The landscape of drug development for ultra-rare diseases is undergoing a significant transformation, driven by the U.S. Food and Drug Administration’s (FDA) increasing recognition that traditional clinical trial paradigms are often impractical and ethically challenging for these profoundly underserved patient populations. With conditions affecting as few as 10 to a maximum of 1,000 individuals globally, the conventional randomized controlled trial (RCT) — long considered the gold standard for evidence generation — is frequently unfeasible. This reality has spurred the FDA to embrace more flexible, yet scientifically rigorous, approaches to demonstrate therapeutic effectiveness, notably through the Rare Disease Evidence Principles (RDEP) process and the evolving "plausible mechanism framework" for individualized therapies. These initiatives mark a pivotal shift, offering new pathways for sponsors to bring desperately needed treatments to patients grappling with conditions that previously offered little hope.
The Intractable Challenges of Ultra-Rare Disease Drug Development
Developing treatments for ultra-rare diseases presents a unique confluence of scientific, logistical, and ethical hurdles that fundamentally differentiate it from drug development for more common conditions. The defining characteristic — an extremely small patient population — cascades into a multitude of challenges:
- Statistical Impossibility: Achieving statistical power for an RCT typically requires hundreds, if not thousands, of participants. For diseases affecting only dozens or hundreds worldwide, such numbers are simply unattainable. This makes it difficult to detect statistically significant differences between treatment and placebo groups.
- Ethical Dilemmas: Many ultra-rare diseases, particularly those affecting children, are severe, rapidly progressive, and life-threatening. Withholding a potentially life-saving or disease-modifying therapy from a patient in a placebo arm is often deemed ethically unacceptable, especially when no other treatment options exist.
- Patient Recruitment and Retention: Identifying, recruiting, and retaining patients for clinical trials is a formidable task, often requiring international collaboration and significant resources. Geographic dispersion, disease heterogeneity (even within a single rare condition), and the fragile health of patients further complicate matters.
- Lack of Natural History Data: For many ultra-rare diseases, the natural progression of the condition without intervention is poorly understood. This lack of robust natural history data makes it challenging to design trials, establish meaningful endpoints, and interpret treatment effects without a concurrent control group.
- Disease Heterogeneity: Even within a specific ultra-rare disease, genetic variations, onset age, and symptom presentation can vary significantly, making it difficult to establish a uniform patient cohort for study.
- High Development Costs, Low Return on Investment: The immense costs associated with drug development, coupled with the tiny market size for ultra-rare diseases, traditionally deterred pharmaceutical companies. Despite incentives, the risk-reward profile remained challenging.
These inherent difficulties necessitate a departure from rigid traditional methodologies, demanding innovative evidentiary strategies that maintain scientific integrity while acknowledging the unique constraints.
A Historical Arc: FDA’s Evolving Stance on Orphan Drug Development
The FDA’s current flexibility is not an overnight phenomenon but rather the culmination of decades of evolving regulatory thought, spurred by legislative action and a growing understanding of rare diseases. The landmark Orphan Drug Act of 1983 stands as the cornerstone of this evolution. Prior to this legislation, pharmaceutical companies had little incentive to develop treatments for conditions affecting fewer than 200,000 people in the U.S. because the commercial market was too small to recoup research and development costs.
The Orphan Drug Act introduced critical incentives, including:
- Tax credits for clinical research.
- Seven years of market exclusivity upon approval, regardless of patent status.
- Waiver of user fees.
- Grants and contracts to support orphan drug research.
This act catalyzed significant progress, leading to the approval of hundreds of orphan drugs and transforming the landscape for many rare disease patients. However, as science advanced and the intricacies of ultra-rare diseases became clearer, it became apparent that even with these incentives, the evidentiary bar for the rarest conditions remained exceptionally high. The concept of "substantial evidence" of effectiveness, traditionally met by "at least two adequate and well-controlled investigations," proved an insurmountable barrier for many ultra-rare therapies.
