A groundbreaking study led by researchers at McGill University and the Douglas Research Centre has fundamentally altered the scientific understanding of Major Depressive Disorder (MDD) by identifying two specific types of brain cells that function abnormally in individuals with the condition. The research, published in the prestigious journal Nature Genetics, utilizes advanced single-cell genomic mapping to pinpoint disruptions in gene activity and DNA regulation. These findings represent a significant leap forward in psychiatric neuroscience, offering a high-resolution map of the biological malfunctions that underpin one of the world’s most prevalent and debilitating mental health conditions. By focusing on the molecular level of individual cells rather than general brain regions, the team has provided a blueprint for the development of next-generation antidepressants that could target the specific cellular drivers of depression.
The study comes at a critical time for global public health. According to the World Health Organization (WHO), depression affects more than 264 million people of all ages and is a leading cause of disability worldwide. Despite its prevalence, current pharmacological treatments—many of which were developed decades ago—often rely on a "one-size-fits-all" approach that focuses on neurotransmitter levels like serotonin and norepinephrine. However, nearly one-third of patients do not respond adequately to these traditional therapies. The McGill study suggests that the lack of efficacy in current treatments may be due to a failure to address the specific cellular and genetic disruptions now identified by Dr. Gustavo Turecki and his colleagues.
The Science of Single-Cell Genomics
To achieve this breakthrough, the research team employed a technique known as single-nucleus chromatin accessibility profiling alongside transcriptomic analysis. Traditional brain research often involves "bulk" sequencing, where a piece of brain tissue is ground up and analyzed as a whole. This method, while useful, masks the diversity of the brain, which contains billions of cells with vastly different functions. By contrast, the McGill team isolated thousands of individual nuclei from post-mortem brain samples, allowing them to see exactly which genes were "turned on" or "off" within specific cell types.
This level of precision allowed the scientists to examine the "epigenetic" landscape of the brain. Epigenetics refers to the mechanisms that regulate the DNA code—effectively the switches that determine how and when a gene is expressed. By mapping these switches in 59 individuals diagnosed with depression and comparing them to 41 healthy controls, the researchers identified distinct patterns of cellular dysfunction that had previously remained invisible to the scientific community.
Identifying the Cellular Culprits: Neurons and Microglia
