A recent profile by The New York Times lauded Medvi as a prime example of artificial intelligence’s potential to empower individual entrepreneurs, projecting the telehealth company’s valuation to reach an astounding $1.8 billion this year. The article highlighted Medvi’s rapid ascent, particularly in the lucrative market for compounded versions of popular metabolic drugs like tirzepatide (Eli Lilly’s Mounjaro/Zepbound) and semaglutide (Novo Nordisk’s Ozempic/Wegovy). However, this celebratory narrative stands in stark contrast to a series of escalating concerns from regulatory bodies and investigative journalism, painting a picture of a company leveraging sophisticated AI and intricate business structures to navigate, and some would argue exploit, significant gaps in healthcare oversight. Just six weeks prior to the NYT feature, the U.S. Food and Drug Administration (FDA) issued a pointed warning letter to Medvi for alleged misbranding violations. This regulatory action followed an earlier, comprehensive investigation by Futurism in May of the previous year, which uncovered widespread use of AI-generated content, including fabricated advertisements, counterfeit patient reviews, and misleading doctor testimonials, raising serious questions about the company’s ethical practices and commitment to patient safety.
The Medvi business model is a complex web designed to offload regulatory burdens onto third-party providers, effectively operating as a sophisticated customer acquisition and marketing engine. The company itself does not own pharmacies, directly employ physicians, or hold any pharmaceutical drug licenses. Instead, it meticulously outsources all clinical and dispensing functions to a network of partners, including CareValidate, OpenLoop Health, Beluga Health, and Belmar Pharma Solutions. This strategic design places Medvi in a unique "gray area," allowing it to sidestep direct accountability for many of the highly regulated aspects of pharmaceutical sales and medical practice. This structural arrangement has enabled Medvi to thrive by capitalizing on the immense demand for GLP-1 agonists, particularly during periods of critical drug shortages, while simultaneously creating a labyrinthine challenge for regulators attempting to enforce existing laws.
The Compounding Conundrum: GLP-1 Shortages and the Rise of Alternative Supply Chains
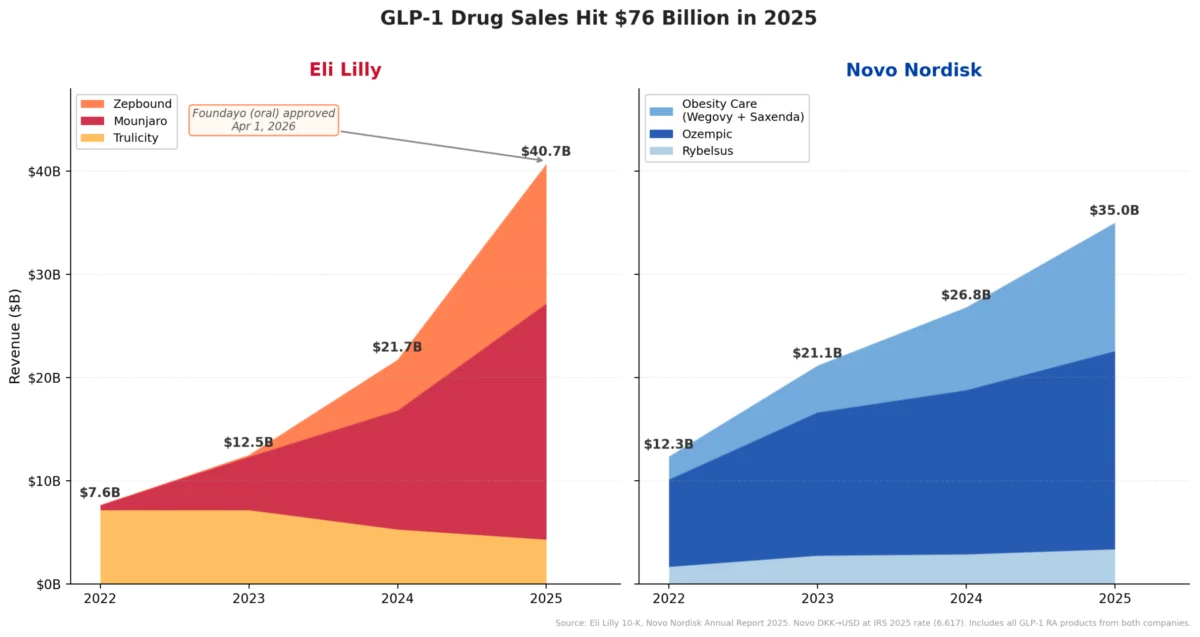
The rapid rise of GLP-1 agonists like semaglutide and tirzepatide, initially approved for type 2 diabetes and later for weight management, created unprecedented demand, leading to significant shortages of the branded medications. This scarcity inadvertently opened a crucial loophole in FDA regulations. Under specific circumstances of a declared drug shortage, the FDA permits compounding pharmacies to produce copies of branded drugs to ensure patient access. This provision, intended as a public health safety net, became a critical pathway for companies like Medvi and even larger telehealth providers such as Hims & Hers to enter the market with compounded versions of semaglutide. These compounded drugs, often offered at a lower cost and without undergoing the rigorous standard approval processes required for branded pharmaceuticals, quickly gained traction among consumers seeking weight loss solutions.