Over time, the FDA began to acknowledge that in "appropriate circumstances," a single adequate and well-controlled trial, supplemented by robust confirmatory evidence, could satisfy this standard. This flexibility was particularly evident in oncology and rare diseases, where expedited approvals based on single pivotal trials became more common. The recent RDEP process and the draft guidance on the plausible mechanism framework represent the latest iteration of this longstanding, risk-based regulatory flexibility, formalizing principles that have been applied in practice and providing clearer pathways for developers.
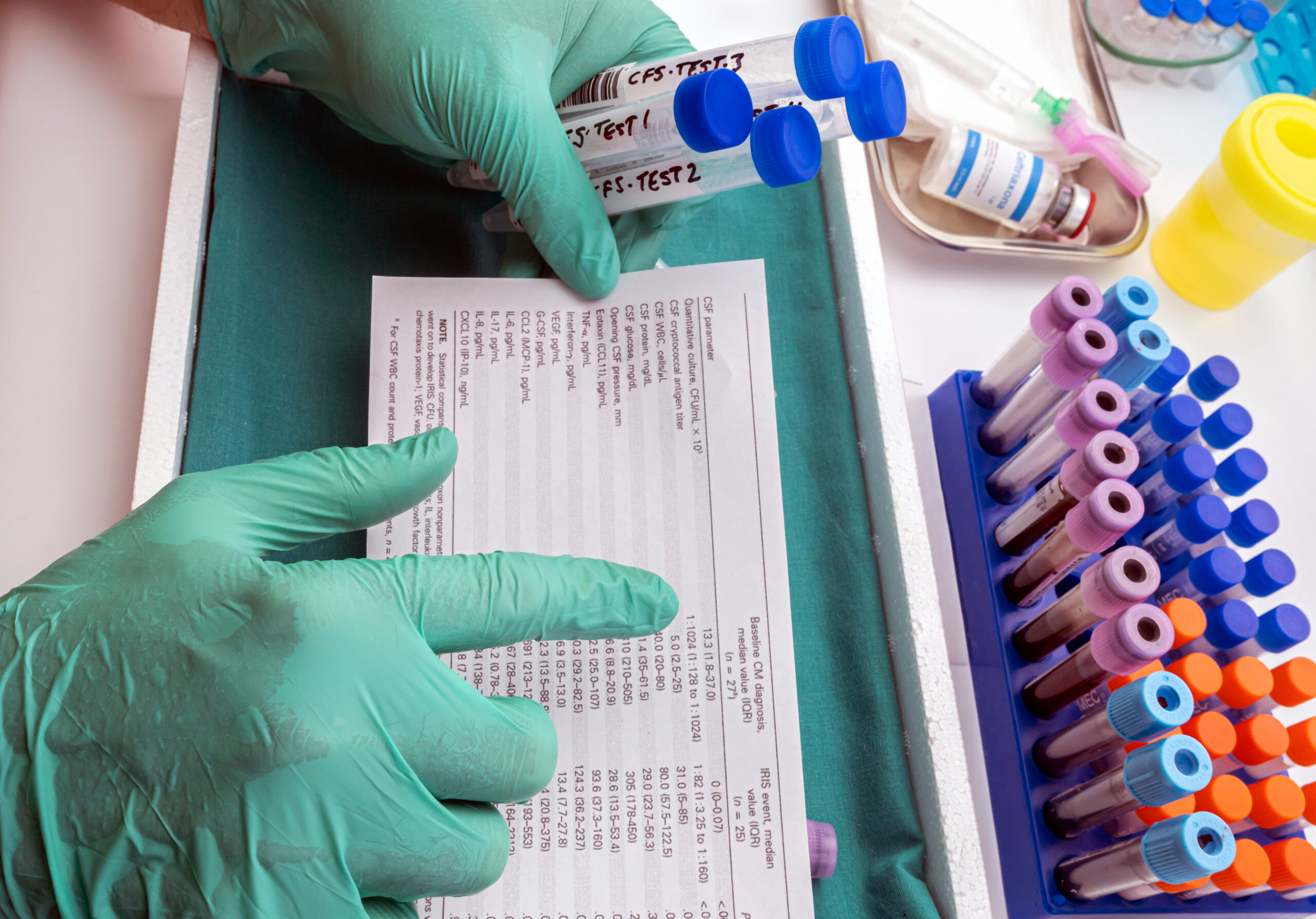
The Rare Disease Evidence Principles (RDEP) Process: A Tailored Approach
The FDA introduced the Rare Disease Evidence Principles (RDEP) process specifically to enhance clarity and predictability for sponsors developing therapies for ultra-rare diseases. It serves as a formalized mechanism for early, focused dialogue between drug developers and regulators regarding evidentiary strategy, particularly when conventional development approaches are unworkable.
