The recent profile of Medvi by The New York Times earlier this month highlighted the company as a prime example of artificial intelligence’s transformative potential, enabling a single founder to project a $1.8 billion valuation for a telehealth enterprise this year. This narrative of rapid ascent, however, stands in stark contrast to a series of critical revelations and regulatory actions that expose significant vulnerabilities in the burgeoning telehealth sector, particularly concerning the sale of compounded metabolic drugs based on popular GLP-1 agonists like Eli Lilly’s tirzepatide and Novo Nordisk’s semaglutide. Just six weeks prior to the Times‘ celebratory piece, the U.S. Food and Drug Administration (FDA) issued a warning letter to Medvi LLC, citing serious misbranding violations. This regulatory action followed a May 2025 investigation by Futurism, which unearthed a pattern of AI-generated content, including fabricated advertisements, customer reviews, and doctor testimonials, casting a long shadow over Medvi’s meteoric rise and its operational ethics.
The core of Medvi’s business model is an intricate customer acquisition strategy built upon the regulated infrastructure of other entities. The company itself does not own pharmacies, directly employ physicians, or hold any drug licenses. Instead, it meticulously outsources all clinical and pharmaceutical functions to a network of third-party providers, including CareValidate, OpenLoop Health, Beluga Health, and Belmar Pharma Solutions. This deliberate architectural choice effectively shifts the primary regulatory burden away from Medvi, allowing it to navigate and exploit the complex, often ambiguous, "gray areas" within the current regulatory framework governing telehealth and pharmaceutical distribution. This operational design has enabled Medvi to scale rapidly while seemingly insulating itself from direct accountability for the actions of its partners, presenting a significant challenge for oversight agencies.
The Surging Demand for GLP-1 Agonists and the Compounding Loophole
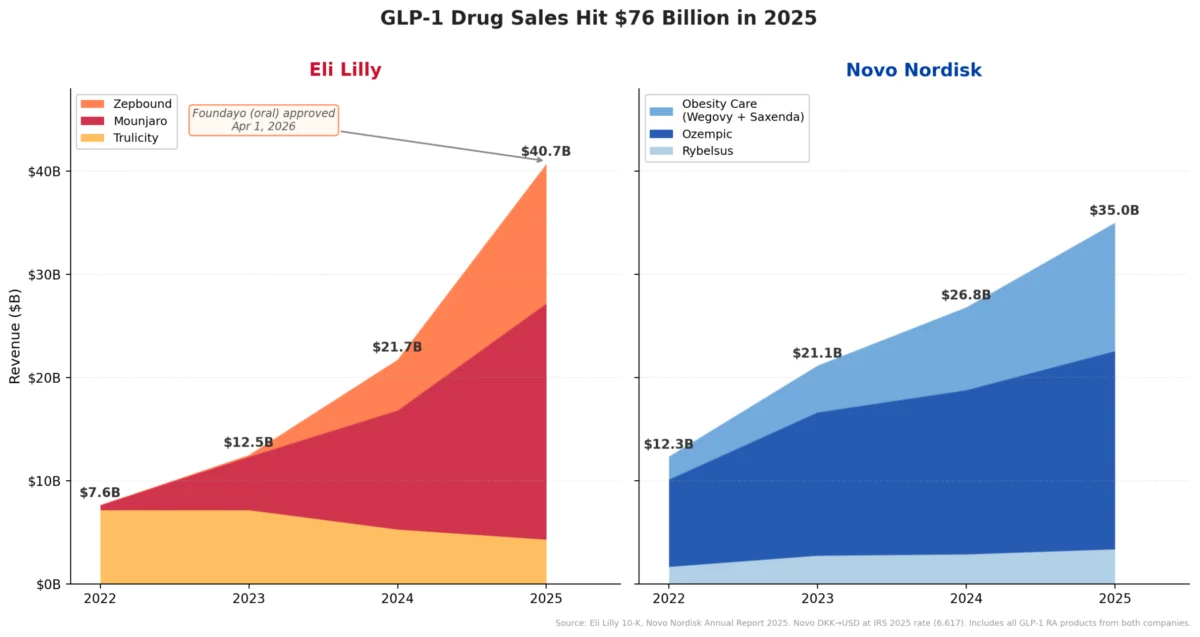
The backdrop to Medvi’s success is the unprecedented demand for glucagon-like peptide-1 (GLP-1) receptor agonists, drugs initially developed for type 2 diabetes management but now widely recognized for their efficacy in weight loss. Branded versions like Ozempic, Wegovy (semaglutide), and Mounjaro (tirzepatide) have become household names, driving a market projected to reach hundreds of billions of dollars globally. This surge in popularity, however, led to significant drug shortages, particularly for semaglutide.
