Pharmaceutical research and development stands at a pivotal juncture, experiencing a profound transformation that challenges long-held dichotomies in drug design. While small molecules, the traditional backbone of pharmacology, surprisingly accounted for 65% of novel drug approvals by the U.S. Food and Drug Administration (FDA) in 2025—a significant leap from 56% in both 2023 and 2024—the market simultaneously projects biologics to surpass small molecule sales by 2027, with their sales growing three times faster. This apparent paradox underscores a fundamental shift: the historical "small versus large molecule" debate is evolving into a more complex, hybrid-driven landscape where convergence, rather than competition, defines innovation.
The Evolving Pharmaceutical Landscape: A Decade of Transformation
The global pharmaceutical market has witnessed rapid expansion and a rebalancing of its core modalities over the past decade. In 2018, the market was estimated at $828 billion, with small molecules dominating 69% of sales, while biologics held 31%. By 2023, the total market had surged to $1.344 trillion, with small molecules’ share receding to 58% and biologics growing to 42%. This trajectory highlights the accelerating growth of biologics, driven by their inherent specificity and ability to address previously "undruggable" targets. Analysts widely anticipate that biologics will indeed outstrip small molecule sales within the next few years, potentially as early as 2027, marking a historic milestone in pharmaceutical economics.
This dynamic shift is not merely a battle for market share but a reflection of deeper scientific and technological advancements. Drug discovery is rapidly transitioning from a broad-spectrum approach to one of precision medicine. Breakthroughs in genomics, refined target biology, and the transformative power of artificial intelligence (AI) are empowering researchers to identify and attack diseases with unprecedented specificity and efficacy. Andreas Matern, vice president of professional services at Elsevier, aptly describes this evolution: "It’s no longer trying to shotgun blast a whole bunch of things, but instead trying to sniper and be really tight in what we’re attacking."
Pharmaceutical companies are increasingly adopting a "biology-first" approach, investing heavily in biological intelligence to thoroughly understand the target, underlying genomics, and patient population before committing to a particular drug modality. This upfront investment in data-driven insights aims to de-risk the development process and improve success rates.
AI’s Accelerating Role in Drug Discovery
Artificial intelligence is proving to be a game-changer, compressing drug discovery timelines, generating novel hypotheses, and informing crucial modality selection decisions. Advanced AI tools, including DeepMind’s AlphaFold for protein structure prediction, generative chemistry models for designing new molecules, and large language models for analyzing vast datasets, are being layered onto proprietary and public scientific repositories. This integration unlocks new insights, allowing scientists to navigate the immense chemical and biological space with greater efficiency and accuracy.
Daphne Koller, CEO and founder of Insitro, emphasized the critical role of AI at the Danaher Summit, stating, "Most programs fail in the clinic because of the early stages of the decision-making process. The focus of the next few years needs to be on increasing the success rate (the yield), rather than just efficiency. AI must help us select the right therapeutic hypotheses and the right patient populations from the start." This sentiment underscores a broader industry recognition that AI is not just about speed but, more importantly, about improving the probability of success in an inherently risky endeavor.
