A groundbreaking study published in The Lancet Digital Health has unveiled a remarkable neurological phenomenon: the human brain appears to undergo a process of structural "rejuvenation" in undamaged areas following a severe stroke. Researchers at the University of Southern California (USC) Mark and Mary Stevens Neuroimaging and Informatics Institute (Stevens INI) have demonstrated that while a stroke accelerates biological aging in the affected hemisphere, the opposite, undamaged side of the brain may reorganize itself to appear structurally "younger." This paradoxical finding offers a new window into the mechanisms of neuroplasticity and suggests that the brain’s compensatory strategies are far more complex than previously understood.
The research, which utilized advanced artificial intelligence to analyze brain scans from hundreds of stroke survivors across the globe, represents a significant leap forward in understanding how the central nervous system responds to traumatic injury. By identifying these patterns of regional brain aging, scientists believe they are closer to developing personalized rehabilitation protocols that can be tailored to an individual’s unique neurological profile.
The Science of Brain Age and Neuroplasticity
At the heart of the study is the concept of "brain age," a metric that estimates the biological health of brain tissue compared to a person’s chronological age. In healthy individuals, the brain-predicted age difference (brain-PAD) typically remains close to zero. However, neurological conditions, chronic stress, or physical trauma can cause the brain to appear older than its years, a state often associated with cognitive decline and reduced functional capacity.
In the context of stroke, the USC team sought to determine how the brain’s structure shifts during the chronic phase of recovery—the period starting six months after the initial event. Traditionally, stroke research has focused on the site of the lesion (the ipsilesional side). This study, however, shifted its focus to the contralesional hemisphere, the side of the brain that remained physically untouched by the stroke.
The findings indicate that survivors with the most severe motor impairments exhibited the most significant "youthful" structural changes in their undamaged hemispheres. This suggests that the brain is not merely stagnant after an injury; rather, it actively recruits undamaged networks to compensate for the loss of function, effectively rewiring itself in a way that manifests as a more resilient, younger-looking structure in specific regions.
Methodology: Harnessing Global Data and Deep Learning
The scale of the study was made possible through the Enhancing NeuroImaging Genetics through Meta-Analysis (ENIGMA) Stroke Recovery Working Group. ENIGMA is an international consortium that pools neuroimaging data from over 50 countries, allowing researchers to observe patterns that would be statistically invisible in smaller, localized studies.
For this specific analysis, the team examined MRI scans from 532 stroke survivors collected across 34 research centers in eight countries. To process this massive dataset, the researchers employed a graph convolutional network (GCN), a sophisticated type of artificial intelligence capable of analyzing complex structural relationships within the brain.
The AI model was first trained on tens of thousands of MRI scans from healthy individuals to establish a baseline for normal brain aging. Once trained, the system was used to estimate the biological age of 18 specific brain regions in the stroke survivors. By comparing these estimates with the survivors’ actual ages, the researchers could pinpoint exactly where aging was accelerating and where it was seemingly being reversed.
Chronology of Post-Stroke Recovery and Brain Adaptation
The timeline of stroke recovery is generally divided into three phases: the acute phase (the first few days), the subacute phase (weeks to months), and the chronic phase (six months and beyond). This study focused on the chronic phase, a period when many patients find their progress plateaus and traditional rehabilitation becomes less effective.
- Initial Injury (Acute Phase): The stroke causes immediate cell death and disrupts neural pathways in one hemisphere.
- Early Adaptation (Subacute Phase): The brain begins to clear debris and reduce inflammation. Patients often see the most rapid improvements in motor function during this time.
- Long-Term Reorganization (Chronic Phase): This is where the USC study finds its most compelling data. Even after the initial window of rapid recovery has closed, the brain continues to adapt. In patients with severe, persistent motor deficits, the contralesional frontoparietal network—responsible for planning, coordination, and attention—begins to show the "youthful" structural signature identified by the AI.
This chronology suggests that the brain’s attempt to rejuvenate itself is a long-term response to sustained disability, a desperate but sophisticated effort to find new ways to process motor signals when the primary pathways are permanently destroyed.
