The burgeoning market for obesity treatments, now valued at an astonishing $1 trillion, stands at a pivotal juncture. While GLP-1 receptor agonists have emerged as a transformative force, revolutionizing weight loss for millions, a growing chorus of experts, including Mark Bagnall, CEO of Phenomix Sciences, warns against viewing them as a universal panacea. "I remember when we decided the internet was going to cure everything, and it didn’t…it came with a certain set of problems," Bagnall remarked, drawing a parallel to the current enthusiasm surrounding GLP-1s. This sentiment underscores a critical shift in perspective: from a "one treatment for all" narrative to a more nuanced, personalized approach driven by precision medicine.
The GLP-1 Phenomenon: A Market Reshaped
The rise of GLP-1 medications has been nothing short of spectacular. By 2025, over 30 million Americans were utilizing these drugs for weight management, a testament to their efficacy in promoting significant weight loss. This unprecedented demand has had a profound impact on the pharmaceutical industry, propelling Eli Lilly to become the first pharmaceutical company in history to surpass a $1 trillion market capitalization, largely fueled by its GLP-1 offerings. The initial marketing blitz often portrayed GLP-1s as a definitive solution, a "silver bullet" for a complex, chronic disease. However, as widespread adoption continues, a more realistic picture is emerging. A recent survey conducted by Phenomix Sciences revealed that only 33% of patients truly perceive GLP-1s as a definitive answer, highlighting a significant disconnect between market perception and patient experience. This divergence signals a maturing understanding of obesity, moving beyond simplistic solutions to embrace its inherent heterogeneity.
Industry Insiders Hedge Their Bets
The pharmaceutical industry itself is already signaling a strategic diversification beyond the current generation of GLP-1s. Bagnall points to the robust development pipeline as clear evidence: "If you want one piece of evidence that drug companies don’t think GLP-1s are the panaceas… There are 200 new drugs in development. Some are different versions of GLP-1s, some are not GLP-1s at all. The drug companies are telling us we’re going to need a lot of different solutions." This proactive approach by drug manufacturers reflects a deep understanding that while GLP-1s are highly effective for many, they are not universally suitable or maximally effective for every individual with obesity.
Data from TD Cowen in 2025 further substantiates this trend, reporting over 160 obesity drugs in various stages of development, exploring 68 distinct mechanisms of action. This broad scientific exploration signifies a strategic move to address the multifaceted nature of obesity, targeting various physiological pathways involved in appetite regulation, energy expenditure, and fat metabolism. This diversified pipeline includes novel hormones, enzyme inhibitors, and gene-based therapies, all aiming to offer more tailored and effective interventions.
Even global health authorities have adopted a cautious yet supportive stance. The World Health Organization (WHO), while acknowledging the potential of GLP-1s, issued a conditional recommendation for their use as part of a comprehensive approach. This guideline, released on December 1, 2025, explicitly states that GLP-1 therapies should be integrated with healthy diets, regular physical activity, and ongoing support from health professionals. The WHO Director-General unequivocally articulated this holistic view, stating, "medication alone won’t solve this global health crisis." This official position underscores the complex interplay of biological, environmental, and behavioral factors contributing to obesity, and the necessity of multi-modal interventions.
The Uncomfortable Truth: Side Effects and Patient Awareness

Beyond efficacy, the widespread use of GLP-1s has brought the issue of side effects into sharper focus. While often transient, gastrointestinal discomforts such as nausea, vomiting, diarrhea, and constipation are commonly reported. More concerning, however, are potential long-term risks, including muscle and bone density loss. A Phenomix survey revealed a worrying gap in patient awareness regarding these risks: only 45% of patients were fully informed, and a significant 17% were entirely unaware.
An October 2024 review from the American Heart Association (AHA) cited two independent studies indicating that less than half of the weight lost with GLP-1 medications typically originates from fat mass, with a substantial portion attributed to the loss of lean muscle mass. This finding carries significant clinical implications. As Bagnall highlighted, "You have to be really thoughtful, because there is a general health benefit to muscle mass – but at some point, if you’re already weak and older, now we go into a whole other category of issues: falls, broken bones." The preservation of muscle mass is crucial for metabolic health, strength, mobility, and overall quality of life, particularly in older adults or those with sarcopenia.
The financial burden associated with managing these side effects further complicates the picture. Patients are reportedly paying up to an additional $1,000 out of pocket to mitigate side effects, a cost layered on top of the already significant expense of the drugs themselves, which often lack comprehensive insurance coverage. For some patients, side effects are not merely transient but can be persistent and severe, ultimately leading to discontinuation of the medication. This scenario can be profoundly disheartening. "They’ve been told there’s a silver bullet. And then six months later, nothing happened," Bagnall lamented. "I think where you really feel despair as a patient is when the thing that has been promised to you as the answer to your problems fails." This emotional and financial toll underscores the urgent need for more personalized and predictable treatment outcomes.