Defining the Modalities: A Deeper Dive
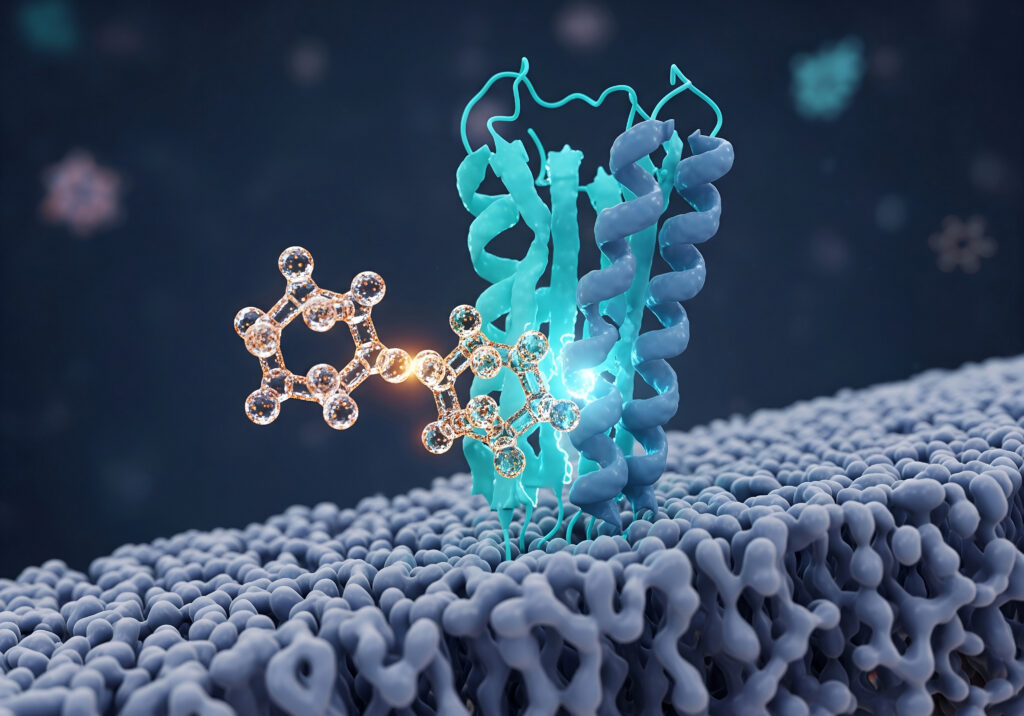
To understand the convergence, it’s essential to delineate the characteristics of small and large molecules.
Small Molecules: The Traditional Pillars
Small molecules are chemically synthesized compounds, typically characterized by molecular weights below 900 Daltons. Their diminutive size is a key advantage, enabling them to readily cross cell membranes and access intracellular targets—a vast domain that includes many disease-driving proteins. These medicines generally boast oral bioavailability, offering significant convenience for patients, are stable at room temperature, simplifying storage and distribution, and are highly manufacturable at scale, contributing to lower production costs. With well-established regulatory pathways and manufacturing infrastructure, small molecules have historically been the dominant paradigm in pharmaceuticals, forming the foundation of modern medicine.
Large Molecules: The Biologic Revolution
In contrast, large molecules, or biologics, are derived from living organisms, encompassing a diverse array of structures such as cells, proteins, and nucleic acids. These molecules are significantly more complex and substantially larger than small molecules, typically weighing over 1,000 Daltons. Their size generally prevents them from easily crossing cell membranes, necessitating administration via injection or infusion. Examples of biologics include monoclonal antibodies (mAbs), antibody-drug conjugates (ADCs), messenger RNA (mRNA) therapies, Chimeric Antigen Receptor (CAR)-T cell therapies, and engineered peptides like GLP-1 agonists. Biologics are renowned for their high specificity to their targets, which often translates to reduced off-target toxicity. However, their complexity poses challenges in manufacturing and storage, frequently requiring cold chain logistics.
The fundamental choice between these modalities is primarily dictated by target biology. Key considerations include the desired specificity, the target patient population, and whether the disease target is intracellular or extracellular. Advanced data platforms are becoming indispensable tools, aggregating published research, clinical trial data, and pipeline intelligence to inform these critical decisions. As Matern notes, "The choice of modality — whether I use a small molecule or any number of the large molecules — really comes down to understanding your target, understanding the biology."
Historically, small molecules faced limitations, primarily targeting proteins with well-defined binding pockets. This left an estimated 80% of the human proteome "undruggable" by traditional small molecule approaches. This significant gap served as a primary impetus for the development and expansion of biologics, which possess the structural diversity and binding capabilities to engage a broader range of targets inaccessible to their smaller counterparts.
The Market Landscape and R&D Investment: A Nuanced Picture
Despite the narrative of impending biologic dominance, the global small molecule drug discovery market was valued at $61.9 billion in 2025 and is projected to reach $103 billion by 2031. This resilience is fueled by AI-accelerated hit identification and lead optimization, alongside significant innovations in oral delivery. This trend is corroborated by IQVIA’s 2024 data, where Murray Aitken observed that while biologics indeed drive market value, small molecules are undergoing a "technological upgrade" through advancements like induced proximity and breakthroughs in oral delivery.
