In a collaborative breakthrough that may redefine the clinical understanding of psychiatric disorders, researchers from the University of Queensland and the University of Minnesota have uncovered a distinct biological signature linked to the earliest stages of major depressive disorder (MDD). By analyzing adenosine triphosphate (ATP)—the primary molecule responsible for energy transfer within cells—the team has identified a specific pattern of cellular dysfunction that manifests in both the brain and the bloodstream of young adults. This discovery, published in the journal Translational Psychiatry, offers a potential roadmap for the development of objective diagnostic tools and more effective, targeted interventions for a condition that has long relied on subjective self-reporting for diagnosis.
The study represents a significant departure from traditional psychiatric research, which has historically focused heavily on neurotransmitter imbalances, such as serotonin and dopamine. Instead, this research pivots toward bioenergetics, examining how the body’s fundamental energy production systems fail during the onset of mental illness. For the first time, scientists have detected synchronized patterns of ATP fluctuation in the neural tissues and peripheral blood cells of patients aged 18 to 25, suggesting that depression is not merely a "chemical imbalance" in the brain but a systemic biological failure of energy regulation.
The Bioenergetic Paradox: High Activity and Low Resilience
The core of the findings lies in what researchers describe as an "unusual and unexpected" pattern of energy production. Lead researchers at the Queensland Brain Institute (QBI), including Dr. Roger Varela and Associate Professor Susannah Tye, observed that the cells of participants with MDD actually produced higher levels of ATP while in a resting state compared to healthy control subjects. However, when these same cells were subjected to physiological stress or increased demand, they lacked the capacity to "ramp up" energy production.
This phenomenon suggests that in the early stages of depression, the body’s mitochondria—the powerhouses of the cell—may be operating in a state of chronic overwork. This baseline hyperactivity appears to exhaust the cellular reserves, leaving the individual unable to meet the cognitive and emotional demands of daily life. Dr. Varela noted that this "overworking" phase likely precedes the more commonly recognized stages of burnout and chronic lethargy associated with long-term depression.
The inability of the mitochondria to respond to demand provides a biological explanation for the debilitating fatigue and "brain fog" that many patients report. When the brain cannot access the ATP required to maintain synaptic plasticity and neurotransmission, cognitive functions such as motivation, focus, and emotional regulation begin to deteriorate. This shift from cellular overexertion to exhaustion marks a critical window for medical intervention.
Methodology and Technological Innovations
The study utilized advanced imaging techniques and molecular analysis to bridge the gap between brain activity and systemic biology. The University of Minnesota team, led by Dr. Katie Cullen, recruited 18 participants diagnosed with MDD and compared their data against a control group of healthy peers. The research focused on the 18-to-25 age demographic, a period frequently identified as the peak onset window for major psychiatric disorders.
