The landscape of neurodegenerative diagnostics is undergoing a fundamental shift as researchers move beyond simple protein quantification to investigate the complex physical geometry of molecules within the human bloodstream. In a landmark study published in the journal Nature Aging on February 27, 2026, a team of scientists at Scripps Research unveiled a novel diagnostic approach that identifies Alzheimer’s disease not by the amount of specific proteins present in the blood, but by their structural integrity and folding patterns. This breakthrough addresses a critical limitation in current diagnostic frameworks, potentially offering a more sensitive window into the earliest biological deviations that precede cognitive decline.
Currently, the Alzheimer’s Association estimates that approximately 7.2 million Americans aged 65 and older are living with the disease, a figure projected to rise significantly as the "baby boomer" generation continues to age. Traditional diagnostic methods have long focused on the accumulation of amyloid beta (Aβ) and phosphorylated tau (p-tau) proteins. While blood tests for these biomarkers have become increasingly sophisticated over the last five years, they essentially act as a "census," counting the concentration of these proteins in blood or cerebrospinal fluid. However, many researchers argue that concentration levels may only fluctuate after significant pathology has already taken hold in the brain. The Scripps Research team, led by senior author and professor John Yates, suggests that the physical "misfolding" of proteins—a process known as the breakdown of proteostasis—may serve as a much earlier and more accurate harbinger of neurological decay.
The Science of Proteostasis and Protein Folding
To understand the significance of this shift, one must look at the biological concept of proteostasis. Within a healthy organism, proteostasis acts as a rigorous quality-control system, ensuring that proteins are folded into the precise three-dimensional shapes required for them to function. When proteins are produced, they must fold correctly to interact with other molecules; if they misfold, they can become toxic or lose their utility. As the human body ages, the cellular machinery responsible for this folding and for the disposal of "damaged" proteins begins to falter.
In Alzheimer’s disease, this failure has historically been observed in the brain in the form of amyloid plaques and tau tangles. The Scripps team hypothesized that this proteostatic collapse is not localized solely within the central nervous system. Instead, they proposed that the systemic nature of the disease means that structural changes in proteins should be detectable in the peripheral blood long before clinical symptoms like memory loss become undeniable. By focusing on the "shape" of the proteins rather than their "count," the researchers aimed to capture the functional state of the body’s protein-management system.