While the specific criteria for RDEP eligibility are typically detailed in FDA guidance, they generally revolve around the characteristics of ultra-rare conditions that render traditional RCTs impractical: an extremely limited patient population, often a high unmet medical need with no existing therapies, and frequently a genetic basis. It’s crucial to understand what RDEP is and is not:
- What RDEP Is: It formalizes existing principles and guidance, offering a structured pathway for discussing flexible evidence packages. Its primary value lies in achieving early alignment on acceptable evidence requirements when traditional methods are insufficient.
- What RDEP Is Not: It does not replace other established FDA engagement mechanisms, such as end-of-Phase II or pre-New Drug Application (NDA)/Biologics License Application (BLA) meetings. Importantly, it does not expedite review timelines; its focus is on clarifying the nature of the evidence, not the speed of its review.
Under RDEP, studies designed to support development programs must still ensure reliable outcome assessment, minimize bias, and be capable of supporting causal inference. However, the paradigm shifts from requiring multiple RCTs. Single-arm trials may be acceptable when paired with high-quality external controls. These external controls can be derived from meticulously characterized natural history cohorts or other relevant real-world data (RWD) sources, providing a crucial comparative context that a placebo arm would otherwise offer.
The Plausible Mechanism Framework: Anchoring Evidence in Biological Understanding
Complementing the RDEP process, the FDA’s recent draft guidance on the "plausible mechanism framework" provides additional clarity on how approval may be supported in situations where clinical benefit is observed across patients and is underpinned by a scientifically robust mechanism. This framework emphasizes a holistic view of evidence, where a therapy’s molecular action is demonstrably linked to the known biological cause of the disease.
Within this framework, evidentiary packages are expected to integrate a combination of:
- Clinical Data: While potentially from smaller, single-arm studies, these data demonstrate actual patient outcomes.
- Mechanistic Evidence: Data detailing the drug’s mechanism of action (MOA) and how it precisely targets the underlying pathophysiology of the disease. This can include detailed biomarker data, genetic evidence, and pharmacodynamic studies.
- Contextual Data Sources: This is where natural history data and external controls become indispensable.
A well-characterized natural history of the disease in untreated patients is a core component of the plausible mechanism framework. It provides essential context for interpreting treatment effects observed in clinical trials, allowing regulators to assess whether observed improvements are genuinely due to the therapy or part of the disease’s natural course. Similarly, external control arms, meticulously derived from robust patient registries, observational studies, or other high-quality RWD sources, can support causal inference when randomization is not feasible. These controls must be carefully matched to the treated population to minimize confounding factors.
A notable example illustrating these principles is the approval of ITVISMA® (onasemnogene abeparvovec-brve) for certain spinal muscular atrophy (SMA) patients. In this case, primary evidence from a well-controlled study was effectively supported by confirmatory evidence relating to the mechanism of action and efficacy data from another therapy containing the same active ingredient. This multi-faceted approach, integrating various data sources, reinforced the plausibility and consistency of the observed treatment effect, paving the way for a crucial therapy for a devastating ultra-rare disease.