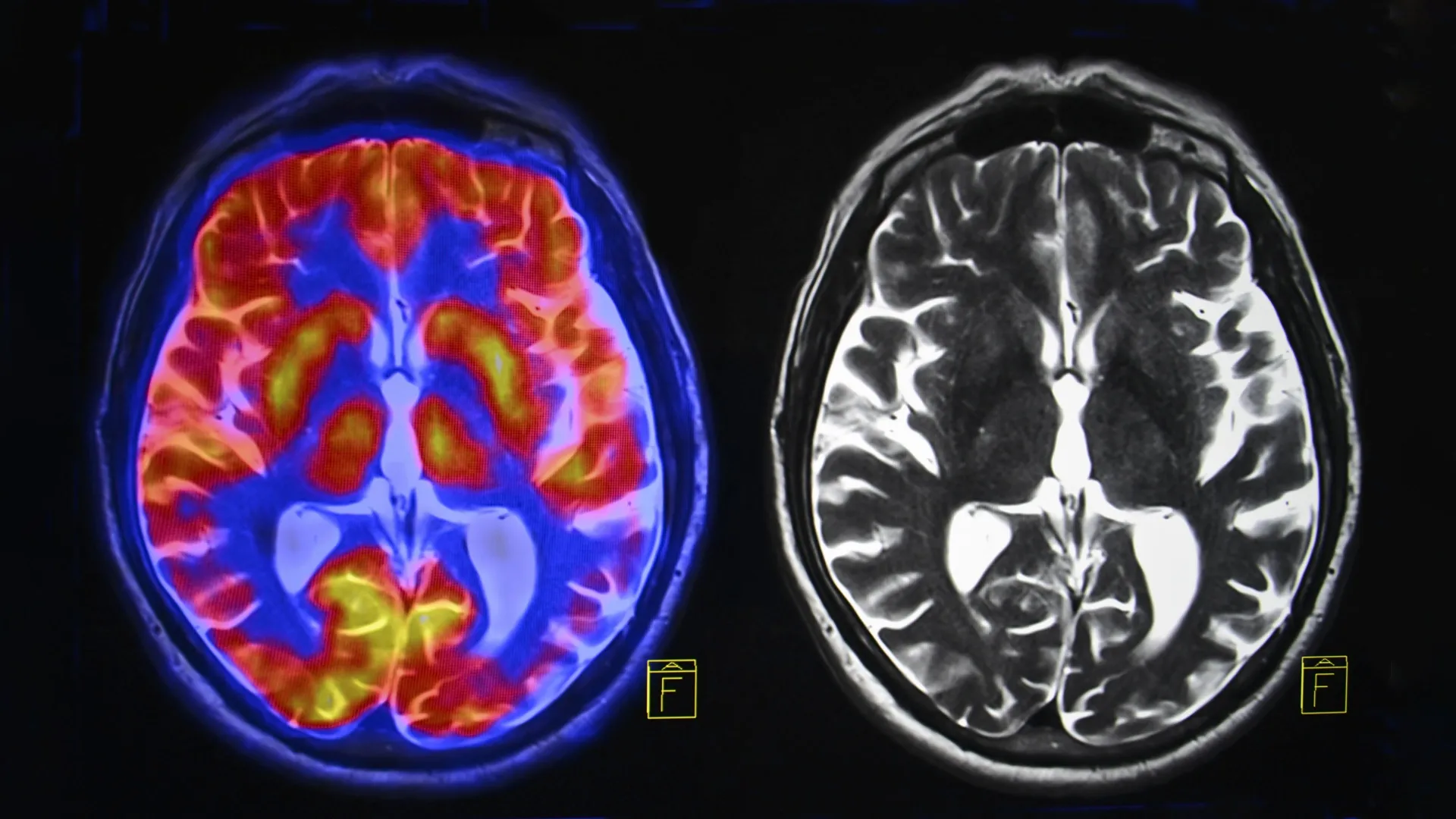
To measure ATP production within the living brain, the team employed a sophisticated imaging method developed by Professors Xiao Hong Zhu and Wei Chen. This technique allows for the non-invasive quantification of metabolic rates in neural tissues, providing a real-time look at how the brain utilizes its energy currency. Simultaneously, blood samples were collected and sent to the Queensland Brain Institute for cellular analysis.
The correlation found between the ATP patterns in the blood and the brain is perhaps the most significant logistical outcome of the study. If the energy deficits in the brain are mirrored in the blood, it raises the possibility of developing a simple blood test to diagnose depression or monitor a patient’s response to treatment. Currently, diagnosing MDD is a process of elimination and clinical observation, which can take months or years to yield an accurate treatment plan.
Contextualizing the Global Burden of Depression
The urgency of this research is underscored by the rising global prevalence of MDD. According to the World Health Organization (WHO), depression is a leading cause of disability worldwide, affecting more than 280 million people. Among young adults, the rates of diagnosis have surged over the last decade, yet the "trial and error" approach to prescribing antidepressants remains the standard of care.
