The rapid ascent of Medvi, a telehealth company projected to achieve a staggering $1.8 billion valuation this year, has thrust a critical spotlight onto the evolving landscape of digital healthcare, artificial intelligence, and regulatory oversight. Hailed by some, including a recent New York Times profile in April 2026, as a testament to the power of AI to enable solo entrepreneurs to build massive enterprises, Medvi’s success story is simultaneously intertwined with significant regulatory challenges, including an FDA warning letter for misbranding and prior investigations into its use of AI-generated deceptive content. This dichotomy underscores a growing tension between innovative, fast-moving digital health models and the slower, often fragmented mechanisms designed to protect public health and consumer trust.
Medvi’s business model is particularly noteworthy for its strategic exploitation of regulatory ambiguities. It operates not as a traditional drug manufacturer, pharmacy, or direct healthcare provider, but rather as a sophisticated customer acquisition engine. The company famously owns no pharmacies, directly employs no physicians, and holds no drug licenses. Instead, all clinical and pharmaceutical functions are outsourced to a network of partners, including CareValidate, OpenLoop Health, Beluga Health, and Belmar Pharma Solutions. This architecture effectively externalizes the primary regulatory burden, allowing Medvi to thrive in a legal gray area that has become increasingly lucrative, particularly in the booming market for metabolic drugs like those based on GLP-1 agonists such as tirzepatide (Eli Lilly’s Mounjaro/Zepbound) and semaglutide (Novo Nordisk’s Ozempic/Wegovy).
The story of Medvi is not just about a single company; it is a microcosm of a broader industry-wide challenge where rapid technological advancement, particularly in AI and telehealth, is outpacing the legislative and enforcement capabilities of existing regulatory frameworks. The consequences of this disconnect are profound, raising serious questions about patient safety, ethical marketing practices, and the very future of healthcare governance in the digital age.
The GLP-1 Gold Rush and the Compounding Conundrum
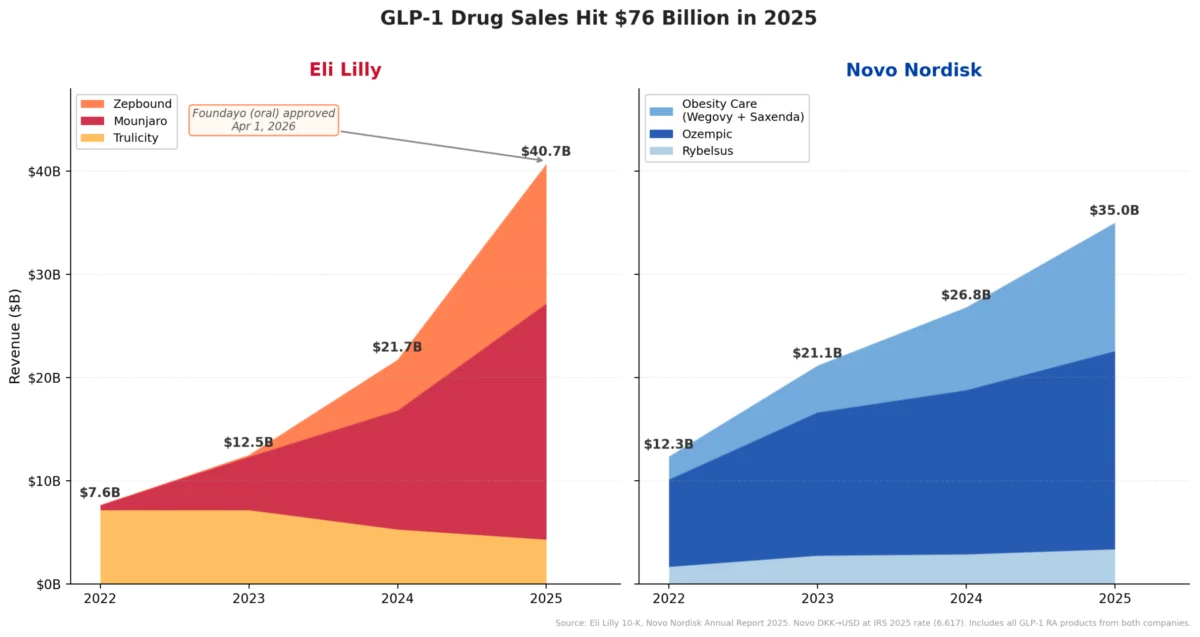
The foundation of Medvi’s rapid growth is deeply rooted in the unprecedented demand for GLP-1 agonist drugs, which have revolutionized weight management and diabetes treatment. Semaglutide, marketed as Ozempic for diabetes and Wegovy for weight loss, along with tirzepatide, marketed as Mounjaro for diabetes and Zepbound for weight loss, have become household names due to their remarkable efficacy. This surging demand, however, quickly outstripped supply, leading to critical shortages that inadvertently opened a significant regulatory loophole.