The Indispensable Role of Real-World Evidence (RWE)
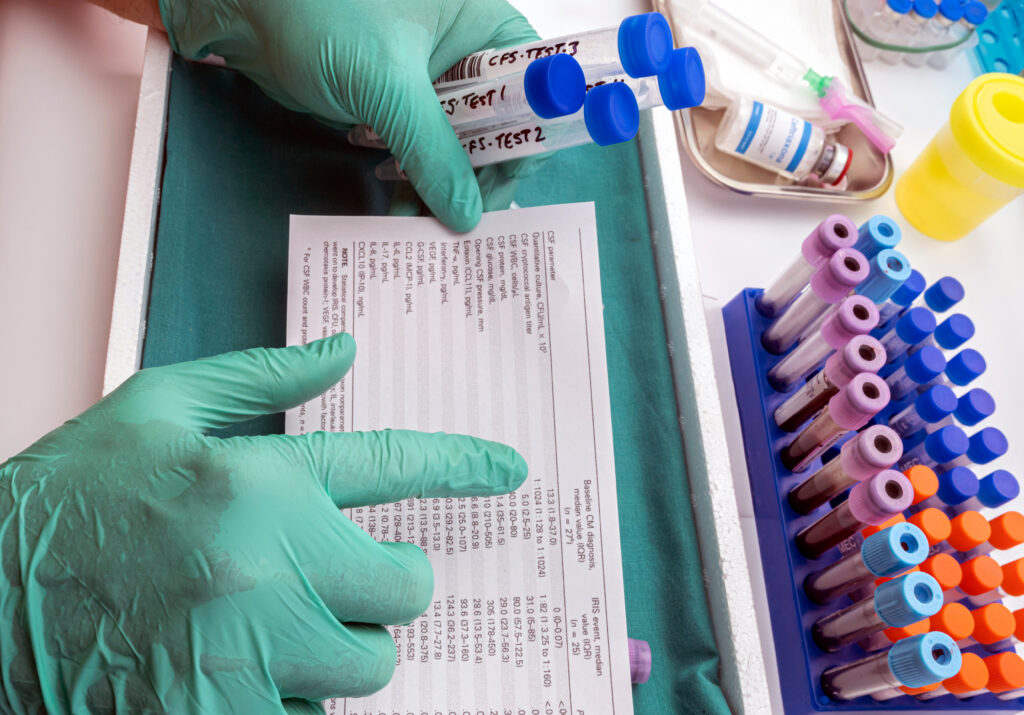
Real-world evidence (RWE), derived from real-world data (RWD) sources such as electronic health records, claims data, patient registries, and wearable devices, has emerged as a cornerstone in the development and review process for ultra-rare disease therapies, particularly within the RDEP framework. Its utility spans multiple critical stages:
- Establishing Eligibility: RWE can play a crucial role in demonstrating that a disease meets the ultra-rare prevalence threshold required for RDEP eligibility. This is especially vital for conditions that are underdiagnosed, inconsistently coded across healthcare systems, or clinically heterogeneous, where official statistics may underestimate true prevalence. Sophisticated epidemiological analyses of large RWD datasets can help accurately characterize disease incidence and prevalence.
- Informing Study Design: RWE can inform the selection of appropriate patient populations, aid in defining clinically meaningful endpoints, and optimize trial protocols. By understanding typical disease progression and common comorbidities from RWD, researchers can design more relevant and efficient studies.
- Generating External Controls: As discussed, high-quality RWD sources are invaluable for constructing external control arms for single-arm trials. These controls provide a historical or concurrent comparison group against which the treatment effect can be assessed, thereby strengthening causal inference in the absence of a randomized placebo arm. Patient registries, in particular, are powerful tools for collecting standardized, longitudinal data on disease natural history.
- Post-Market Surveillance and Lifecycle Management: After approval, RWE continues to play a vital role in monitoring the long-term safety and effectiveness of therapies in broader, more diverse patient populations. It can also help identify new indications, evaluate comparative effectiveness, and support value-based contracting models.