Key Findings and Supporting Data
The data revealed a clear correlation between the severity of physical impairment and the degree of contralesional "rejuvenation." Patients were evaluated using standard motor function scores, which measure their ability to move their limbs and perform daily tasks.
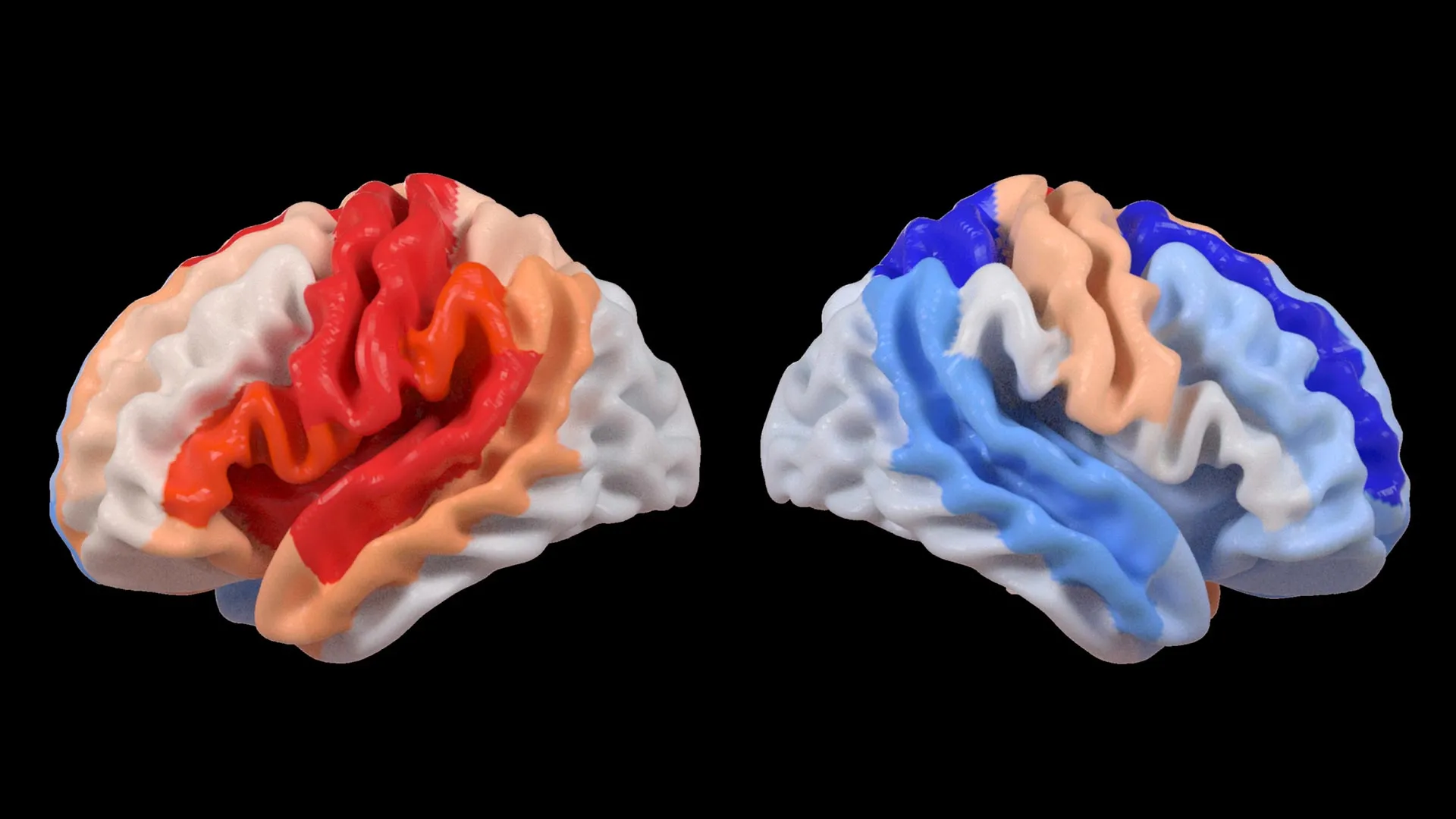
- Ipsilesional Hemisphere: In almost all cases, the hemisphere where the stroke occurred showed signs of accelerated aging. The larger the stroke, the older the tissue appeared compared to the patient’s chronological age.