Methodology: Mass Spectrometry and Machine Learning
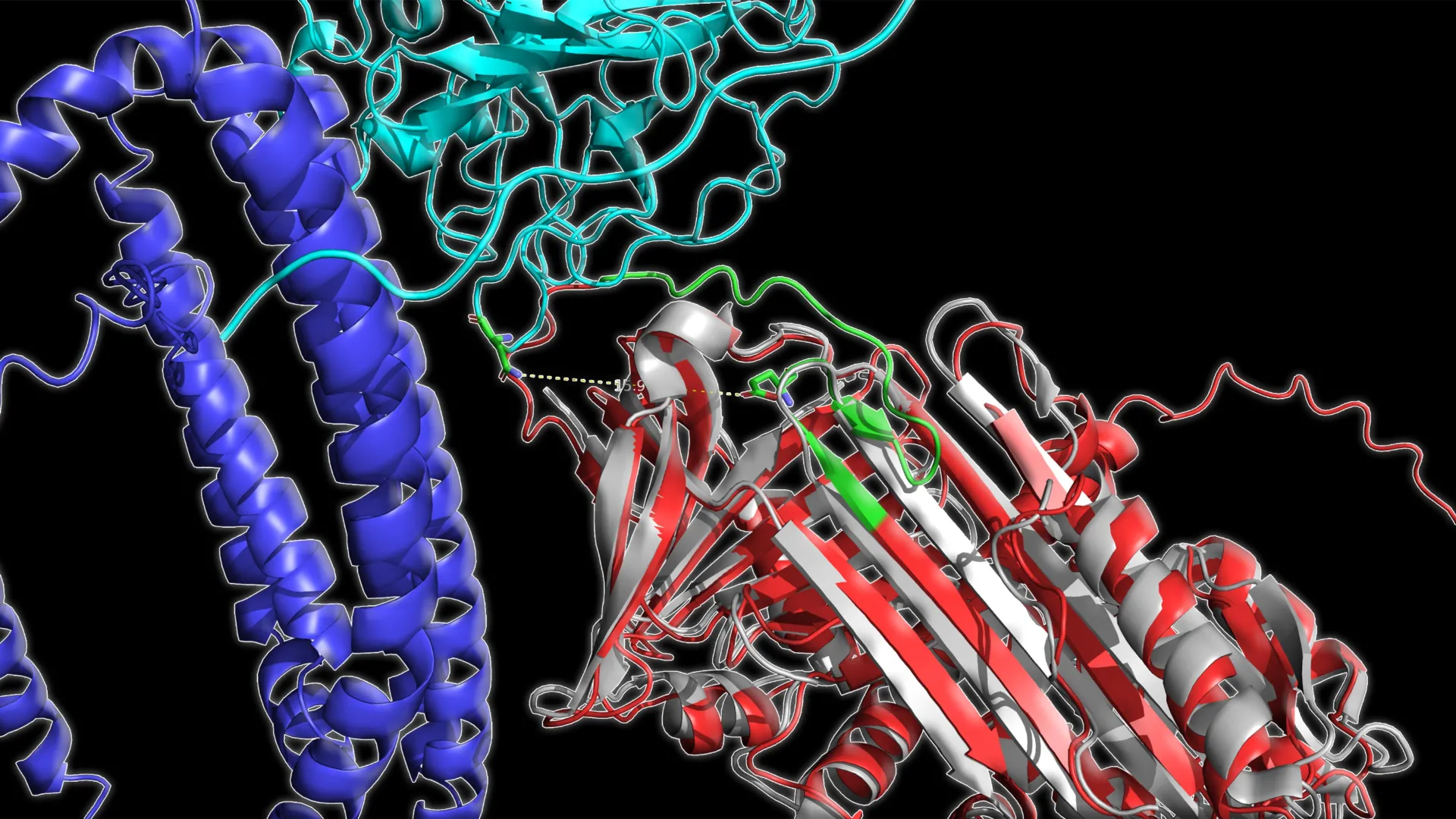
The study involved a rigorous analysis of plasma samples from a cohort of 520 participants. This group was strategically divided into three categories: individuals who were cognitively normal, those diagnosed with mild cognitive impairment (MCI), and patients with confirmed Alzheimer’s disease. To analyze these samples, the researchers utilized advanced mass spectrometry. Unlike standard assays that measure protein volume, this technique allowed the team to map the topography of the proteins. Specifically, they measured how "exposed" or "buried" certain amino acid sites—specifically lysine sites—were within the protein’s architecture.
When a protein misfolds or changes its shape, certain parts of its structure that were once tucked away inside may become exposed to the surface, or vice versa. By identifying these "structural signatures," the researchers created a digital map of the protein’s physical state. They then applied machine learning algorithms to process this vast amount of structural data, searching for patterns that could distinguish a healthy brain from one in the early or late stages of neurodegeneration.
The results revealed a consistent trend: as Alzheimer’s progressed, specific proteins became structurally "closed" or less "open." This structural tightening served as a more reliable indicator of disease than the actual amount of the protein circulating in the system.
Identification of Three Critical Protein Markers
While the researchers examined hundreds of proteins, three specific plasma proteins emerged as the most powerful predictors of Alzheimer’s status. Each of these proteins plays a distinct role in human physiology, and their structural deformation provides a multifaceted view of the disease’s progression:
- C1QA (Complement Component 1, q subcomponent, A chain): This protein is a foundational element of the immune system’s complement pathway, which helps clear pathogens and cellular debris. Structural changes in C1QA suggest that the body’s innate immune response is being altered or "exhausted" by the ongoing neurodegenerative process.
- Clusterin: Often referred to as a "molecular chaperone," clusterin is directly involved in the folding of other proteins and the clearance of amyloid beta from the brain. Its structural degradation is a direct reflection of the failure of the proteostasis system.
