Antibody-drug conjugates (ADCs) represent a significant leap forward in targeted cancer therapy, a sophisticated class of drugs that marries the specificity of antibodies with the cytotoxic power of small-molecule payloads. This innovative approach aims to revolutionize cancer treatment by delivering potent chemotherapy directly to tumor cells, thereby minimizing collateral damage to healthy tissues and expanding the therapeutic window. The success of ADCs hinges on the intricate synergy between their biological and chemical components, a delicate balance that researchers and manufacturers are continuously striving to perfect. As the oncology landscape evolves, the growing prominence of ADCs underscores their potential to address unmet needs in treating tumors that resist conventional therapies.
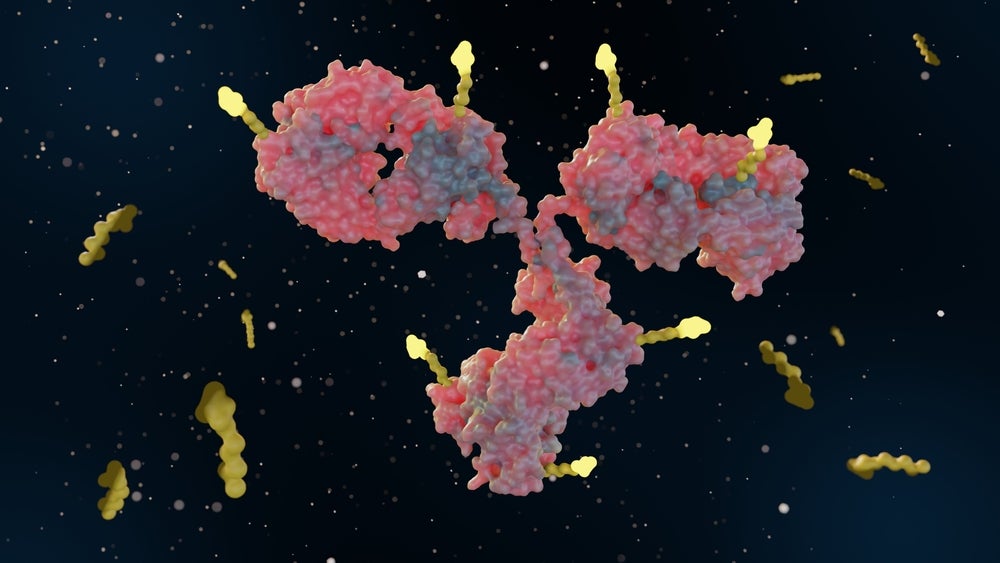
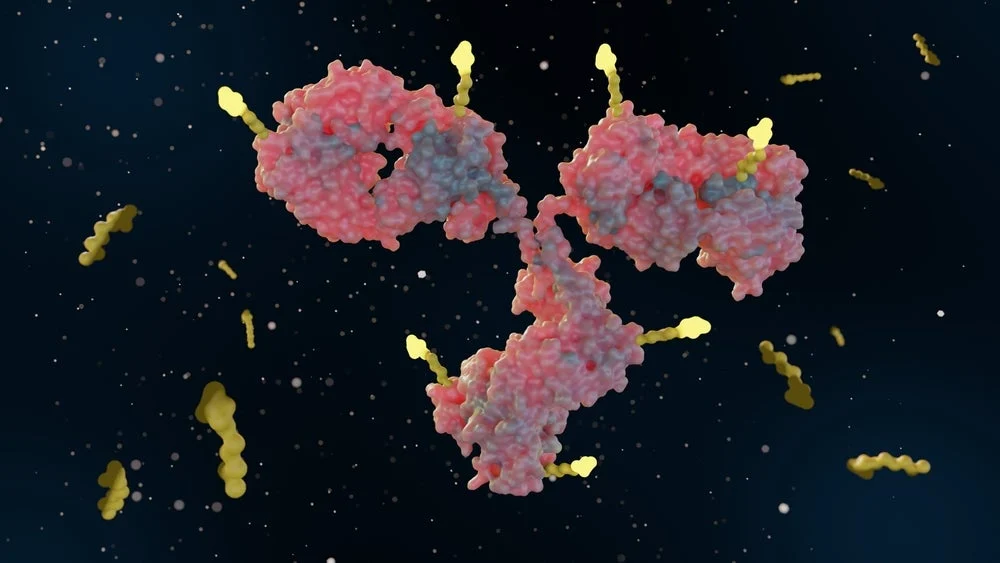
The fundamental architecture of an ADC involves three key elements: a tumor-binding antibody, a potent small-molecule payload, and a chemical linker designed to connect them. The antibody acts as a highly specific homing device, recognizing and attaching to antigens uniquely or overexpressed on the surface of cancer cells. Once bound, the ADC is internalized by the cancer cell, where the linker is cleaved, releasing the cytotoxic payload. This payload then initiates a cascade of events leading to cancer cell death. This targeted delivery mechanism offers a distinct advantage over traditional chemotherapy, which floods the entire body with toxic agents, leading to significant side effects.