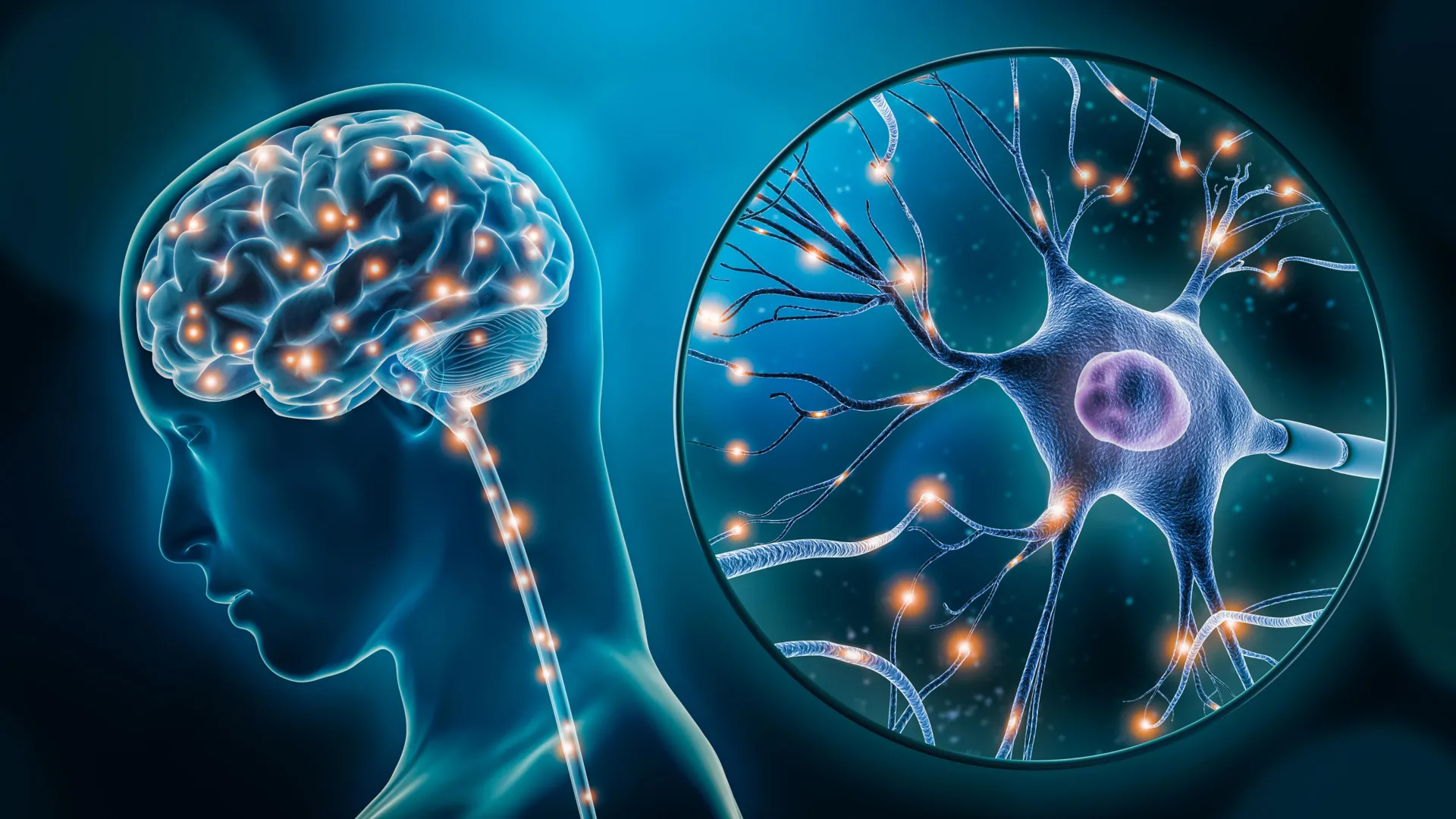
The analysis revealed that the most significant changes occurred in two distinct populations of cells: excitatory neurons and microglia. Each plays a vital role in brain health, and their dysfunction offers a compelling explanation for the complex symptoms of depression.
Excitatory neurons are the primary "communicators" of the brain, responsible for sending signals that stimulate activity in other neurons. The study found that in people with depression, specific groups of these neurons—particularly those located in the prefrontal cortex, a region responsible for mood regulation and executive function—showed altered gene activity. These neurons are heavily involved in the brain’s response to stress. When their genetic programming is disrupted, it can lead to a breakdown in the neural circuits that manage emotional resilience, potentially explaining the persistent low mood and cognitive "fog" often reported by patients.
The second type of cell identified was a subtype of microglia. Microglia are the resident immune cells of the central nervous system. For decades, they were thought to be simple "housekeepers" that cleared away debris. However, modern neuroscience has revealed that microglia are active participants in brain signaling and inflammation. The McGill study found that in the depressed brain, microglia show genetic signatures associated with chronic inflammation. This supports the "inflammatory hypothesis" of depression, which suggests that an overactive immune response in the brain can interfere with normal neuronal function, leading to depressive symptoms.
The Essential Role of the Douglas-Bell Canada Brain Bank
The success of this research was made possible by the Douglas-Bell Canada Brain Bank (DBCBB), one of the most extensive and well-characterized repositories of human brain tissue in the world. Located at the Douglas Research Centre in Montreal, the bank houses over 3,000 brains, many of which were donated by individuals who suffered from various psychiatric disorders.
"This is a rare and invaluable resource," said Dr. Gustavo Turecki, the study’s senior author and a professor at McGill. "To understand a human disorder as complex as depression, we must study the human brain itself. Animal models provide clues, but the Douglas-Bell Canada Brain Bank allows us to look directly at the molecular architecture of the condition in humans."
The use of post-mortem tissue is ethically sensitive but scientifically necessary. By analyzing the brains of individuals who had a documented history of Major Depressive Disorder, the researchers were able to correlate biological findings with clinical realities. The bank’s rigorous protocols for tissue preservation ensured that the delicate RNA and DNA structures remained intact for the advanced genomic sequencing required for the study.