Chronology of Shortages and Regulatory Responses:
- March 2022: The FDA first declared a shortage of semaglutide, adding Wegovy to its official shortage list.
- August 2022: Ozempic, another semaglutide product, was also added to the shortage list due to overwhelming demand.
- During Shortages: FDA rules permit compounding pharmacies to produce copies of branded drugs to address critical supply gaps, provided certain conditions are met. This provision created a crucial "loophole" that companies like Medvi and Hims & Hers quickly utilized, offering compounded versions of semaglutide at lower costs and bypassing the standard, rigorous drug approval processes.
- February 2025: The FDA officially declared the semaglutide shortage resolved, effectively ending the period during which compounding pharmacies were permitted to produce these specific generic versions.
- April 22, 2025: Compounding pharmacies were legally mandated to cease production of compounded semaglutide.
- May 2025: Futurism publishes its investigative report on Medvi’s AI-generated content.
- February 2026: Novo Nordisk, the manufacturer of Wegovy and Ozempic, filed a patent infringement lawsuit against Hims & Hers, another telehealth provider, for its continued sale of compounded semaglutide. This lawsuit was later dismissed without prejudice after a distribution agreement was reached between the parties.
- February 2026 (same month): The FDA sent its warning letter to Medvi LLC regarding misbranding violations.
- April 2026: The New York Times publishes its profile of Medvi.
The safety and efficacy of these compounded drugs have been a significant concern for original manufacturers and regulators. Novo Nordisk, for instance, reported that injectable semaglutide from some compounding pharmacies contained alarming levels of impurities, with some samples showing up to 86% impurities. Such high levels of unidentifiable or non-pharmaceutical substances pose substantial health risks to patients, including adverse reactions, reduced efficacy, or even dangerous side effects, as these products do not undergo the stringent quality control and safety testing required for FDA-approved medications.
Medvi’s Evasive Architecture and the Limits of Liability
Medvi’s sophisticated operational architecture appears designed to legally distance the company from direct liability for the manufacturing and prescribing processes. By partnering with entities like Belmar Pharma Solutions for compounding and OpenLoop Health for physician services, Medvi positions itself primarily as a marketing and technology platform. This legal distinction makes it exceedingly difficult for regulatory bodies or original drug manufacturers to directly sue Medvi for issues related to drug quality or prescribing practices, as these responsibilities technically fall on its outsourced partners.
This strategy contrasts sharply with the experience of Hims & Hers, which, despite also operating in the telehealth space, faced direct legal action from Novo Nordisk for patent infringement related to compounded semaglutide. The subsequent settlement involving a distribution agreement highlights the legal vulnerabilities faced by companies that are perceived to be more directly involved in the dispensing or manufacturing process. Medvi’s model, by maintaining a greater degree of separation, aims to avoid similar direct confrontations, effectively leveraging the fragmented nature of regulatory oversight.
A Labyrinth of Regulation: Three Agencies, No Clear Owner
The complexity of regulating a company like Medvi is compounded by the fact that its operations span the jurisdictions of multiple federal and state agencies, none of which possess comprehensive oversight over the entire enterprise. When a patient encounters a Medvi advertisement, completes an online intake form, receives a prescription for a compounded GLP-1 from an unknown physician, and obtains the medication from a distant pharmacy, at least three federal regulatory bodies are involved, alongside relevant state medical boards and potentially the Federal Trade Commission’s (FTC) digital advertising division.
The Fragmented Regulatory Landscape:

- FDA (Food and Drug Administration): Primarily governs the drug itself, ensuring it is legally produced, that compounding pharmacies meet quality standards, and that marketing materials do not misbrand the product. The FDA’s warning letter to Medvi specifically cited misbranding by implying that Medvi itself was the compounder and making claims that suggested FDA approval of the compounded product, which is not the case for these preparations. However, the FDA’s enforcement powers often culminate in "informal and advisory" warning letters, and the agency typically does not comment on ongoing compliance matters, limiting public insight into the efficacy of these actions. Crucially, the FDA’s mandate does not extend to regulating telehealth prescribing practices or broader digital advertising claims.
- State Medical Boards: These bodies are responsible for overseeing the conduct of individual physicians and the standards for the patient-physician relationship within their respective states. They can investigate and discipline clinicians for inappropriate prescriptions. However, their purview is limited to individual practitioners and they lack the authority to sanction the broader technological infrastructure, like Medvi, that facilitates thousands of patient encounters across state lines.