Historically, the development of new psychiatric medications has been slow. Most current treatments are iterations of drugs developed decades ago. By identifying ATP and mitochondrial health as central players in the pathology of MDD, the UQ and UM team has opened a new frontier for pharmacological research. Instead of only targeting serotonin receptors, future treatments might focus on supporting mitochondrial function or reducing oxidative stress to preserve cellular energy reserves.
Furthermore, the study addresses the profound clinical challenge of treatment-resistant depression. Roughly one-third of patients do not respond to standard SSRIs (Selective Serotonin Reuptake Inhibitors). The researchers suggest that these patients may have a primary bioenergetic deficit that traditional medications are not designed to fix. If a patient’s depression is rooted in ATP dysfunction, then metabolic interventions—such as specific dietary changes, targeted supplements, or new classes of energy-modulating drugs—might prove more effective.
Implications for Stigma and Patient Care
Beyond the clinical applications, the research carries significant social implications. For decades, mental health advocates have fought to have depression recognized as a physical illness rather than a character flaw or a purely psychological state. By demonstrating that depression impacts the body at a cellular and molecular level, this study provides tangible evidence that can help reduce the stigma surrounding the diagnosis.
"This shows that depression impacts energy at a cellular level and that it is a systemic condition," Dr. Varela explained. "It also proves not all depression is the same; every patient has different biology."
This move toward "personalized psychiatry" is a burgeoning field. Just as oncology uses genetic markers to determine which chemotherapy will be most effective for a specific tumor, psychiatry is moving toward using biological markers to tailor treatment to the individual. Identifying ATP patterns could allow clinicians to categorize depression into different biological subtypes, ensuring that a patient receives the right treatment from day one.
Timeline and Future Research Directions
The publication of this study in Translational Psychiatry marks the conclusion of the initial investigative phase, but the researchers emphasize that this is only the beginning of a longer longitudinal effort. The next steps in the research timeline involve expanding the study to include larger and more diverse cohorts.
- Phase II Expansion (Upcoming): Researchers intend to track participants over several years to see how ATP levels change as the illness progresses or as patients enter recovery.
- Diagnostic Refinement: The team will work on refining the blood-based assays to determine if they can distinguish between MDD and other conditions with overlapping symptoms, such as Bipolar Disorder or Chronic Fatigue Syndrome.
- Clinical Trials for Energy-Based Therapies: There is growing interest in whether existing metabolic-boosting compounds could be repurposed as adjunct treatments for depression.
Associate Professor Susannah Tye emphasized that the lack of progress in psychiatric treatment over the past 20 years has been largely due to a lack of fundamental research into the biological "roots" of the illness. "We hope this important breakthrough could potentially lead to early intervention and more targeted treatments," she said. Early intervention is particularly crucial for the 18-to-25 age group, as stabilizing the illness during this developmental window can significantly improve long-term life outcomes, including educational attainment and career stability.
A New Framework for Mental Health
The collaborative effort between the University of Queensland and the University of Minnesota highlights a growing trend of interdisciplinary research in the medical community. By combining expertise in neuroimaging, molecular biology, and clinical psychiatry, the team has managed to connect the dots between the subjective experience of fatigue and the objective reality of cellular failure.
As the medical community digests these findings, the focus will likely shift toward how these bioenergetic markers can be integrated into standard clinical practice. While a diagnostic blood test for depression is not yet available in a primary care setting, the discovery of the "ATP signature" provides the necessary foundation for such a tool.
In summary, the identification of ATP as a key player in Major Depressive Disorder marks a pivotal shift in the landscape of mental health research. By proving that the brain and body are struggling to manage energy at the most basic level, this study validates the physical exhaustion felt by millions and provides a scientific beacon for the development of next-generation therapies. The transition from treating symptoms to treating the underlying cellular cause could herald a new era of hope for patients entering the earliest and most critical stages of the illness.









Leave a Reply