The pharmaceutical landscape is witnessing a profound transformation with the ascendance of in vivo cell therapies, a revolutionary approach that engineers therapeutic cells directly within the patient’s body. This paradigm shift, marked by substantial investor interest and a burgeoning ecosystem of suppliers, promises to redefine the commercial viability and accessibility of advanced therapeutic modalities. Unlike their ex vivo counterparts, which necessitate the complex extraction, genetic modification, and reinfusion of a patient’s cells, in vivo therapies leverage sophisticated delivery systems, such as modified viral vectors or lipid nanoparticles (LNPs), to introduce genetic material directly into target cells within the body. This innovative strategy has ignited a wave of high-profile acquisitions and a surge in dedicated research, signaling a maturing field poised for significant clinical and commercial impact.
The rapid acceleration of in vivo cell therapy development is underscored by a series of landmark financial maneuvers in the past two years. In March 2025, AstraZeneca’s $1 billion acquisition of EsoBiotec, a prominent in vivo developer, sent ripples through the cell and gene therapy (CGT) community at the Advanced Therapies conference in London. This event, a key gathering for stakeholders in the rapidly evolving field, served as a focal point for discussing the latest breakthroughs and investment trends. The momentum continued into 2026, with Eli Lilly’s $2.4 billion acquisition of Orna Therapeutics in February, following earlier significant billion-dollar deals announced by AbbVie and Bristol Myers Squibb in the latter half of 2025. These substantial investments, often made with limited clinical data, reflect a strong conviction in the future potential of in vivo modalities. The increasing number of dedicated sessions at industry conferences, such as the 2026 Advanced Therapies event, further testifies to the growing maturity of this field, attracting substantial interest from major pharmaceutical players and fostering a dynamic environment of innovation among suppliers focused on overcoming the inherent technical and logistical challenges.
In Vivo Therapies Transition from Concept to Clinical Reality
The current landscape of in vivo cell therapies is characterized by early-stage development, with the majority of pioneering companies operating in the preclinical or Phase I stages. Davide Zocco, Head of Commercial Development for exosomes and mRNA-LNPs at the Swiss contract development and manufacturing organization (CDMO) Lonza, highlights the significance of these early-stage, high-value acquisitions by established pharmaceutical giants. "Most of the players in the field are [in] either preclinical stage or Phase I," Zocco observed, "Nonetheless, Zocco notes the high-value deals by big pharma with in vivo biotechs, a signal of the modality’s potential." This investor confidence, even in the absence of extensive clinical validation, speaks volumes about the perceived transformative power of this therapeutic approach.
David Peritt, Founder and Chief Scientific Officer of Lupagen, a Texas-based company specializing in bedside cell therapy delivery systems, corroborates this observation. "These big pharma-biotech acquisitions were made with very little clinical data," Peritt stated, emphasizing the forward-looking nature of these strategic investments.
The clinical progress of in vivo therapies is beginning to yield promising initial results. AstraZeneca’s acquired in vivo CAR-T therapy, for instance, is currently undergoing a Phase I trial (NCT06791681). An interim analysis of this trial recently reported encouraging outcomes in five multiple myeloma patients: four achieved an objective response, and three attained complete remission, as detailed in a 2026 publication in Nature. Prior to this, in late 2025, Massachusetts-based biotechs Create Medicines, developing in vivo CAR-myeloid (CAR-M) treatments, and Kelonia Therapeutics, evaluating its in vivo CAR-T therapy KLN-1010, both released early-stage data, further fueling optimism within the sector.
Adam Inche, CEO and Founder of Lentitek, a Scottish company innovating in viral vector technology, anticipates the next twelve months to be a critical period. "The next 12 months will be pivotal as more comprehensive data for in vivo cell therapies emerges," Inche stated, adding that while investor enthusiasm is palpable, the inherent risks associated with this nascent technology are still being thoroughly assessed.
Reconceptualizing In Vivo Cell Therapies Within the CGT Framework
A nuanced understanding of the terminology surrounding these advanced therapies is emerging. Adam Inche contends that the term “in vivo cell therapy” may be somewhat of a misnomer. He posits that these treatments bear a closer resemblance to gene therapies, with a key distinction: while gene therapies typically aim to correct existing cellular dysfunctions, in vivo cell therapies are designed to introduce entirely new therapeutic functions to cells. This conceptual overlap is reflected in regulatory frameworks, such as the U.S. Food and Drug Administration’s (FDA) guidance for human gene therapy products, which often groups in vivo therapies, and even distinct cell and gene therapies, under broader categories like "gene therapy" or "genomic modification." Inche suggests that the persistent use of the "in vivo" designation is largely a strategic marketing effort, aiming to capitalize on the established success and recognition of ex vivo cell therapies, particularly Chimeric Antigen Receptor (CAR) T-cell therapies.
