The burgeoning global market for obesity treatments, propelled past the $1 trillion valuation by the meteoric rise of GLP-1 receptor agonists, is on the cusp of a profound transformation. While drugs like those from Eli Lilly have been lauded as game-changers, achieving unprecedented market capitalization for pharmaceutical companies, industry insiders and medical experts are increasingly advocating for a more nuanced, personalized approach. This shift mirrors past technological waves, as Mark Bagnall, CEO of Phenomix Sciences, observes: "I remember when we decided the internet was going to cure everything, and it didn’t…it came with a certain set of problems." GLP-1s, he suggests, are experiencing a similar moment of both immense promise and emerging complexities.
The GLP-1 Phenomenon: A Double-Edged Sword
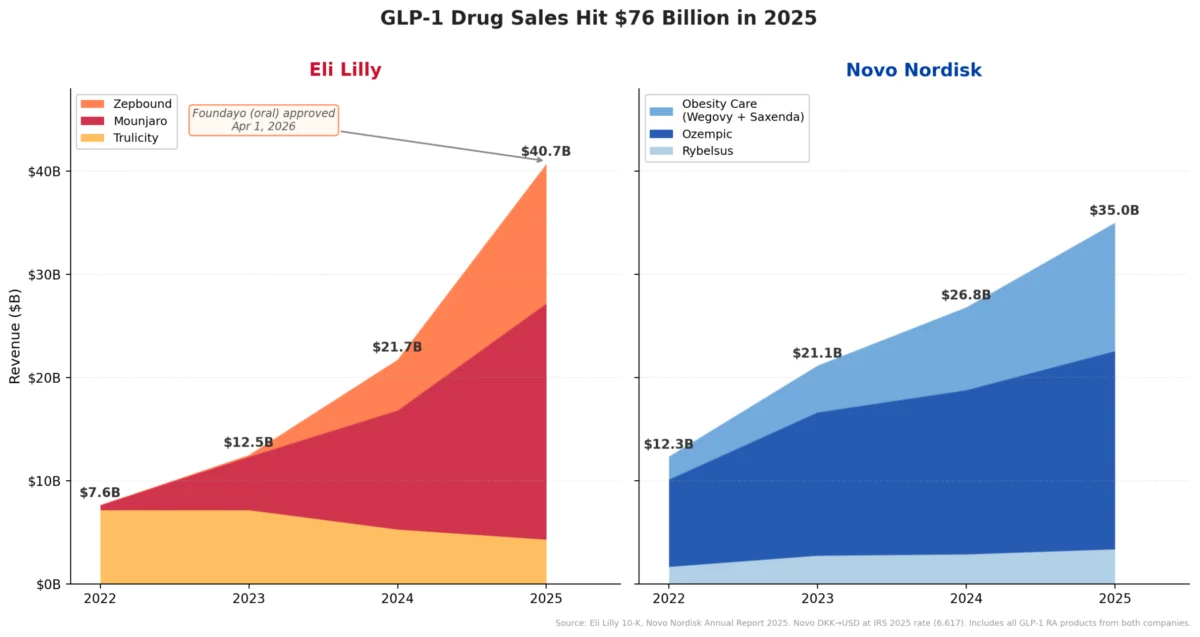
The introduction of GLP-1 (Glucagon-like peptide-1) receptor agonists, initially developed for type 2 diabetes management, marked a significant turning point in the treatment of obesity. By 2025, over 30 million Americans were reportedly taking these medications for weight loss, a testament to their perceived efficacy and the urgent global need for effective obesity interventions. The mechanism of action involves mimicking a natural hormone that signals satiety, slows gastric emptying, and regulates blood sugar, leading to substantial weight reduction for many patients. This broad success has fueled pharmaceutical giants, with Eli Lilly becoming the first pharmaceutical company to surpass a $1 trillion market capitalization, largely on the back of demand for its obesity medications. The marketing narrative often portrayed GLP-1s as a definitive solution, a "silver bullet" for a complex chronic disease.