- Contralesional Hemisphere: Paradoxically, in survivors with severe movement loss, the opposite side of the brain appeared significantly younger.
- The Frontoparietal Network: This specific network showed the strongest "youthful" trend. Because this area is critical for motor planning and executive function, its structural change is viewed as a compensatory mechanism.
Dr. Hosung Kim, associate professor of research neurology at the Keck School of Medicine of USC and co-senior author, noted that this pattern is a form of structural neuroplasticity. "This pattern suggests the brain may be reorganizing itself, essentially rejuvenating undamaged networks to compensate for lost function," Kim explained. He emphasized that this "youthful" appearance does not necessarily mean the patient has regained full movement, but rather that the brain has fundamentally changed its architecture to manage the impairment.
Perspectives from the Scientific Community
The study has been met with significant interest from the global neurology community. Researchers not involved in the study suggest that these findings validate long-held theories about the "vicariation" of function—the idea that one part of the brain can take over the duties of another.
Arthur W. Toga, PhD, director of the Stevens INI and a leading figure in neuroimaging, highlighted the importance of the technology used. "By pooling data from hundreds of stroke survivors worldwide and applying cutting-edge AI, we can detect subtle patterns of brain reorganization that would be invisible in smaller studies," Toga said. He added that these "regionally differential" aging patterns are a crucial step toward moving away from a one-size-fits-all approach to stroke recovery.
Logically inferred reactions from the clinical community suggest that this data could revolutionize how physical therapists approach chronic patients. If a scan reveals that a patient’s frontoparietal network is undergoing significant reorganization, therapists might prioritize cognitive-motor tasks that leverage that specific network, rather than focusing solely on repetitive limb movements that rely on damaged pathways.
Implications for the Future of Personalized Medicine
The broader implications of this research extend into the realm of precision medicine. Currently, stroke rehabilitation is often a trial-and-error process. Some patients respond well to robotic-assisted therapy, while others benefit more from constraint-induced movement therapy.
By using AI to map a patient’s "brain age profile," doctors could theoretically predict which patients have the highest potential for neuroplasticity and tailor their treatments accordingly. For instance:
- Patients with high contralesional rejuvenation might be candidates for advanced brain-computer interfaces (BCIs) that bypass damaged areas and tap directly into the "younger," more adaptable networks.
- Patients with accelerated aging in both hemispheres might require different interventions, perhaps focusing on neuroprotective drugs or lifestyle changes to slow further degradation before intensive physical therapy begins.
The USC Stevens INI team plans to expand their research by following patients longitudinally. By tracking how these brain age patterns change from the moment of the stroke through years of recovery, they hope to identify the exact window when the brain is most "plastic" and receptive to intervention.
Conclusion and Global Impact
The study, funded by the National Institutes of Health (NIH) grant R01 NS115845, was a massive collaborative effort involving institutions such as the University of British Columbia, Monash University, Emory University, and the University of Oslo. It underscores the power of big data in modern medicine.
As stroke remains a leading cause of disability worldwide, affecting millions of families and placing a multi-billion-dollar burden on healthcare systems, the discovery of contralesional rejuvenation provides a much-needed beacon of hope. It proves that the brain’s capacity for change persists even in the face of severe damage. While the journey from a "younger" brain structure to restored physical movement is complex, scientists now have a clearer map of the territory, guided by the objective and precise lens of artificial intelligence.
The findings published in The Lancet Digital Health serve as a reminder that the human body possesses internal mechanisms for resilience that science is only beginning to decode. Through the integration of global data and advanced machine learning, the medical community is moving toward a future where "brain age" is as common a metric as blood pressure, providing a vital tool in the quest to help stroke survivors reclaim their independence.








Leave a Reply