However, the unregulated nature of compounded drugs presents substantial risks. Unlike FDA-approved medications, compounded versions are not subject to the same stringent quality control and manufacturing standards. Concerns about purity and efficacy quickly emerged. Notably, Novo Nordisk, the manufacturer of Ozempic and Wegovy, conducted its own investigations and reported alarming findings: injectable semaglutide sourced from some compounding pharmacies was found to contain up to 86% impurities. Such high levels of impurities can compromise the drug’s effectiveness, introduce unknown side effects, and pose serious health risks to patients, potentially leading to adverse reactions ranging from mild discomfort to severe, life-threatening complications.
A Critical Timeline of Regulatory Scrutiny and Market Maneuvers
The chronology of events surrounding Medvi highlights the slow and often reactive nature of regulatory enforcement in a rapidly evolving digital healthcare landscape.
- March 2022: The FDA officially declares a semaglutide shortage, adding Wegovy to its shortage list. This declaration activates the compounding loophole.
- August 2022: Ozempic is also added to the FDA’s drug shortage list, further expanding the market for compounded GLP-1s.
- May 2025 (approximately): Futurism publishes its investigative report on Medvi, exposing the company’s extensive use of AI-generated content, including fake ads, fabricated patient reviews, and artificial doctor testimonials, raising the first public alarms about its potentially deceptive marketing practices.
- February 2025: The FDA declares the semaglutide shortage officially resolved. This resolution theoretically ends the regulatory allowance for compounding pharmacies to produce non-FDA-approved versions of semaglutide. Compounding pharmacies were given a deadline of April 22, 2025, to cease production of these specific compounds.
- February 2026: Novo Nordisk files a patent infringement lawsuit against Hims & Hers. The lawsuit alleged that Hims & Hers failed to fully wind down its compounded semaglutide business and attempted to sell a compounded version of Novo Nordisk’s newly approved Wegovy pill after the shortage was resolved. This case underscores the ongoing tension between branded pharmaceutical companies and telehealth providers utilizing compounding pharmacies. The lawsuit was later dismissed without prejudice after the two companies reached a distribution agreement, likely involving Hims & Hers shifting to authorized distributors.
- February 2026 (approximately six weeks prior to the NYT profile): The FDA sends a formal warning letter to Medvi LLC, citing misbranding violations. The letter specifically called out Medvi for implying it was the compounder itself and for making claims that suggested FDA approval of its compounded products, which is strictly prohibited for unapproved drugs.
- April 2026: The New York Times publishes its profile on Medvi, focusing on its entrepreneurial success and AI integration, largely overlooking or downplaying the recent regulatory challenges and ethical concerns.
Medvi’s architectural design, by outsourcing all direct clinical and pharmaceutical operations, has strategically insulated it from direct legal action in ways that other companies, like Hims & Hers, were not. By positioning itself primarily as a marketing and technology platform rather than a drug manufacturer or prescriber, Medvi has made it significantly harder for pharmaceutical giants or regulators to sue it directly for actions taken by its pharmacy suppliers. This "asset-light" model, while innovative from a business perspective, creates profound accountability challenges.
Navigating the Regulatory Labyrinth: The Tripartite Oversight Challenge
The modern telehealth landscape presents a unique challenge for regulatory bodies, particularly when a single entity like Medvi spans multiple domains that traditionally fall under separate jurisdictions. A typical patient interaction with Medvi – from seeing a social media ad, filling out an intake form, receiving a prescription for a compounded GLP-1 from an unknown physician, to receiving medicine from a pharmacy – involves at least three distinct federal regulatory agencies, plus relevant state medical boards and potentially the Federal Trade Commission’s (FTC) digital advertising division.