The increasing interest in ADCs stems from the limitations of existing targeted therapies. Despite advancements in biomarker selection, many tumors exhibit resistance to treatments that rely on single-pathway inhibition. ADCs circumvent this by not solely depending on blocking a specific signaling pathway. Their mechanism of action involves direct engagement with the tumor cell, followed by intracellular processing and payload release, driving cell death through a more direct cytotoxic attack. This makes them particularly valuable for tackling heterogeneous tumors where not all cells may express the target antigen uniformly.
The Nuances of Target Selection for Optimal Efficacy
The selection of an appropriate antigen target is paramount to the success of an ADC. It extends beyond merely confirming the presence of an antigen on tumor cells. Critical considerations include the antigen’s density on the cell surface, the consistency of its expression across different tumor lesions within a patient, and the efficiency with which the antibody-antigen complex is internalized into the cell. Antigens that are highly shed from the tumor surface can bind to the circulating ADC, effectively sequestering the drug and reducing its delivery to the intended site. Conversely, targets with significant expression on essential normal tissues can severely compromise the safety profile of the ADC, narrowing the therapeutic margin and increasing the risk of dose-limiting toxicities. For instance, early ADC development faced challenges with targets like HER2 in certain contexts, where off-target binding to normal tissues expressing lower levels of HER2 led to cardiac toxicity.
Understanding the Bystander Effect and Emerging Resistance Mechanisms
A crucial aspect of ADC functionality is the "bystander effect." This phenomenon occurs when the cytotoxic payload released within a targeted cell diffuses to nearby cancer cells that may express lower levels of the target antigen or have lost it altogether. This can be a significant advantage in treating heterogeneous tumors, ensuring a broader anti-tumor effect. However, the bystander effect also presents a potential risk. If payload release occurs outside the tumor microenvironment, it can lead to unintended toxicity in healthy tissues.
Resistance to ADCs can manifest through various mechanisms. Cancer cells can downregulate the expression of the target antigen, thereby reducing the ADC’s ability to bind. Impaired internalization of the antibody-antigen complex, altered lysosomal processing of the conjugate within the cell, or increased drug efflux mechanisms can also contribute to resistance. Identifying and understanding these potential resistance pathways early in the drug development process is crucial for designing more robust and durable therapeutic strategies. For example, the development of ADCs targeting TROP2, a widely expressed antigen, has been a focus of research precisely because it offers a potential avenue for overcoming resistance to HER2-targeted therapies in breast cancer.
Bioconjugation: The Chemical Foundation of Consistency
The process of bioconjugation, where the antibody is chemically linked to the payload, is a cornerstone of ADC development, dictating the consistency and behavior of the drug from batch to batch. Traditional conjugation methods often involve attaching payloads to accessible lysine residues or reduced interchain cysteines on the antibody. While these methods are well-established and have been successfully employed in several approved ADCs, they can result in heterogeneous mixtures of conjugates. These mixtures may vary in the specific site of payload attachment and the number of payloads attached per antibody, known as the drug-to-antibody ratio (DAR). This heterogeneity can complicate analytical characterization, stability assessments, and potentially impact the drug’s pharmacokinetic profile and efficacy.