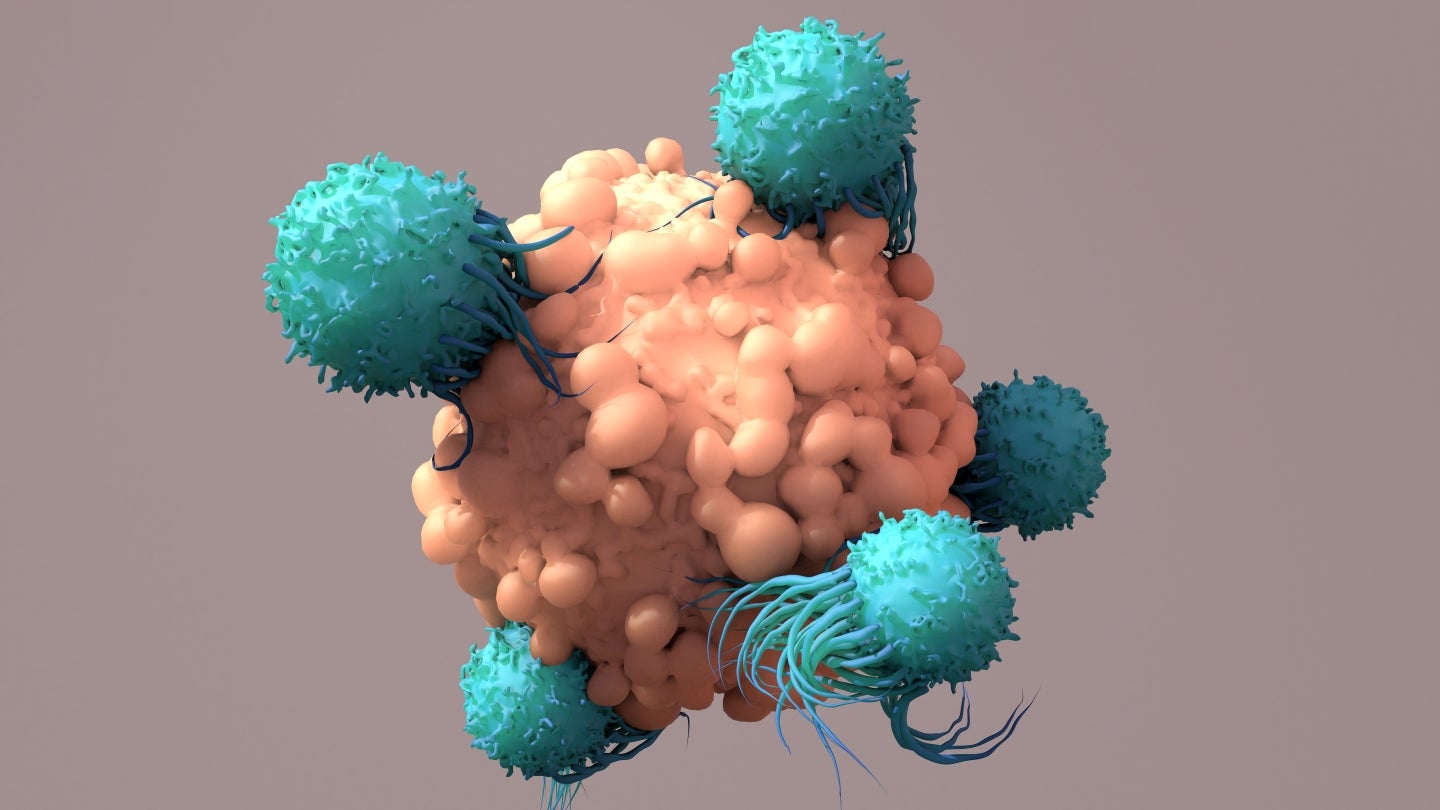
Kella Kapnisi, Head of Cell and Gene Therapy at Team Consulting, a medical device consultancy based in Cambridge, UK, concurs that these novel treatments could indeed be classified as gene therapies. A significant draw of in vivo therapies lies in their potential to deliver the benefits of off-the-shelf, allogeneic cell therapies without the extensive and costly requirements for complex processing, transportation, and storage of live cells. As David Peritt explains, "In vivo therapies shed many technical challenges that plague ex vivo therapies, but in doing so have inherited the limitations of gene therapies."
Lentitek: Addressing Splicing Challenges in Viral Vector Production
A specific hurdle in the development of lentiviral in vivo therapies involves the manufacturing process. In this context, a lentiviral vector is used to introduce a genetic payload into a host cell, enabling that cell to target a second host cell type. During the replication of lentiviruses in manufacturing, the genetic payload can occasionally be truncated, or "spliced," resulting in an incomplete genetic message. This splicing can lead to the vector expressing the gene and subsequently transfecting the incorrect cell type. To circumvent this critical issue, Lentitek has developed an innovative genetic element designed to prevent splicing during lentiviral vector production, ensuring the integrity and targeted delivery of the therapeutic payload.