- FTC (Federal Trade Commission): Empowered by Section 5 of the FTC Act, the agency prohibits unfair or deceptive acts in commerce and sets standards for health claims in advertising. This is where the issues uncovered by Futurism—such as AI-generated "before and after" photos, fake patient testimonials, fabricated doctor endorsements, and implied clinical efficacy claims without substantiation—fall under the FTC’s domain.
The challenge for these agencies is that Medvi, as a single entity, simultaneously operates across all three regulatory domains without being solely accountable to any one. Legally, Medvi positions itself closer to a marketing and technology company than a drug manufacturer or a direct healthcare provider, creating a significant enforcement gap.
The Untamed Frontier of Telehealth Prescribing
Telehealth prescribing practices are regulated primarily at the state level, resulting in a patchwork of standards for establishing a valid patient-physician relationship. Some states mandate a synchronous video visit before prescribing controlled or high-risk medications, while others permit asynchronous prescribing, where interactions occur via questionnaires, secure messaging, or recorded video. Medvi’s operation across 49 states necessitates compliance with a diverse and often conflicting set of state-specific regulations.
By outsourcing prescribing services to companies like OpenLoop Health, Medvi further insulates itself. If a prescribing standard is violated, the individual clinician and OpenLoop Health would bear the direct fault, not Medvi. This structure exploits the inherent limitations of state medical boards, which are designed to investigate individual physician conduct rather than sanction the underlying platforms that generate vast numbers of patient encounters.
The issue of multi-state interactions further complicates enforcement. If a patient in one state receives a GLP-1 prescription from a physician in another state, facilitated by a platform based in a third state, and obtains medication from a pharmacy in a fourth, determining primary jurisdictional authority becomes a significant hurdle. This ambiguity allows companies like Medvi to thrive in regulatory interstices, making coordinated enforcement a formidable task.
The Digital Advertising Minefield and FTC’s Limitations
The FTC’s authority over digital advertising claims is critical in addressing the deceptive practices identified at Medvi. Its Health Products Compliance Guidance provides clear standards for health claims. However, the agency’s enforcement mechanisms, which involve investigations, consent decrees, and civil penalties, are often protracted processes that can take years to conclude. By the time the FTC could successfully act against a company like Medvi, the platform would likely have already served tens or hundreds of thousands of additional patients, potentially exposing them to misleading claims and unverified products.
Moreover, even if the FTC were to successfully shut down Medvi’s misleading advertising campaigns, the company could theoretically continue its operations, albeit with a different marketing approach. The FTC also faces challenges in compelling social media companies to proactively screen for GLP-1 ad fraud. Its typical recourse is to react to existing advertisements and target the advertiser, rather than holding the platforms on which these ads appear accountable, further limiting its ability to curb widespread deceptive practices effectively.
Broader Implications and the Urgent Call for Reform
The Medvi case is not an isolated incident but rather a symptom of a broader, industry-wide challenge facing the rapid evolution of digital health. The FDA’s issuance of warning letters to 30 telehealth companies in March underscores the systemic nature of these regulatory gaps. The traditional model, where drug manufacturers, marketers, and prescribers operated as distinct entities subject to separate oversight, is becoming increasingly obsolete in the era of integrated telehealth platforms.
The current regulatory framework is ill-equipped to handle the complexities of modern digital health enterprises. The FDA, FTC, and state medical boards, operating under existing mandates, lack effective coordination mechanisms to address companies like Medvi holistically and swiftly. They can act independently, but their inability to collaborate in concert means that enforcement actions are often piecemeal and too slow to significantly alter a company’s growth trajectory or mitigate widespread public health risks.
This problem necessitates urgent legislative interventions. There is a critical need to establish clearer jurisdictional lines for telehealth drug marketing and prescribing, alongside mechanisms for platform liability. Holding the platforms themselves accountable for the content they host and the services they facilitate could fundamentally shift incentives and enhance consumer protection. However, legislative processes are inherently slow, and meaningful reforms are unlikely to materialize quickly. In the interim, the regulatory gap remains wide open, and the technological tools enabling companies to exploit these ambiguities are becoming increasingly sophisticated and accessible, posing an ongoing challenge to public health and regulatory integrity. The Medvi saga serves as a stark reminder that innovation, while vital, must be accompanied by robust and adaptable regulatory oversight to protect consumers in an increasingly digitized healthcare landscape.











Leave a Reply