In a landmark study that bridges the gap between molecular genetics and clinical psychiatry, researchers at McGill University and the Douglas Research Centre have identified two specific types of brain cells that function abnormally in individuals diagnosed with major depressive disorder. The findings, published in the prestigious journal Nature Genetics, represent a significant leap forward in the biological understanding of depression, a condition that the World Health Organization identifies as a leading cause of disability affecting more than 264 million people globally. By utilizing high-resolution genomic mapping techniques, the research team has pinpointed disruptions in excitatory neurons and microglia, offering a microscopic look at the cellular machinery that drives mood regulation and stress response.
The study was led by senior author Dr. Gustavo Turecki, a professor at McGill University, clinician-scientist at the Douglas Institute, and the Canada Research Chair in Major Depressive Disorder and Suicide. According to Dr. Turecki, this research provides the first comprehensive map of how gene activity and the mechanisms regulating the DNA code interact within specific cell types to contribute to the pathology of depression. This discovery marks a departure from traditional "bulk" brain tissue analysis, which often averages the signals of millions of different cells, potentially masking the subtle but critical malfunctions occurring within specific cellular populations.
The Biological Foundation of a Global Health Crisis
For decades, the scientific community and the public alike have debated the origins of depression, often oscillating between psychological frameworks and biological theories. While the "chemical imbalance" theory—specifically focusing on neurotransmitters like serotonin—dominated the late 20th century, modern neuroscience has moved toward a more complex understanding of neural circuitry and gene expression. Despite this progress, the specific "drivers" of depression at a cellular level remained elusive until now.
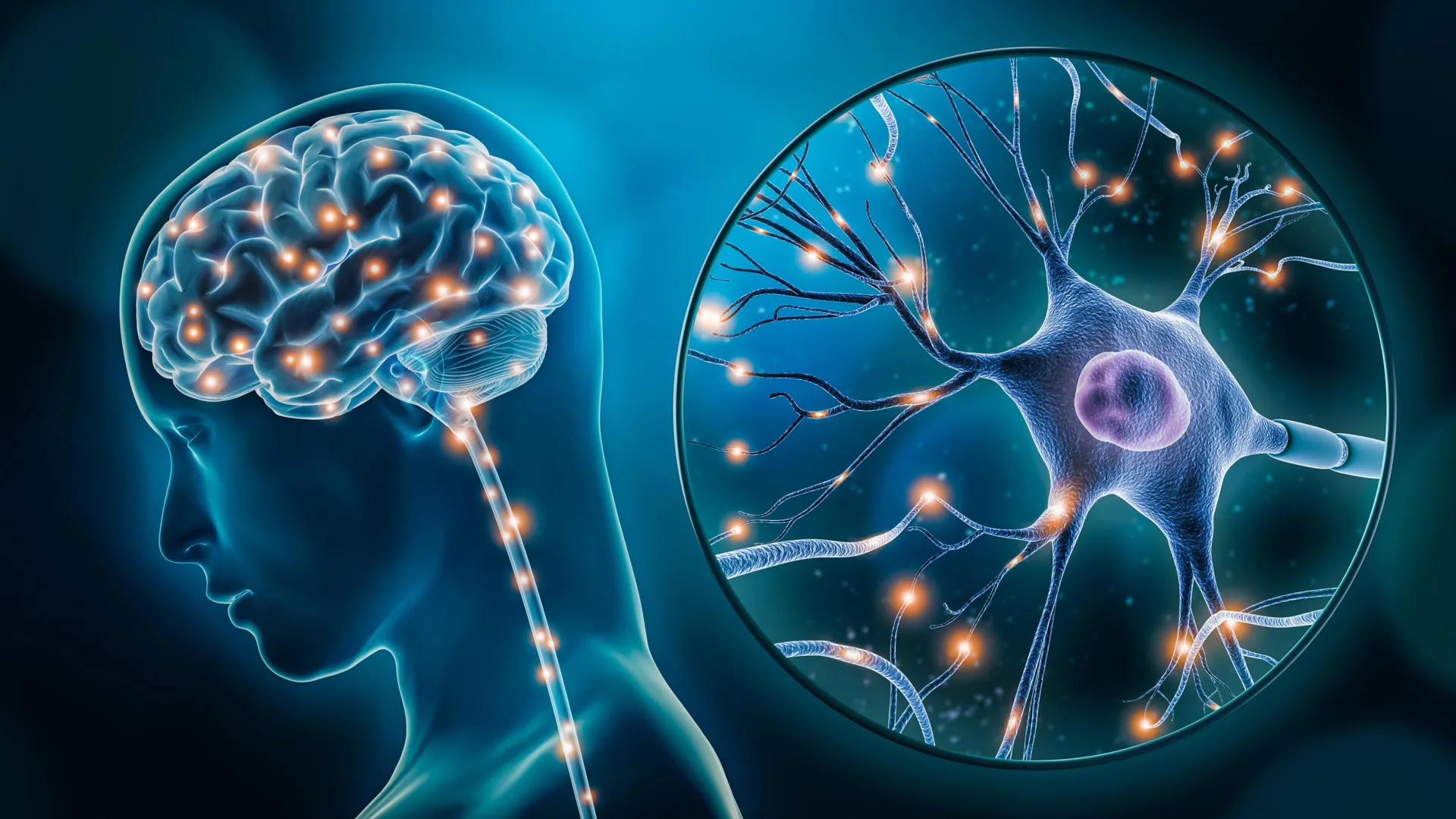
The McGill study reinforces the emerging consensus that depression is a systemic brain disorder characterized by measurable biological changes. By identifying the exact cells involved, the research team has provided concrete evidence that can be used to combat the lingering stigma that characterizes depression as a purely emotional or "invisible" ailment. The identification of excitatory neurons—those responsible for sending signals that activate other neurons—and microglia—the brain’s resident immune cells—suggests that depression may be rooted in a failure of both communication and maintenance within the central nervous system.
A Breakthrough Enabled by Rare Brain Tissue Resources