However, a growing chorus of scientists and healthcare professionals is sounding an alarm, cautioning against overconfidence in a "one treatment for all" paradigm. The enthusiasm, while understandable given the dire statistics surrounding obesity—affecting over 650 million adults globally and contributing to numerous comorbidities like heart disease, diabetes, and certain cancers—may have overshadowed the inherent variability in human physiology and individual patient responses. A survey conducted by Phenomix Sciences revealed a stark disconnect: only 33% of patients taking GLP-1s actually view them as a definitive solution, suggesting a gap between public perception, marketing, and lived experience.
Acknowledging Limitations: The Side Effect Profile and Patient Awareness
One of the most significant challenges associated with GLP-1 medications is their side effect profile. While often described as transient, common gastrointestinal effects such as nausea, vomiting, diarrhea, and constipation can be debilitating for some. Beyond these, concerns have emerged regarding the potential for increased risk of muscle or bone density loss. A sobering finding from the Phenomix survey indicated that only 45% of patients were fully aware of these risks, and a concerning 17% were entirely unaware.
Further scientific scrutiny has deepened these concerns. An October 2024 review from the American Heart Association, citing two independent studies, highlighted that less than half of the weight lost with GLP-1 medications typically comes from fat, with a significant portion attributed to a reduction in lean muscle mass. This finding carries substantial implications for long-term health, particularly for vulnerable populations. As Mark Bagnall explains, "You have to be really thoughtful, because there is a general health benefit to muscle mass — but at some point, if you’re already weak and older, now we go into a whole other category of issues: falls, broken bones." The financial burden on patients is also considerable; beyond the high cost of the drugs themselves—often paid out-of-pocket due to limited insurance coverage—patients may incur an additional $1,000 or more out of pocket to manage these side effects. While many experience only temporary adverse reactions, for a subset of patients, these side effects can be permanent, leading to treatment discontinuation and, critically, a sense of despair. "They’ve been told there’s a silver bullet. And then six months later, nothing happened," Bagnall laments. "I think where you really feel despair as a patient is when the thing that has been promised to you as the answer to your problems fails."

The variability in side effect experience among patients strongly suggests underlying biological differences, potentially rooted in genetics. This observation is a crucial driver for companies like Phenomix Sciences, which is actively pursuing genetic tests to identify patients who are most likely to benefit from GLP-1s versus those who may be intolerant or experience severe adverse reactions. Such advancements could revolutionize patient safety and treatment adherence, ensuring that individuals are matched with therapies best suited to their unique biological makeup.
Industry’s Strategic Pivot: Beyond GLP-1s
The pharmaceutical industry itself, despite the current success of GLP-1s, appears to be hedging its bets and acknowledging the need for a diversified approach. "If you want one piece of evidence that drug companies don’t think GLP-1s are the panaceas… There are 200 new drugs in development," Bagnall reveals. This robust pipeline includes not only different versions of GLP-1s but also a significant number of entirely novel compounds with distinct mechanisms of action. According to TD Cowen, over 160 obesity drugs were in development in 2025, exploring 68 different mechanisms. This extensive research and development activity underscores a consensus within the industry: a broad array of solutions will be required to tackle the multifaceted challenge of obesity effectively.
Global health authorities echo this sentiment. The World Health Organization (WHO) has consistently framed GLP-1s as merely one component of a broader strategy. In December 2025, the organization issued a conditional recommendation for GLP-1 therapies, emphasizing their integration into a comprehensive approach that must include healthy diets, regular physical activity, and sustained support from health professionals. The WHO director-general explicitly stated that "medication alone won’t solve this global health crisis." This official stance further reinforces the growing recognition that effective obesity management demands a holistic and personalized strategy, moving away from the simplistic "pill for every ill" mentality.
The Promise of Precision Medicine: Tailoring Treatment to Phenotype
This evolving landscape sets the stage for precision medicine to become the cornerstone of future obesity care. Precision medicine, already transforming fields like oncology, aims to tailor medical treatment to the individual characteristics of each patient, leveraging genetic, environmental, and lifestyle factors. For obesity, this means moving beyond a single diagnostic label to identify distinct biological subtypes that respond differently to various interventions.