However, leveraging RWE for ultra-rare diseases comes with its own set of challenges:
- Data Scarcity and Fragmentation: While RWD is abundant for common diseases, it remains sparse and fragmented for ultra-rare conditions. Data often resides in disparate systems globally, making aggregation difficult.
- Data Quality and Consistency: RWD can suffer from issues of incompleteness, inaccuracies, and lack of standardization. Different coding systems (e.g., ICD-9, ICD-10, SNOMED CT) and varying clinical practices across regions can lead to inconsistent reporting, making it difficult to interpret aggregated data reliably.
- Privacy and Re-identification Risk: With extremely small patient populations, the risk of patient re-identification from anonymized or de-identified datasets is significantly higher. Robust privacy protections, stringent data governance frameworks, and advanced de-identification techniques are paramount to protect patient confidentiality.
- Standardization and Interoperability: To maximize the utility of global RWD, there is an urgent need for standardized data models and shared clinical ontologies. Initiatives like the Observational Medical Outcomes Partnership (OMOP) Common Data Model aim to transform disparate RWD into a consistent format, enabling more reliable analysis and interpretation across different data systems and geographies. This harmonization is critical for drawing meaningful conclusions from limited data.
Strategic Engagement and Broader Implications for Patients and Industry
Despite the increasing flexibility in evidence generation, successful development programs for ultra-rare diseases continue to depend heavily on early, continuous, and strategic engagement with regulators. Sponsors are strongly encouraged to submit an RDEP request under an existing Investigational New Drug (IND) application, accompanied by a formal meeting request, at an early stage — ideally when initial clinical data are available and there is still flexibility to shape study design and evidence strategy. This proactive dialogue can clarify RDEP eligibility and gain alignment on acceptable confirmatory evidence, significantly de-risking development decisions and preventing costly missteps.
Beyond regulatory approval, sponsors must anticipate the evidence needs of other crucial stakeholders. Payer and post-market evidence requirements often differ from regulatory expectations, especially when pre-approval datasets are small. Understanding these needs early on is essential for securing market access and ensuring that therapies are reimbursed and available to patients.
Furthermore, integrating the patient perspective into evidentiary strategies is paramount. This includes leveraging quality-of-life measures, clinical outcome assessments (COAs), and patient-reported outcomes (PROs). By grounding evidence generation in the "lived experience" and needs of rare disease patients, sponsors can ensure that therapies not only meet regulatory efficacy standards but also deliver meaningful improvements in patients’ daily lives. Collaborating closely with patient advocacy organizations can also refine evidence generation to support broader efforts, such as clinician education and disease awareness campaigns, ensuring that approved therapies reach the people who need them most.
Julien Heidt, Associate Director, Scientific Strategy, Applied AI Science, AI & Technology Solutions at IQVIA, an epidemiologist with a focus on rare disease evidence generation, underscores this integrated approach. Her work, including co-chairing the International Society for Pharmacoepidemiology (ISPE) Rare Disease Special Interest Group, highlights the critical role of fit-for-purpose RWD and the responsible use of advanced analytics and AI to support robust study design and decision-making in this complex domain. Her insights reinforce that the path forward requires not just regulatory flexibility but also methodological innovation and cross-stakeholder collaboration.
The mechanisms like the RDEP process and the plausible mechanism framework represent significant progress in providing greater structure and transparency for discussing evidentiary strategies in ultra-rare disease settings. They reflect a broader, ongoing evolution in regulatory science, demonstrating how "substantial evidence of effectiveness" can be robustly established even when traditional paradigms are unfeasible. For sponsors dedicated to ultra-rare diseases, success will increasingly hinge on their ability to integrate multiple complementary sources of evidence — including clinical trial data, a strong mechanistic rationale, comprehensive natural history studies, and high-quality real-world evidence — while maintaining close and continuous engagement with regulators, patients, and advocacy communities throughout the entire development lifecycle. This collaborative, flexible, and patient-centric approach is vital to unlocking treatments for diseases that have long been neglected, bringing hope and improved outcomes to those living with the rarest of conditions.









Leave a Reply