To address this challenge, site-specific bioconjugation techniques have emerged as a critical area of innovation. These advanced methods aim to create more homogeneous ADC populations by precisely controlling the attachment site of the payload. Common approaches include utilizing engineered cysteines introduced at specific locations on the antibody, employing enzymatic tagging strategies, or leveraging glycan-directed conjugation. By producing more uniform conjugates, these site-specific methods offer the potential for more predictable clearance rates and enhanced potency. This predictability becomes increasingly valuable as ADC manufacturing scales up to meet clinical and commercial demands. The development of technologies like the proprietary Fc-based site-specific conjugation platforms by companies such as Lonza highlights the industry’s drive towards greater precision in ADC manufacturing.
Linkers: Dictating Stability and Payload Release Dynamics
The linker plays a pivotal role in an ADC’s performance, influencing its stability in circulation and the precise conditions under which the payload is released. Linkers are broadly categorized as cleavable or non-cleavable. However, the critical question for therapeutic efficacy and safety is where the dominant cleavage occurs.
Cleavable linkers are designed to be broken down by specific triggers within the tumor microenvironment or inside the cancer cell. These triggers can include the acidic pH found in lysosomes, the presence of specific lysosomal proteases, or the reducing environment within the cell. For example, valine-citrulline linkers, often used in ADCs like Adcetris, are designed to be cleaved by lysosomal enzymes.
Non-cleavable linkers, on the other hand, rely on the natural catabolism of the antibody within the cell to release the payload. This process involves the breakdown of the antibody into smaller peptides, which then liberates the payload. The choice of linker significantly impacts the identity of the released metabolite and the types of impurities that must be carefully monitored throughout the ADC drug development lifecycle. Understanding these dynamics is crucial for ensuring both efficacy and safety. For instance, the linker technology employed by Enhertu, a trastuzumab deruxtecan conjugate, allows for a high payload release and a potent bystander effect, contributing to its remarkable efficacy in HER2-positive cancers.
The Drug-to-Antibody Ratio (DAR): A Multifaceted Attribute
The drug-to-antibody ratio (DAR) is a fundamental characteristic of any ADC, representing the average number of payload molecules attached to each antibody molecule. A higher DAR can potentially enhance cellular killing power by delivering a greater cytotoxic punch. However, it can also introduce undesirable properties, such as increased hydrophobicity, a higher risk of aggregation, and faster clearance from the bloodstream. Conversely, a lower DAR might improve the ADC’s stability and tolerability but could necessitate higher doses or the use of even more potent payloads to achieve comparable anti-tumor activity.
However, the average DAR is only one part of the story. The distribution of loaded species—meaning the proportions of antibodies with zero, two, four, six, or eight payloads—can significantly influence aggregation propensity and, in some cases, even antigen binding. For many ADC programs, controlling this DAR distribution is as critical, if not more so, than simply controlling the mean DAR. This fine-tuning ensures batch-to-batch consistency and predictable clinical behavior.
Manufacturing ADCs: Bridging Biologics and High-Potency Chemistry
The manufacturing of ADCs is a complex undertaking that integrates the established processes of biologics production with the stringent requirements of high-potency small-molecule chemistry and rigorous containment protocols. The upstream and purification stages for the antibody are crucial, as they must yield an antibody with tightly controlled levels of aggregates and charge variants. These antibody attributes directly influence the efficiency of the subsequent conjugation process and the overall stability of the final ADC product.
The conjugation step itself introduces controlled reduction or activation steps and demands an unwavering focus on keeping the concentration of free, unlinked payload below strictly defined safety limits. This requires specialized facilities and meticulous handling procedures to protect manufacturing personnel and the environment.