- Apolipoprotein B (ApoB): Primarily known for its role in transporting fats and cholesterol through the bloodstream, ApoB is essential for vascular health. Its inclusion in the diagnostic panel highlights the growing understanding of the link between cardiovascular integrity and the health of the blood-brain barrier.
"The correlation was amazing," noted co-author Casimir Bamberger, a senior scientist at Scripps Research. "It was very surprising to find three lysine sites on three different proteins that correlate so highly with disease state." By focusing on these specific sites, the team achieved an overall diagnostic accuracy of 83%. Most notably, when the test was used to distinguish between healthy individuals and those with MCI—the "yellow light" phase of the disease—the accuracy surged to over 93%.
Longitudinal Reliability and Clinical Correlation
One of the most significant hurdles for any new biomarker is longitudinal stability—the ability of the test to remain accurate over time and across different populations. The Scripps team addressed this by testing their three-protein model against independent groups and conducting repeat tests on the same participants several months apart.
In these follow-up sessions, the protein-folding panel maintained an 86% accuracy rate. Furthermore, the "structural score" generated by the test showed a high degree of correlation with established cognitive assessments, such as the Mini-Mental State Examination (MMSE). The researchers also compared their findings with MRI data, finding a moderate but significant association between the protein-folding scores and physical brain shrinkage (atrophy). This suggests that the blood test is not just a chemical snapshot but a reflection of the actual physical state of the patient’s brain.
Implications for Early Intervention and Drug Development
The potential clinical implications of this structural blood test are profound. Currently, the "gold standard" for Alzheimer’s diagnosis involves Amyloid-PET scans or lumbar punctures to collect cerebrospinal fluid. PET scans can cost upwards of $5,000 and are not always covered by insurance, while lumbar punctures are invasive and often avoided by patients. A blood test that measures protein folding could be administered in a standard primary care setting, making screening more accessible to the general population.
"Detecting markers of Alzheimer’s early is absolutely critical to developing effective therapeutics," said John Yates. The medical community is currently witnessing the arrival of the first generation of disease-modifying therapies, such as lecanemab and donanemab. These drugs are most effective when administered in the earliest stages of the disease, before irreversible neuronal loss has occurred. A high-accuracy structural blood test could serve as a "triage" tool, identifying patients who should be prioritized for these advanced treatments.
Furthermore, this method could revolutionize clinical trials for new drugs. By monitoring the "refolding" or stabilization of these proteins, researchers could obtain real-time data on whether a trial medication is successfully restoring proteostasis in the patient.
Future Research and Broader Applications
The success of the Scripps Research study has opened new avenues for investigating other conditions characterized by protein misfolding. Neurodegenerative diseases such as Parkinson’s, Amyotrophic Lateral Sclerosis (ALS), and Huntington’s disease all involve the breakdown of proteostasis. The research team is already beginning to explore whether similar "structural signatures" can be identified in the blood of patients with these conditions.
There is also potential for this technology in the field of oncology. Some cancers are driven by structural mutations in proteins that govern cell growth. A blood-based structural profile could theoretically detect these changes long before a tumor is visible on a scan.
However, the path to clinical implementation requires further validation. The researchers emphasized that while the 520-person study is robust, larger-scale, multi-ethnic clinical trials are necessary to ensure the test’s accuracy across diverse populations. These future studies will also need to track participants over several years to determine exactly how early the structural changes appear before the onset of MCI.
Conclusion
The findings from Scripps Research represent a pivot in how the scientific community conceptualizes disease detection. By moving from a "quantitative" to a "qualitative" analysis of blood proteins, the team has tapped into the fundamental biological failures that drive Alzheimer’s. As the global burden of dementia continues to grow, the development of a highly accurate, non-invasive, and biologically grounded blood test could be the key to shifting Alzheimer’s from a terminal diagnosis to a manageable chronic condition.
The study was supported by several grants from the National Institutes of Health (NIH), reflecting the high priority the federal government has placed on solving the Alzheimer’s crisis. With the 2026 publication of these findings, the medical community moves one step closer to a future where a simple blood draw can reveal the hidden structural shifts of the brain, allowing for intervention years before the first memory fades.











Leave a Reply