Concurrently, the global biologics market, valued at $349 billion in 2023, is projected for explosive growth, potentially reaching $1.077 trillion by 2035. This expansion is happening even as biosimilar competition intensifies, with blockbuster biologics losing patent protection. The robust innovation pipeline, encompassing new ADC approvals, the maturation of mRNA platform technology, the scaling of CAR-T and other cell/gene therapies, and the increasing regulatory traction of RNA-based therapies, continues to drive this growth.
How pharmaceutical companies approach modality investment is deeply intertwined with their size, existing infrastructure, and overarching strategic objectives. Large pharmaceutical corporations typically maintain diversified portfolios that span small molecules, biologics, and emerging modalities. This diversification allows them to absorb risk across multiple therapeutic areas and leverage extensive manufacturing infrastructure to scale various drug types. In contrast, biotech companies are often platform-driven, built around a specific modality or proprietary technology. While this specialization can lead to higher risk concentration, it also fosters faster, more focused innovation. Matern elucidates this dynamic: "Large pharma has the privilege of running diversified portfolios across molecules, biologics — maybe they can try newer modalities so they can balance some of that risk across different therapeutic areas. Whereas smaller biotechs are often built around a specific platform… a lot of biotechs are built around, ‘we have a really clever way of doing this modality — so what can we point this modality at?’" This interplay between large pharma and nimble biotechs fuels a robust deal-making environment, with large players frequently acquiring or licensing biotech platforms to access novel modalities without the lengthy process of building capabilities from scratch.
Small Molecule R&D: A Renaissance Underway
For years, the prevailing narrative in the pharmaceutical industry posited that biologics would gradually supplant small molecules as the preeminent drug modality. However, this narrative is now being actively challenged by a dynamic resurgence in small molecule R&D. A confluence of AI-driven discovery, groundbreaking chemical approaches, and innovative delivery mechanisms is unlocking previously inaccessible target classes and reaffirming the enduring value of small molecules.
The intrinsic advantages of small molecules—their oral bioavailability, scalability in manufacturing, inherent stability, ability to access intracellular targets, and lower cost of goods—ensure their continued foundational role. Matern predicts, "Small molecules will remain at the foundation because they’re scalable, they’re orally delivered, they’re stable." Consequently, small molecules are likely to remain the default modality for numerous indications, particularly in widespread areas like metabolic and infectious diseases, where broad patient access and convenient administration are paramount.
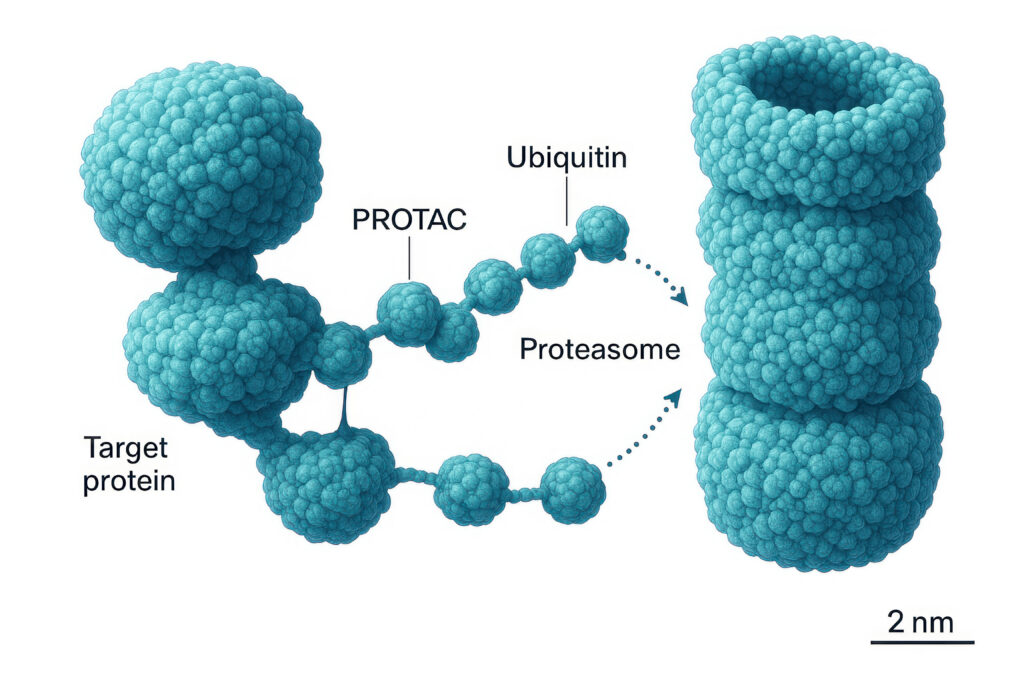