The success of this study was made possible by the Douglas-Bell Canada Brain Bank (DBCBB). Established in 1980 and located at the Douglas Research Centre in Montreal, the DBCBB is one of the world’s most significant repositories of human brain tissue. It houses over 3,500 brains, many of which were donated by individuals who lived with various psychiatric and neurodegenerative conditions.
Access to such a specialized collection allowed the researchers to conduct their analysis on post-mortem samples from 59 individuals who had been diagnosed with major depressive disorder and 41 healthy control subjects. The use of human tissue is critical in psychiatric research, as animal models, while useful, often fail to capture the full complexity of human cognitive and emotional processing. The Douglas-Bell Canada Brain Bank provides a unique window into the human brain that is unavailable through imaging techniques like MRI or PET scans, which lack the resolution to see individual gene activity within single cells.
Methodology: Single-Nucleus Chromatin Accessibility Profiling
The technical backbone of the study involved advanced single-cell genomic techniques, specifically single-nucleus chromatin accessibility profiling. This method allows scientists to look at the "epigenetic" landscape of the cell—essentially determining which parts of the DNA are "open" and available to be read by the cell’s machinery and which parts are "closed" or silenced.
By examining both the RNA (the instructions being sent out) and the DNA (the master blueprint) from thousands of individual nuclei, the researchers were able to create a high-definition profile of cellular behavior. This approach allowed them to identify "functional variants"—genetic differences that actually change how a cell operates—rather than just observing correlations. This granular level of detail is what allowed the team to separate the activity of excitatory neurons from that of inhibitory neurons, and the activity of microglia from other support cells like astrocytes or oligodendrocytes.
Key Findings: Excitatory Neurons and Microglial Dysfunction
The analysis revealed distinct abnormalities in two primary cell types:
1. Excitatory Neurons
Excitatory neurons are the workhorses of the brain’s communication network. They release neurotransmitters like glutamate to stimulate activity in other neurons. In the samples from individuals with depression, the researchers found significant alterations in the gene activity of these neurons, particularly in areas of the brain associated with mood regulation and the stress response. These disruptions suggest that the brain’s ability to process and respond to external stimuli may be fundamentally compromised at the circuit level, leading to the persistent low mood and cognitive fog associated with clinical depression.