Under specific FDA rules, during a declared drug shortage, compounding pharmacies are permitted to produce copies of branded drugs to ensure patient access. This provision, intended as a temporary measure to alleviate critical supply gaps, became a gateway for numerous companies to enter the lucrative market for GLP-1s. The FDA officially declared a shortage of Wegovy in March 2022, followed by Ozempic in August 2022. This declaration enabled compounding pharmacies to legally create and distribute compounded versions of semaglutide, often at a lower cost and without undergoing the rigorous standard approval processes mandated for branded pharmaceuticals.
However, these compounded drugs are not identical to their branded counterparts and carry inherent risks. They are not FDA-approved, meaning they have not undergone the same stringent testing for safety, efficacy, and quality. Novo Nordisk, the manufacturer of Ozempic and Wegovy, conducted its own analysis, revealing that injectable semaglutide obtained from some compounding pharmacies contained alarming levels of impurities, in some cases up to 86%. Such high levels of impurities raise serious concerns about potential adverse effects, unpredictable potency, and overall patient safety. Despite these documented risks, the lower cost and easier access offered by compounded versions made them highly attractive to a public desperate for these life-changing medications. The global market for GLP-1 drugs is projected to exceed $100 billion by the early 2030s, making it an incredibly tempting arena for both legitimate and less scrupulous players.
The regulatory landscape shifted again in February 2025, when the FDA officially declared the semaglutide shortage resolved. This resolution meant the temporary rule allowing compounded versions was set to expire, with compounding pharmacies instructed to cease production by April 22, 2025. This deadline created a scramble within the industry, with companies like Hims & Hers, another prominent telehealth provider, facing direct legal challenges. In February 2026, Novo Nordisk sued Hims & Hers for patent infringement after it allegedly failed to fully wind down its compounded semaglutide business and attempted to sell a compounded version of Novo’s newly approved Wegovy pill. While that particular lawsuit was later dismissed without prejudice following a distribution agreement between the two companies, it highlighted the aggressive stance pharmaceutical giants were taking against unauthorized compounded versions.
Medvi, however, artfully navigated these treacherous waters. By design, Medvi is not the compounder itself; it merely acts as an intermediary, partnering with licensed compounding pharmacies like Belmar Pharma Solutions and Beluga Health. This strategic distance from the direct act of drug production or compounding insulates Medvi from many of the direct liabilities that its partners or competitors might face. Legally, Medvi positions itself closer to a marketing and technology company, making it exceptionally difficult to hold it directly accountable for issues pertaining to drug manufacturing or patent infringement. This innovative, albeit controversial, business architecture demonstrates a sophisticated understanding of regulatory loopholes and liability frameworks.
A Chronology of Scrutiny and Success
Medvi’s journey to its projected $1.8 billion valuation is marked by a parallel timeline of rapid expansion and increasing regulatory and journalistic scrutiny, highlighting the speed at which digital health can evolve compared to traditional oversight:

- March 2022: The FDA declares a shortage of Wegovy (semaglutide), a key GLP-1 agonist, opening the door for compounded alternatives to ensure patient access.
- August 2022: The FDA extends the shortage declaration to include Ozempic (semaglutide), further fueling the market for compounded semaglutide. This period sees a significant proliferation of telehealth companies offering compounded versions.
- February 2025: The FDA announces the official resolution of the semaglutide shortage, signaling the impending end of the temporary allowance for compounded versions. This move aims to return the market to branded, FDA-approved drugs.
- April 22, 2025: Compounding pharmacies are legally mandated to cease production of semaglutide copies, closing the temporary loophole.
- May 2025: Futurism, an online publication focused on science and technology, publishes a critical article investigating Medvi’s extensive use of AI-generated content. The exposé details the company’s deployment of sophisticated AI to create misleading advertising, including fake patient testimonials, fabricated "before and after" photos, and even AI-generated doctor endorsements, raising serious ethical questions about its marketing practices and the potential for consumer deception.
- February 2026 (approximately six weeks prior to the NYT profile): The U.S. Food and Drug Administration (FDA) issues a formal warning letter to Medvi. The letter specifically cites misbranding violations, accusing Medvi of falsely implying it was directly involved in the compounding process and making claims that suggested FDA approval for its compounded products, which are, by definition, not FDA-approved. This signals the FDA’s concern over consumer confusion and potential safety risks.
- February 2026: Pharmaceutical giant Novo Nordisk initiates a lawsuit against competitor telehealth platform Hims & Hers for alleged patent infringement related to its continued sale of compounded semaglutide. This action underscores the rising legal pressure on companies operating in this space and highlights the drug manufacturers’ resolve to protect their intellectual property and ensure product integrity.
- April 2026: The New York Times publishes a profile celebrating Medvi’s entrepreneurial success, highlighting its founder’s ability to leverage AI to build a massive telehealth enterprise. This article, appearing shortly after the FDA warning, inadvertently underscored the disconnect between popular perception of innovation and the underlying regulatory challenges and risks.