One of the most significant recent developments in small molecule R&D is the emergence of Targeted Protein Degradation (TPD). Unlike traditional inhibitors that merely block a protein’s function, degraders such as proteolysis-targeting chimeras (PROTACs) and molecular glues hijack the cell’s own ubiquitin-proteasome system—the natural protein disposal machinery—to selectively eliminate the target protein. This revolutionary approach dramatically expands the druggable target space. Proteins previously considered "undruggable" due to lacking conventional binding pockets or being too large or flexible for traditional inhibitors now become accessible.
Nello Mainolfi, CEO of Kymera Therapeutics, articulated the impact of TPD: "Targeted protein degradation allows us to reach broader patient populations compared to injectable biologics. We are developing oral drugs with biologics-like activity, reaching critical signaling nodes that have been historically ‘undruggable’ with traditional inhibitors." This technology holds immense promise for treating a wide array of diseases, including various cancers and autoimmune disorders, by offering a fundamentally different mechanism of action.
Another emerging frontier is RNA-targeting small molecules. Historically, RNA was considered an intractable target for small molecules due to its complex and dynamic structures. However, advances in structural biology, high-throughput screening, and AI are rapidly changing this perception. These molecules are designed to bind directly to specific RNA sequences, modulating their function upstream of protein expression. This opens up possibilities for addressing targets previously inaccessible to both traditional small molecules and most biologics, including transcription factors and splice sites. The substantial commercial validation came last year when Merck Group entered a $2 billion strategic collaboration with Skyhawk Therapeutics specifically focused on discovering novel RNA-targeting small molecules for neurological disorders, signaling strong industry confidence in this nascent field.
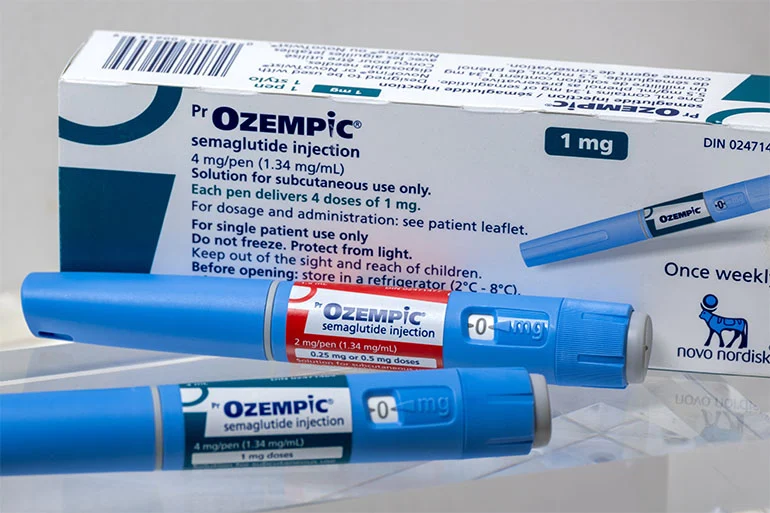
Perhaps one of the most commercially significant trends in small molecule R&D is the relentless push to make complex molecules, including peptides and other structures that traditionally required injection, orally available. The GLP-1 receptor agonist story stands as the highest-profile example of this innovation. Semaglutide, initially developed as an injectable peptide, is now available in an oral formulation, with next-generation oral small molecule GLP-1 agonists already in advanced development. This shift dramatically improves patient convenience and adherence. Matern highlights the broader implications: "If you can make complex biological drugs orally available, you expand access, you make them stable, you can deliver them to remote corners of the world without worrying about a cold chain." Oral peptide technologies are poised to unlock a new generation of drugs that combine the targeting precision characteristic of biologics with the unparalleled convenience and scalability of small molecules.