2. Microglia and Neuroinflammation
Perhaps more surprising was the discovery of significant changes in a subtype of microglia. Traditionally viewed merely as "support cells," microglia serve as the brain’s dedicated immune system. They are responsible for "pruning" synapses (connections between neurons) and clearing out cellular debris. The McGill study found that in depressed individuals, certain microglia exhibited gene activity patterns suggestive of a dysfunctional immune response.
This finding aligns with the "inflammaging" and neuroinflammation theories of depression, which suggest that chronic stress can trigger an overactive immune response in the brain. If microglia are not functioning correctly, they may inadvertently damage healthy neurons or fail to maintain the synaptic connections necessary for healthy emotional processing.
A Chronology of Depression Research
To understand the weight of this discovery, it is helpful to look at the timeline of how depression has been studied over the last century:
- 1950s-1960s: The discovery of the first antidepressants (MAOIs and TCAs) happened largely by accident during research into tuberculosis and allergies. This led to the "Monoamine Hypothesis," suggesting depression was caused by a lack of serotonin or norepinephrine.
- 1980s: The introduction of SSRIs (like Prozac) revolutionized treatment, focusing almost exclusively on neurotransmitter levels at the synapse.
- 2000s: The Human Genome Project enabled large-scale studies (GWAS) that identified hundreds of small genetic risks for depression, but these studies could not explain how those genes caused the disease.
- 2010s: Researchers began focusing on "neuroplasticity"—the brain’s ability to rewire itself—and the role of the stress hormone cortisol.
- Present Day: The McGill study represents the "Single-Cell Era." Researchers are no longer looking at the brain as a whole, but as a complex ecosystem of distinct cell types, each with its own genetic program.
Implications for Future Treatments and Precision Medicine
The current standard of care for depression involves a "trial and error" approach to medication. Patients often wait weeks or months to see if a drug works, only for many to find that their symptoms remain. By identifying specific cell types, this research opens the door for "precision psychiatry."
If a patient’s depression is primarily driven by microglial dysfunction (an immune-related pathology), they might require a completely different class of medication than someone whose depression is driven by excitatory neuron signaling issues. Future therapies could be designed to target these specific cells, potentially reducing side effects and increasing efficacy. For instance, drugs that modulate neuroinflammation or support microglial health could become a new frontier in psychiatric pharmacology.
Furthermore, the study’s focus on chromatin accessibility—the way DNA is packaged—suggests that "epigenetic" drugs might be another avenue. These drugs would not change the genetic code itself but would change how the brain "reads" its own DNA, potentially reversing the cellular patterns identified in the McGill study.
Institutional Support and Collaborative Effort
The research, titled "Single-nucleus chromatin accessibility profiling identifies cell types and functional variants contributing to major depression," was a collaborative effort involving several leading scientists, including first author Anjali Chawla. The interdisciplinary nature of the work—combining clinical psychiatry, bioinformatics, and molecular biology—reflects the modern trend toward "team science" in tackling complex health issues.
Funding for this ambitious project was provided by several major Canadian and provincial organizations, highlighting the study’s importance to the national health agenda. Supporters included:
- The Canadian Institutes of Health Research (CIHR)
- The Brain Canada Foundation
- The Fonds de recherche du Québec – Santé (FRQS)
- The Healthy Brains, Healthy Lives (HBHL) initiative at McGill University
These organizations have increasingly prioritized research that moves beyond symptom management and toward the discovery of underlying biological mechanisms.
Conclusion: A New Chapter in Mental Health
The findings from Dr. Turecki and his team provide a much-needed roadmap for the next decade of mental health research. By moving the focus from generalized brain regions to specific cellular actors, the study provides a clearer picture of the biological disruptions that define major depressive disorder.
As the scientific community continues to digest these results, the focus will shift to clinical applications. The researchers plan to expand their work to investigate how these cellular differences manifest across different stages of life and whether they can be used as biomarkers to diagnose depression more accurately. For the millions of people living with depression, this research offers more than just data; it offers the hope of a future where mental health treatment is as precise and biologically grounded as any other field of modern medicine.














Leave a Reply