Technical Hurdles Driving Supplier-Side Innovation
The path to widespread adoption of in vivo cell therapies is paved with significant technical challenges. David Peritt identifies three primary obstacles: dosing accuracy, given the difficulty in directly controlling the number of circulating modified cells; off-target effects, where delivery vectors may inadvertently target unintended cells; and immunogenicity, where the patient’s immune system may react against the vectors.
Different vector systems offer distinct solutions to these challenges, according to Zocco. Viral vectors, such as lentiviruses, offer the advantage of durable gene integration into host cells. However, they carry the risk of introducing potentially oncogenic genetic changes and are also susceptible to triggering an immune response. In contrast, Lipid Nanoparticles (LNPs) facilitate the transient expression of mRNA payloads. While less enduring than lentiviral integration, LNPs provide greater control and are generally easier to manufacture. Nevertheless, LNPs can also elicit an immune response and are known to exhibit a predilection for targeting liver cells.
Lupagen: Redefining In Vivo Delivery with an "Ex Vivo" Approach
Lupagen is pioneering a novel approach with its Xynvivo system, which fundamentally alters the administration of in vivo cell therapies. Peritt likens the system to a sophisticated dialysis machine. In this process, a patient’s blood cells are continuously extracted, genetically modified, filtered to remove unbound vectors, and then returned to the patient, all at the bedside in a closed-loop system. This innovative method effectively filters out unbound vectors before the cells are reintroduced, thereby mitigating the risk of immune reactions triggered by these vectors. By performing the transfection outside the patient’s body, the Xynvivo system allows for precise cell-type targeting and meticulous control over dosing. Peritt notes that this approach blurs the traditional lines between in vivo and ex vivo therapies.
Navigating a Unique Logistical Terrain
A primary hope surrounding in vivo therapies is their potential to surmount the formidable logistical complexities that have historically hampered the commercial success of many cell therapies, particularly autologous treatments. The prospect of off-the-shelf in vivo treatments, where the patient effectively serves as the manufacturing facility, could dramatically simplify and reduce the cost associated with delivering these advanced therapies.
However, experts acknowledge that scalability remains a significant limiting factor. Current in vivo technologies are not yet equipped for complex genetic editing. Consequently, these factors suggest that ex vivo treatments will continue to hold a vital place in the therapeutic arsenal, and it is more likely that both modalities will coexist rather than one superseding the other.
Lonza: Consolidating the Supply Chain for Emerging Therapies
The material supply network for in vivo therapies is still in its nascent stages. Zocco points out that the availability of essential components, such as ionizable lipids crucial for creating LNPs with reduced toxicity, is limited to only a handful of suppliers. Furthermore, many cutting-edge materials and technologies necessitate substantial licensing fees. As a CDMO, Lonza plays a critical role in de-risking the commercialization pathway. "As a CDMO, Zocco describes Lonza’s role as, ‘to de-risk the technical path for commercialisation.’" The company provides an established manufacturing infrastructure and assumes licensing costs, thereby offering developers "freedom to operate," according to Zocco.
Team Consulting: Prioritizing "Scaling Out" for Personalized Therapies
The diverse nature of advanced therapies often necessitates highly specialized manufacturing processes, with many personalized treatments requiring bespoke production for each individual patient. This inherent variability poses a challenge for the development of a unified, standardized global supply chain system for in vivo therapies. Team Consulting has focused on strategies to "scale-out" personalized therapy production, as opposed to traditional "scale-up" methods. For example, Kapnisi highlights the company’s support for the design of the NANOme device, developed by German pharmaceutical equipment supplier LEON. This device is engineered to encapsulate genetic payloads in LNPs for single-patient batches, offering a cost-effective solution for small-scale production that is better suited for personalized in vivo applications.
Despite these ongoing challenges, Peritt maintains that in vivo therapies benefit from the foundational work laid by earlier generations of cell therapies. They also offer comparatively simpler manufacturing processes than their ex vivo counterparts. The elimination of costly and sensitive cell handling procedures, coupled with a well-established vector manufacturing infrastructure—a process already perfected for ex vivo cell therapy supply—presents a significant advantage.
Kapnisi believes that expanding production capacity to meet commercial demand is achievable. She advises in vivo developers to learn from the experiences of previous cell therapy endeavors and to prioritize scaling production early in the clinical development phase. "This can be done, but investors need to back these efforts with cash, against their instincts to hold back capital until late-phase readouts," Kapnisi stated, underscoring the need for proactive investment strategies to support the growth of this field.
Cell & Gene Therapy coverage on Pharmaceutical Technology is supported by Cytiva.
Editorial content is independently produced and follows the highest standards of journalistic integrity. Topic sponsors are not involved in the creation of editorial content.











Leave a Reply