Streamlining Conjugation and Purification Processes
Efficient mixing and mass transfer are critical considerations during the conjugation process. If the payload is added too rapidly, local over-concentration can lead to the formation of species with excessively high DARs and increased aggregation. Similarly, uneven reduction of antibody disulfide bonds can result in disulfide scrambling, altering the antibody’s structure and generating variants that are difficult to remove during purification. Factors such as pH, temperature, and reaction time all play a vital role in shaping the final DAR profile of the ADC.
Following conjugation, purification steps are essential to remove any residual free payload, process reagents, and unwanted reaction byproducts. These purification steps also serve to tighten the product distribution, ensuring a more homogeneous final drug substance. Techniques such as hydrophobic interaction chromatography (HIC), mixed-mode chromatography, and tangential flow filtration (TFF) are commonly employed. The specific sequence and combination of these methods are tailored to the unique chemistry of the payload and linker. It is important to note that a batch that appears acceptable based on a single purity metric might still carry residual risks if significant amounts of free drug or high-DAR species remain undetected.
Analytical Rigor: Connecting Chemistry to Patient Safety
The release testing for ADCs represents a sophisticated integration of both biologics and small-molecule analytical methodologies. Intact mass analysis and peptide mapping are essential for confirming the identity of the ADC and characterizing the conjugation sites. Techniques like HIC and liquid chromatography-mass spectrometry (LC-MS) are indispensable for accurately quantifying the DAR and its distribution. Rigorous testing for free drug levels, aggregation, and subvisible particle counts is paramount for mitigating safety risks to patients.
A comprehensive overview of ADC services, encompassing discovery, conjugation, and analytical support, is vital for efficient drug development. Bioanalytical laboratory solutions play a critical role here, employing orthogonal methods to detect subtle shifts in product quality early in the development process. This allows for comparability assessments across different manufacturing process updates, ensuring product consistency over time.
The Underpinnings of "Precision" in ADC Drug Development
Effective ADC drug development thrives when biology, chemistry, and CMC (Chemistry, Manufacturing, and Controls) are viewed as an interconnected decision-making chain. Target selection is continuously refined through detailed analysis of antigen expression data and internalization kinetics. The choices of linker and payload are carefully aligned with the specific tumor biology and the desired anti-tumor effect, including the potential for a bystander effect. The bioconjugation strategy is selected to achieve an optimal balance between manufacturability and product consistency. Ultimately, ADC manufacturing is designed to exert precise control over the attributes that most significantly influence drug exposure and patient safety, with particular emphasis on DAR, linker stability, and free payload levels.
The process of scaling up ADC manufacturing from laboratory to commercial production serves as a critical stress test. Minor deviations in mixing energy, hold times, or the filtration sequence can lead to unintended widening of the DAR distribution or shifts in impurity profiles. When such changes occur, the clinical behavior of the drug can be altered, even if the batch records appear outwardly similar. This phenomenon, while often frustrating, represents a genuine constraint that necessitates meticulous process control and validation.
Furthermore, a consistent and reliable supply of the antibody starting material is equally important. Robust antibody production services help minimize variability at the outset, leading to more predictable conjugation outcomes and a more straightforward release testing process. This upstream consistency is the bedrock upon which the entire ADC manufacturing process is built.
A Realistic Perspective on Precision Oncology
The burgeoning success of antibody-drug conjugates reflects a pragmatic response to the enduring challenge of achieving more focused tumor killing while maintaining acceptable levels of patient tolerability. ADCs offer a powerful means of delivering targeted therapy for cancer, but their full potential can only be realized when target biology, bioconjugation chemistry, and ADC manufacturing are integrated and managed as a unified system. Through disciplined control of critical quality attributes such as drug-to-antibody ratio and linker stability, the promise of "precision" in cancer treatment becomes not just an aspiration, but a measurable and reproducible reality. As research and development continue, ADCs are poised to play an increasingly central role in the armamentarium against various forms of cancer, offering new hope for patients and further advancing the frontiers of precision medicine.












Leave a Reply