This timeline reveals a company consistently pushing the boundaries, often navigating a fine line between innovation and regulatory compliance, and thriving despite—or perhaps because of—the inherent ambiguities in the current legal framework. It paints a picture of a digital health sector growing at an exponential rate, with regulatory bodies struggling to keep pace.
The Fragmented Regulatory Landscape: Three Agencies, No Clear Owner
The Medvi case vividly illustrates a fundamental challenge in regulating modern digital health platforms: the current regulatory framework, designed for a more traditional healthcare ecosystem, is ill-equipped to handle entities that seamlessly span multiple domains. When a patient encounters a Medvi ad on social media, fills out an online intake form, receives a prescription for a compounded GLP-1 from an unseen physician, and obtains medication from a distant pharmacy, at least three distinct federal regulatory agencies, alongside relevant state medical boards and potentially the FTC’s digital advertising division, have a stake. Yet, no single entity possesses clear, comprehensive jurisdiction over the entire transaction.
1. The Food and Drug Administration (FDA):
The FDA’s primary mandate is to ensure the safety, efficacy, and security of drugs, as well as medical devices and certain food products. Under the Federal Food, Drug, and Cosmetic Act, it governs whether a compounded drug is legally produced, whether the compounding pharmacy adheres to quality standards, and whether marketing materials misbrand the product. In Medvi’s case, the FDA acted on its mandate by issuing a warning letter in February 2026. This letter specifically cited Medvi for misbranding, highlighting claims that implied Medvi itself was the compounder and that its compounded products were FDA-approved, which they are not. An FDA spokesperson, when reached for comment on such matters, typically states that the agency "does not comment on ongoing compliance matters," reflecting the formal nature of their enforcement process.
Crucially, the FDA’s jurisdiction has significant limitations in this context. It does not regulate telehealth prescribing practices, which fall under state authority. Nor does it broadly regulate digital advertising claims, a domain primarily overseen by the Federal Trade Commission (FTC). Furthermore, the FDA does not directly regulate marketing intermediaries like Medvi, which operate between the consumer and the compounding pharmacy. Medvi’s legal classification as a "marketing and technology company" rather than a drug manufacturer or prescriber effectively shields it from many direct FDA enforcement actions related to the drug itself.
2. State Medical Boards:
The regulation of telehealth prescribing practices is largely decentralized, falling under the purview of individual state medical boards. Each of the 50 states maintains its own standards for establishing a valid patient-physician relationship. A critical question for companies like Medvi, which often rely on asynchronous online intake questionnaires, is whether such an interaction constitutes a sufficient clinical encounter for prescribing medications, particularly high-risk drugs like GLP-1s. The American Medical Association (AMA) and various professional societies have issued guidelines emphasizing the importance of a legitimate patient-physician relationship, often recommending synchronous visits for initial assessments, especially for complex or high-risk conditions.
Some states mandate a synchronous video visit before prescribing controlled substances or high-risk medications, while others permit asynchronous prescribing, where a physician reviews patient information without a real-time interaction. Medvi’s stated operation in 49 states necessitates compliance with a complex web of varying regulations. However, Medvi further distances itself from this regulatory burden by outsourcing prescribing services to partners like OpenLoop Health. This arrangement means that if a prescribing standard is violated, the individual clinician and the outsourcing partner, not Medvi itself, bear the primary legal and professional responsibility.
State medical boards, designed to investigate individual physician conduct, face inherent limitations in addressing systemic platform behavior. While they can discipline individual physicians for inappropriate prescriptions, they lack the legal authority or infrastructure to sanction an entire platform that facilitates thousands of such encounters across state lines. The multi-state nature of telehealth further complicates matters: if a patient in one state receives a prescription from a physician in another, facilitated by a platform based in a third, and fills it at a pharmacy in a fourth, determining which medical board has primary jurisdiction becomes a formidable challenge. This jurisdictional ambiguity is a critical advantage for companies operating in this gray space.
3. The Federal Trade Commission (FTC):
The FTC is the primary federal agency responsible for consumer protection, including policing unfair or deceptive acts or practices in commerce. Section 5 of the FTC Act prohibits such acts, and the FTC’s Health Products Compliance Guidance sets clear standards for health claims in advertising, requiring them to be truthful and substantiated. This mandate gives the FTC authority over the specific issues Futurism identified in Medvi’s practices: AI-generated "before and after" photos, fake patient testimonials, fabricated doctor endorsements, and unsubstantiated claims of clinical efficacy. The FTC has a history of pursuing companies making unsubstantiated health claims, particularly in emerging markets.
However, the FTC’s enforcement mechanisms, typically involving investigations, consent decrees, and civil penalties, are notoriously slow. The process often takes years to unfold









Leave a Reply