Large Molecule R&D: Expanding the Frontier
Biologics are in the midst of an unprecedented expansion, with a pipeline that is broader, more diverse, and technically ambitious than at any previous point in the industry’s history. What began with the advent of monoclonal antibodies in the 1980s has evolved into a rich ecosystem of modalities, each offering distinct mechanisms, target classes, and patient benefits.
A key advantage of biologics, particularly monoclonal antibodies (mAbs), lies in their ability to be engineered to bind a single target with extraordinary precision, thereby minimizing off-target effects and enhancing safety profiles. Proteins, receptors, and ligands located on the cell surface or circulating in the bloodstream are highly accessible to large molecules. Furthermore, many biologics offer long-lasting therapeutic effects, with some requiring only monthly or even less frequent dosing, greatly improving patient quality of life. From blocking a specific receptor to delivering a cytotoxic payload directly to diseased cells or even editing genes, biologics provide a range of mechanisms unavailable to conventional small molecules.
Monoclonal Antibodies (mAbs) remain the bedrock of the biologic pipeline. Continuous innovation sees them increasingly engineered for improved half-life, reduced immunogenicity, and enhanced targeting capabilities. A significant advancement is the development of bispecific antibodies, designed to simultaneously engage two distinct targets, enabling novel mechanisms such as redirecting T cells to specifically kill tumor cells. Another crucial large molecule class is antibody-drug conjugates (ADCs), which exemplify the convergence theme by combining the exquisite targeting precision of an antibody with the potent cytotoxic efficacy of a small molecule chemotherapy payload. This "guided missile" approach minimizes systemic toxicity while maximizing therapeutic effect.
mRNA therapies have surged to prominence since the COVID-19 pandemic, rapidly diversifying beyond infectious disease vaccines. They are now being actively explored for oncology vaccines, treatments for rare diseases, and other infectious agents. Alongside mRNA, siRNA (small interfering RNA) and antisense oligonucleotides (ASOs) represent other powerful RNA interference approaches. These therapies work by silencing disease-causing genes at the mRNA level, preventing the production of harmful proteins. They have gained regulatory approvals in rare genetic diseases and cardiovascular indications, showcasing their potential to tackle the root causes of disease.
CAR-T cell therapies represent a pinnacle of personalized medicine. These involve extracting a patient’s own T cells, genetically engineering them to recognize and destroy cancer cells, and then reinfusing them back into the patient. CAR-T therapies have achieved transformative results in hematologic malignancies, and intense research is underway to extend their efficacy to solid tumors. Similarly, CRISPR and gene editing technologies are rapidly advancing, with the first approved CRISPR therapy reaching patients in 2023, ushering in an era where genetic diseases can potentially be corrected at their source.
Oncology remains the single largest driver of biologic R&D investment and the therapeutic area where the most ambitious large molecule science is being deployed. ADCs, in particular, have experienced a wave of approvals and robust late-stage pipeline activity, with over 100 ADCs currently in clinical development globally. Immuno-oncology, encompassing checkpoint inhibitors, CAR-T, and bispecific antibodies, continues its expansion, progressively moving from treating hematologic cancers into the more challenging landscape of solid tumors.
The GLP-1 Story: A Case Study in Biologic Validation at Scale
The remarkable success of GLP-1 receptor agonists provides a compelling illustration of the commercial and scientific power of large molecule R&D, and critically, how biologic validation can catalyze small molecule innovation. Drugs like semaglutide and tirzepatide have rapidly ascended to become among the best-selling pharmaceuticals in history, unequivocally validating peptide engineering at an unprecedented scale.