The variability in patient response to GLP-1s, both in terms of efficacy and side effects, is a key driver for the shift towards precision medicine. Genetic differences are increasingly recognized as playing a significant role in determining individual drug metabolism, receptor sensitivity, and propensity for adverse reactions. Phenomix Sciences, for instance, is actively developing genetic tests designed to identify patients who are most likely to benefit from GLP-1s and, crucially, those who may be intolerant to the medications due to severe or permanent side effects. This innovative approach aims to prevent patient suffering and optimize treatment selection from the outset, representing a significant leap forward in patient care.
Precision Medicine: The Tailored Solution
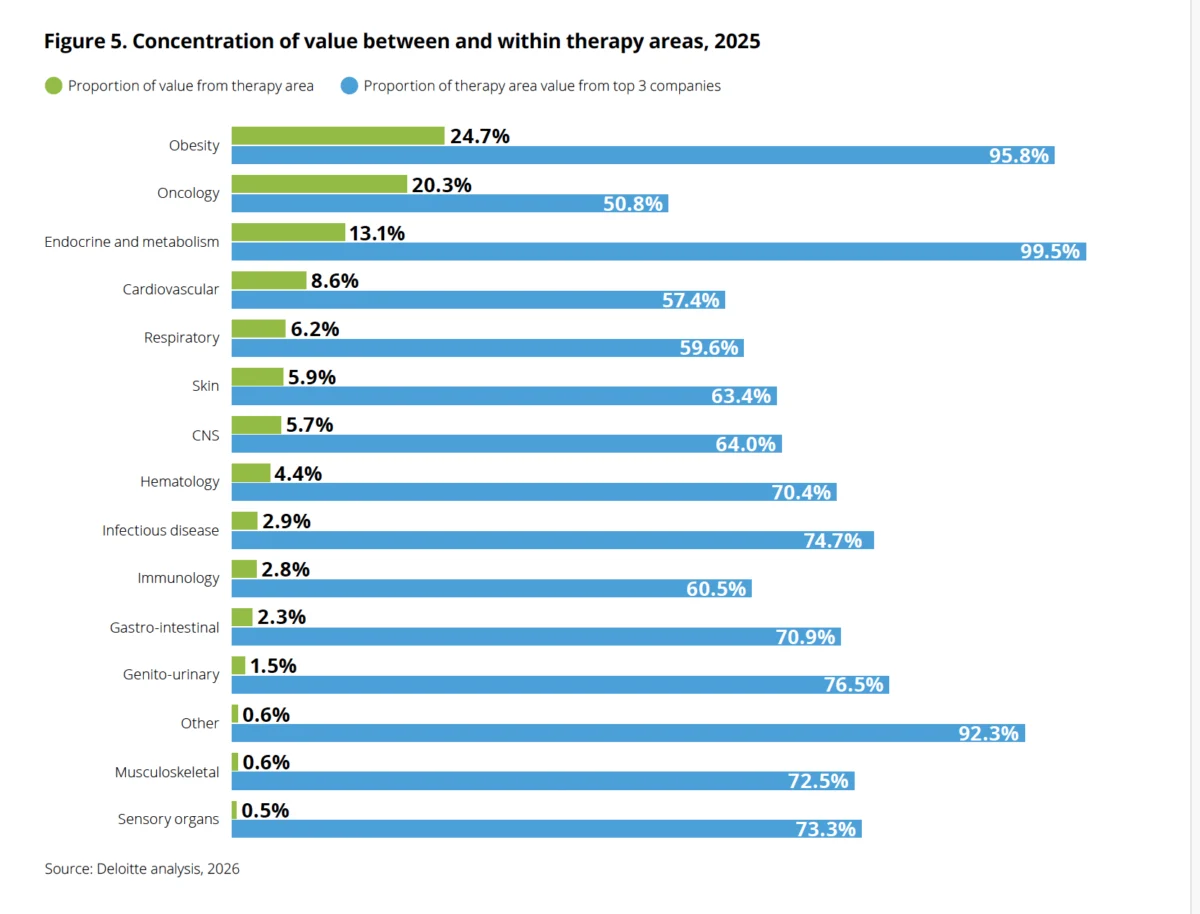
The concept of precision medicine, already transforming fields like oncology, is now poised to redefine obesity treatment. Phenomix Sciences’ philosophy is rooted in groundbreaking research from the Mayo Clinic, which identified four distinct obesity subtypes, or phenotypes: "hungry brain," "hungry gut," "emotional hunger," and "slow burn." These phenotypes are not merely descriptive labels but are based on specific dysregulations within the gut-brain axis, impacting how the body signals hunger and satiety.
