.
Phenomix’s ambition is to bring this precision medicine approach to obesity treatment on a scale previously unimaginable outside of oncology. "It’ll be like oncology, but on a mass scale," Bagnall envisions. The analogy to oncology is apt, given how cancer treatment has been transformed by genomic profiling and targeted therapies.
Implications and The Future Landscape of Obesity Care
The implications of this shift towards precision medicine in obesity are far-reaching, promising a paradigm shift in patient care, pharmaceutical R&D, and healthcare economics.
Firstly, for patients, it offers the promise of more effective treatments with fewer adverse effects. Instead of trial-and-error, individuals can receive therapies specifically chosen for their unique biological profile, leading to higher success rates, better adherence, and a significant reduction in the despair caused by failed treatments. This empowers patients with a more informed and personalized journey toward health.
Secondly, for the pharmaceutical industry, it signals a move towards developing a wider array of targeted therapies and, crucially, the integration of diagnostics into drug development and prescribing practices. The growth of the diagnostics market, particularly genetic testing for drug response and tolerability, will become an essential complement to therapeutic advancements. This also presents an opportunity for smaller biotech firms specializing in diagnostics and rare disease-like obesity phenotypes to play a significant role.
Economically, while the upfront cost of diagnostic tests might be a consideration, the long-term benefits could outweigh them. By improving treatment efficacy, reducing side effects, and minimizing instances of drug discontinuation, precision medicine can lead to more efficient healthcare spending and better overall health outcomes, reducing the substantial burden obesity places on healthcare systems globally.
Looking ahead, Bagnall paints an optimistic, yet realistic, vision for the future. He predicts that within the next decade, the market will feature an impressive array of up to 50 different obesity drugs. This expanded pharmacopoeia will enable a sophisticated, multi-modal approach to obesity treatment, akin to the highly individualized strategies employed in oncology. His ultimate, ambitious forecast is that in 20 years, "we will have cured it," referring to the effective management and prevention of obesity as a public health crisis.
The journey from a "silver bullet" mentality to a precision-driven approach marks a maturation of the obesity treatment landscape. GLP-1s have opened the door, but it is precision medicine, informed by genetic insights and phenotypic understanding, that holds the key to unlocking truly effective, personalized, and ultimately, curative solutions for the complex global challenge of obesity.












Leave a Reply