-
The FDA’s Mandate: The FDA primarily governs the drug itself. Its authority under the Federal Food, Drug, and Cosmetic Act extends to ensuring the compounded drug was legally produced, that the compounding pharmacy meets quality standards, and that marketing materials do not misbrand the product. In Medvi’s case, the FDA’s warning letter focused on misbranding, specifically Medvi’s implication of being the compounder and suggesting FDA approval of its compounded products. The FDA’s warning letters are classified as "informal and advisory," serving as a preliminary step before potential enforcement actions. The agency typically refrains from commenting on ongoing compliance matters, indicating that further investigation or action against Medvi could be underway. However, a significant limitation of the FDA is its lack of jurisdiction over telehealth prescribing practices.
-
State Medical Boards: The Prescribing Authority: The regulation of telehealth prescribing falls predominantly to state medical boards. Each of the 50 U.S. states maintains its own standards for establishing a valid patient-physician relationship. A critical question for companies like Medvi, which often rely on asynchronous online intake questionnaires, is whether such an interaction constitutes a sufficient clinical encounter for prescribing medications, particularly high-risk or controlled substances. While some states mandate synchronous video visits for certain prescriptions, others are more permissive. Medvi’s operation across 49 states means it theoretically must comply with a complex mosaic of differing state standards. By outsourcing prescribing to partners like OpenLoop Health, Medvi shifts the immediate liability: if a prescribing standard is violated, the individual clinician and OpenLoop Health would typically be held accountable, not Medvi. This structure exploits a fundamental limitation of state medical boards, which are primarily designed to investigate and discipline individual physician conduct, not to sanction the vast digital infrastructures that generate thousands of patient encounters. Furthermore, the interstate nature of telehealth interactions – a patient in one state, a physician in another, a platform in a third, and a pharmacy in a fourth – creates a jurisdictional quagmire, an ambiguity from which companies like Medvi significantly benefit.
-
The FTC: Policing Digital Advertising and Consumer Protection: The FTC, under Section 5 of the FTC Act, prohibits unfair or deceptive acts or practices in commerce. Its Health Products Compliance Guidance sets standards for health claims in advertising. This broad authority positions the FTC as the primary agency to address the issues Futurism uncovered at Medvi: the use of AI-generated "before and after" photos, fake patient testimonials, artificial doctor endorsements, and implied clinical efficacy claims for unapproved products. These practices fall squarely within the FTC’s purview of deceptive advertising. However, the FTC’s enforcement mechanisms, which typically involve investigations, consent decrees, and civil penalties, are often protracted processes that can take years to conclude. By the time the FTC might take decisive action against a company like Medvi, the company could have already served tens or hundreds of thousands of additional patients, potentially profiting immensely from misleading claims. Moreover, the FTC faces challenges in compelling social media companies to proactively screen for fraudulent GLP-1 advertisements; its powers are largely reactive and typically target the advertiser rather than the platform hosting the ads.
Broader Industry Implications and the Urgent Call for Reform
The Medvi case is not an isolated incident but rather a potent symptom of a systemic, industry-wide problem within the rapidly expanding telehealth sector. In March of this year, the FDA issued warning letters to 30 other telehealth companies, signaling a growing recognition of these regulatory challenges. The traditional regulatory framework, which historically separated and oversaw distinct entities—drug manufacturers, marketers, and prescribers—is increasingly ill-equipped to handle the integrated, digitally native models exemplified by Medvi.
The lack of effective coordination mechanisms among the FDA, FTC, and state medical boards is a critical flaw. These agencies, operating with distinct mandates and often outdated legislative authorities, struggle to act in concert or with the necessary speed to impact the growth trajectory of agile digital health companies. This jurisdictional fragmentation creates significant enforcement gaps, allowing companies to exploit the seams between regulatory bodies.
The implications for public health are substantial. Unregulated or deceptively marketed compounded drugs pose direct risks to patient safety. The proliferation of AI-generated content and fake testimonials erodes consumer trust and makes it challenging for patients to make informed healthcare decisions. Moreover, the ambiguous liability structures can leave patients with little recourse if adverse events occur.
Addressing this complex problem will require more than just enhanced inter-agency communication. It necessitates fundamental legislative interventions to clarify jurisdictional lines for telehealth drug marketing, establish clear standards for online prescribing, and potentially introduce platform liability for egregious advertising fraud. Such legislative reforms, however, are often slow to materialize, hampered by political complexities and the rapid pace of technological innovation. For the foreseeable future, the regulatory gap remains wide open, and the sophisticated tools, including advanced AI, that companies can leverage to exploit it are only becoming more capable and accessible. The Medvi saga serves as a stark reminder of the urgent need for a modernized regulatory framework that can keep pace with the accelerating evolution of digital healthcare.










Leave a Reply