Crucially, the GLP-1 narrative is also a testament to lifecycle innovation—how the clinical and commercial success of a biologic can drive subsequent development in small molecules. Matern explains, "GLP-1 is really showing how that balance is evolving. They are a peptide-based modality — technically in the large molecule category — but the commercial success is now driving innovation across small molecules: oral delivery and combination therapy." He adds, "I think we’ll see that pattern repeat. Historically, many therapies start as injectables because it’s technically simpler to deliver a complicated molecule that way. But once you get the validation of the biology and the commercial demand becomes clear, there’s a really strong investment incentive to invest in more convenient formats." The journey of GLP-1 from an injectable peptide to an oral small molecule agonist is poised to become a template for future modality evolution across a multitude of therapeutic areas, epitomizing the synergistic relationship between large and small molecules.
Implications for Stakeholders in a Converging Landscape
The evolving drug discovery landscape presents distinct imperatives and opportunities for various stakeholders within the pharmaceutical ecosystem.
For large pharmaceutical companies, the imperative is clear: strategic portfolio diversification across all modalities is crucial. This necessitates significant investment in advanced data infrastructure, including Electronic Laboratory Notebooks (ELNs), ontologies, and structured data capture systems, to leverage AI effectively. Furthermore, strategic acquisition or licensing of platform biotechs, often before their valuations fully reflect clinical validation, becomes a critical mechanism to access novel modalities and accelerate innovation.
For biotechnology companies, maintaining a focused platform remains a strength. However, the most fundable and partnerable strategies will increasingly be those that combine a truly novel modality with a well-validated target and a clear, compelling path to oral or other convenient delivery methods. This emphasis on delivery addresses a key market need and enhances patient adherence.
Investors should keenly observe advancements in delivery technology, paying particular attention to companies that are successfully solving the "last-mile problem" of safely and conveniently delivering complex molecules to their intended biological targets. This includes innovations in lipid nanoparticles, oral peptide technologies, advanced ADC linker chemistry, and next-generation formulation science.
For researchers and R&D teams, the data foundation is rapidly becoming the new lab bench. Investing in data quality, governance, and integration from day one is no longer optional but a fundamental requirement for enabling AI-powered drug discovery and ensuring the reproducibility and scalability of research efforts. Adherence to FAIR (Findable, Accessible, Interoperable, Reusable) data principles is paramount.
Conclusion: A Spectrum, Not a Competition
The perceived binary between small and large molecules is increasingly recognized as a false dichotomy. Far from being a competition for dominance, the relationship between these modalities is evolving into a synergistic spectrum, where the gray area between them continues to expand.
Andreas Matern encapsulates this perspective: "I don’t see small and large molecules competing for dominance. I think there’s going to be a continued balance… small molecules will remain at the foundation because they’re scalable, they’re orally delivered, they’re stable. And biologics will probably be where we continue to expand, where things like precision and durability matter." This balanced view suggests a future where both classes of therapeutics thrive, each leveraging its unique strengths for optimal patient benefit.
The shift from empirical trial and error to data-driven prediction represents the most consequential change in drug discovery in a generation. Organizations that invest proactively in data quality, robust governance frameworks, and seamless integration for AI-powered drug discovery will be best positioned to lead this transformation.
Ultimately, scientific insight alone is insufficient. The enduring challenge of drug discovery lies in consistently getting the right drug to the right target in the right patient. Breakthroughs in lipid nanoparticles for RNA delivery, innovative oral peptide technologies, sophisticated ADC linker chemistry, and cutting-edge formulation science represent the next wave of advancements that will enable this precision.
The ongoing expansion of the pharmaceutical modality toolkit is unequivocally good news for patients, for scientific advancement, and for the industry as a whole. More diverse tools mean an increased number of druggable targets, a wider array of addressable diseases, and ultimately, more patients benefiting from innovative therapies. The true competition is not between modalities themselves, but between organizations that embrace this complexity and adapt to the evolving landscape, and those that fail to do so.











Leave a Reply