Phenomix Sciences’ philosophy is deeply rooted in groundbreaking research from the Mayo Clinic, which identified four distinct obesity phenotypes: "hungry brain," "hungry gut," "emotional hunger," and "slow burn." These phenotypes are not arbitrary classifications but are based on identifiable differences in the gut-brain axis—the complex communication network between the digestive system and the central nervous system—and how it regulates hunger and satiety signals.
- Hungry Brain: Patients in this category experience an intense drive to eat, often due to an imbalance in neurotransmitters that control appetite and reward.
- Hungry Gut: Individuals with this phenotype may have a faster gastric emptying rate or altered gut hormone responses, leading to earlier hunger signals or a delayed sense of fullness.
- Emotional Hunger: This subtype is characterized by eating in response to stress, anxiety, or other emotional cues, rather than true physiological hunger.
- Slow Burn: Patients here often exhibit a slower metabolism, making weight loss more challenging even with reduced caloric intake.
The critical insight from this research is that patients respond differently to various treatments based on their specific phenotype. For instance, patients identified with a "hungry brain" phenotype tend to achieve better outcomes with medications like phentermine or topiramate extended release. Conversely, those experiencing "emotional hunger" often respond more favorably to drugs such as Contrave, which combines bupropion and naltrexone to target reward pathways and reduce cravings. Patients with the "hungry gut" phenotype, aligning with the physiological targets of GLP-1s, are indeed among those who respond best to GLP-1 receptor agonists.

This phenotypic approach offers compelling evidence that older, established obesity drugs, often overshadowed by the GLP-1 hype, can achieve significant efficacy when prescribed to the right patient. While drugs like Qsymia (a combination of phentermine and topiramate) demonstrated an average weight loss of around 10% in general populations, they can achieve a remarkable 17% weight loss in "hungry brain" patients, a figure comparable to the best results seen with GLP-1s. This highlights the profound impact of personalized treatment, where understanding a patient’s underlying biology unlocks the full potential of existing pharmacotherapies. Mark Bagnall emphasizes the profound influence of genetics, stating that it can explain 70% to 80% of a patient’s response to obesity drugs.
Mitigating Risks: Genetic Testing and Patient Safety
A key component of this precision medicine future is the development of advanced diagnostic tools. Phenomix Sciences is at the forefront of this effort, developing a specialized test designed to identify "super intolerant" patients—those who will experience severe and potentially permanent nausea or vomiting when prescribed GLP-1s. Such a test could prevent immense patient suffering, discontinuation, and wasted healthcare resources by ensuring that individuals do not start a drug that is biologically incompatible with them.
The company’s "MyPhenome" test, which generates a detailed report for patients, represents a tangible step towards this personalized future, offering insights into their specific obesity phenotype and guiding treatment selection. "To be able to come in and provide a solution, that feels pretty good to us," Bagnall notes, highlighting the potential for positive impact on patient lives.
Broader Implications and a Vision for the Future
The move towards precision medicine in obesity management carries significant implications for patients, healthcare providers, and the pharmaceutical industry. For patients, it promises more effective treatments with fewer side effects, reducing the frustration of trial-and-error prescribing and improving adherence. For healthcare systems, it could lead to more efficient resource allocation, lower long-term costs associated with managing obesity-related comorbidities, and a reduction in the economic burden of treatment failures. For pharmaceutical companies, it presents a new paradigm for drug development and commercialization, shifting focus from blockbuster drugs to a diverse portfolio of targeted therapies.
Mark Bagnall envisions a future where obesity treatment mirrors the sophisticated, oncology-like approach seen in cancer care, where specific genetic markers or tumor characteristics dictate tailored therapeutic regimens. He predicts that within the next decade, the market will feature up to 50 distinct obesity drugs, enabling highly individualized treatment plans. Looking further ahead, Bagnall makes a bold prediction: in 20 years, he believes, "we will have cured it." This optimistic outlook underscores the transformative potential of precision medicine, moving beyond mere weight management to addressing the root causes of obesity through highly targeted and effective interventions. The journey beyond the "silver bullet" era of GLP-1s is not a retreat, but an evolution towards a more intelligent, individualized, and ultimately, more successful strategy in the global fight against obesity.










Leave a Reply