A Chronology of Discovery in Psychiatric Neuroscience
The McGill study is the culmination of decades of progress in both genetics and psychiatry. To understand its significance, it is helpful to view it within the timeline of brain research:
- 1950s-1960s: The discovery of the first antidepressants (MAOIs and TCAs) led to the "Monoamine Hypothesis," suggesting depression is caused by a chemical imbalance of neurotransmitters.
- 1980s: The founding of the Douglas-Bell Canada Brain Bank established a foundation for biological psychiatry in Canada.
- 2003: The completion of the Human Genome Project provided a map of human DNA, though it did not yet explain how genes were regulated in specific tissues.
- 2010s: The development of single-cell sequencing technologies allowed researchers to move beyond "bulk" tissue analysis to look at individual cells.
- 2015-2020: Increased focus on neuroinflammation and the role of the immune system (microglia) in mental health.
- Current Study: The McGill team integrates single-cell genomics with epigenetic mapping to identify the specific cell types (excitatory neurons and microglia) involved in depression.
Broader Implications for Precision Psychiatry
The findings of this study have profound implications for the future of mental health care, specifically in the movement toward "Precision Psychiatry." This field aims to move away from trial-and-error prescribing and toward treatments tailored to a patient’s specific biological profile.
By identifying excitatory neurons and microglia as key players, the research opens the door for the development of "cell-type-specific" therapies. For example, if a patient’s depression is driven primarily by microglial inflammation, they might benefit from a different class of medication than a patient whose condition is rooted in excitatory neuron dysfunction. This could lead to higher success rates for treatments and a reduction in the side effects associated with broad-spectrum psychiatric drugs.
Furthermore, the study provides a powerful rebuttal to the lingering social stigma that views depression as a purely psychological or "emotional" failing. By demonstrating measurable, physical changes in the DNA regulation of specific brain cells, the research reinforces the fact that depression is a biological brain disorder, no different in its physical reality than cardiovascular disease or diabetes.
Expert Reactions and Institutional Support
The scientific community has reacted with optimism to the publication. While not directly involved in the study, independent neuroscientists have noted that the integration of chromatin accessibility with RNA sequencing provides a "double-check" on the data, making the findings particularly robust. The identification of specific functional variants—the "switches" that go wrong—provides pharmaceutical companies with clear targets for drug screening.
The research was a collaborative effort involving several prominent institutions and funding bodies. Support was provided by the Canadian Institutes of Health Research (CIHR), the Brain Canada Foundation, the Fonds de recherche du Québec – Santé (FRQS), and the Healthy Brains, Healthy Lives (HBHL) initiative at McGill University. These organizations have emphasized that long-term investment in basic science and bio-banking is essential for breakthroughs in complex diseases like depression.
Dr. Turecki, who also serves as the Canada Research Chair in Major Depressive Disorder and Suicide, emphasized that while the results are a major milestone, they are also a beginning. "We have the ‘who’ and the ‘where’—we know which cells are involved and where the disruptions are happening. The next step is the ‘how’ and the ‘what.’ We need to understand how these genetic changes translate into the symptoms patients experience and what we can do to reverse those changes."
Looking Ahead: The Future of Depression Research
The McGill team plans to expand their research to look at other brain regions and to determine if these cellular changes are present in other psychiatric conditions, such as bipolar disorder or schizophrenia. There is also a significant interest in determining whether current treatments, such as Ketamine or Transcranial Magnetic Stimulation (TMS), exert their effects by correcting the specific cellular disruptions identified in this study.
As the global burden of mental health continues to rise, the transition from broad observations to cellular-level precision marks a turning point. For the millions of people living with depression, the work of Dr. Turecki and his team offers more than just scientific data; it offers the promise of a future where mental health treatment is as precise and effective as any other branch of modern medicine. The discovery that depression is etched into the very regulation of our brain cells is a sobering reminder of the condition’s complexity, but it is also the clearest map yet for how to find a way out.








Leave a Reply