Understanding these phenotypes allows for a truly personalized therapeutic strategy. For example:
- Hungry Brain: Patients in this category often experience persistent hunger signals from the brain despite adequate caloric intake. They tend to respond favorably to medications like phentermine or topiramate extended release (found in Qsymia). While older drugs like Qsymia historically showed an average weight loss of around 10%, in "hungry brain" patients, they can achieve a remarkable 17% weight loss, comparable to the efficacy seen with GLP-1s in their target population.
- Emotional Hunger: Individuals with this phenotype often use food as a coping mechanism for stress, anxiety, or other emotional states. They may benefit more from drugs like Contrave, which combines bupropion (an antidepressant) and naltrexone (an opioid antagonist) to target reward pathways and reduce cravings.
- Hungry Gut: This phenotype is characterized by a gut that sends insufficient satiety signals to the brain, leading to overeating. Patients in this group are often the best responders to GLP-1 receptor agonists, which work by mimicking gut hormones to slow gastric emptying and enhance feelings of fullness.
- Slow Burn: This phenotype is associated with a slower metabolism, making weight loss particularly challenging despite dietary and exercise efforts.
This phenotypic stratification offers a robust framework for matching the right patient to the right drug. Bagnall emphasizes the profound influence of genetics, stating that it can explain 70% to 80% of a patient’s response to obesity drugs. This genetic predisposition extends not only to efficacy but also to the likelihood of experiencing specific side effects. Phenomix’s "MyPhenome" test is designed to provide this crucial information, offering an example of the personalized reports patients can receive to guide their treatment journey.
A critical application of this precision approach is the identification of "super intolerant" patients—those who will experience severe, permanent nausea or vomiting on GLP-1s. A diagnostic test that can flag these individuals before they even start medication would be a monumental step forward, preventing significant distress, costly medical interventions, and treatment failure.

Broader Implications: Reshaping Healthcare and Patient Journeys
The advent of precision medicine in obesity management holds far-reaching implications across the healthcare ecosystem. For patients, it promises not just greater efficacy and reduced side effects, but also a renewed sense of hope and agency in managing a chronic condition. Instead of cycles of trial-and-error, individuals can embark on a treatment path tailored to their unique biology, leading to more sustainable and meaningful weight loss outcomes.
For healthcare providers, this shift necessitates enhanced training in obesity phenotyping, genetic testing interpretation, and a more nuanced understanding of the diverse drug landscape. The diagnostic tools developed by companies like Phenomix will become indispensable for informed prescribing decisions, fostering a multidisciplinary approach that integrates endocrinologists, dietitians, behavioral therapists, and genetic counselors.
The pharmaceutical industry will likely see a continued diversification of its R&D pipelines, with increasing investment in diagnostics alongside novel therapeutics. Strategic partnerships between pharmaceutical companies and diagnostic firms will become more common, reflecting an integrated approach to drug development and patient stratification. Regulatory bodies like the FDA and EMA will need to adapt their approval pathways to accommodate precision diagnostics and stratified drug indications, ensuring that these innovative tools reach patients safely and efficiently.
Economically, precision medicine could lead to more efficient healthcare spending. By optimizing drug selection from the outset, it can reduce the costs associated with ineffective treatments, managing severe side effects, and the long-term health complications of untreated or poorly managed obesity. This targeted approach promises to transform the $1 trillion obesity market from one driven by broad-spectrum blockbusters to a sophisticated, oncology-like landscape of highly personalized therapies.
Mark Bagnall envisions a future where this transformation is complete. He predicts that within 10 years, the market will feature up to 50 different obesity drugs, allowing for an incredibly sophisticated and individualized approach to treatment. Looking further ahead, he confidently states that in 20 years, "we will have cured it," suggesting a future where obesity is largely preventable or effectively managed through highly targeted interventions, much like many cancers today.
Challenges and the Road Ahead
Despite its immense promise, the journey towards widespread precision medicine in obesity is not without its challenges. Integrating these advanced diagnostic tools and personalized treatment algorithms into routine clinical practice will require significant effort in educating practitioners, overcoming inertia, and standardizing protocols. The cost and accessibility of genetic and phenotypic testing will also need careful consideration to ensure equitable access across diverse patient populations. Furthermore, ethical considerations surrounding genetic information and its use in treatment decisions will need to be addressed transparently and responsibly. It is also crucial to remember that precision medicine, while powerful, will not negate the foundational importance of healthy lifestyle interventions, which remain cornerstones of obesity management.
In conclusion, the era of the "silver bullet" for obesity is giving way to a more sophisticated, individualized approach. While GLP-1s have undeniably moved the needle, the future of the $1 trillion obesity market lies in precision medicine. By leveraging an understanding of distinct obesity phenotypes and genetic predispositions, healthcare professionals can move towards truly tailored interventions, promising improved efficacy, fewer side effects, and ultimately, a more hopeful and effective future for the millions living with obesity worldwide. This represents a monumental shift, ushering in an era where obesity is not just treated, but truly understood and managed with unparalleled specificity.










Leave a Reply