The pharmaceutical landscape is currently undergoing a seismic shift, largely driven by the unprecedented success of GLP-1 receptor agonists in the treatment of obesity. These medications, which have surged in popularity, promised a transformative solution for millions struggling with weight management, propelling companies like Eli Lilly to historic valuations. However, as the initial euphoria settles, a more nuanced understanding of these drugs is emerging, suggesting that the era of a "one-size-fits-all" approach to obesity treatment may be drawing to a close. Industry leaders, including Mark Bagnall, CEO of Phenomix Sciences, are cautioning against overreliance on any single therapeutic, drawing parallels to past technological hypes. "I remember when we decided the internet was going to cure everything, and it didn’t…it came with a certain set of problems," Bagnall remarked, reflecting on the current moment for GLP-1s.
The GLP-1 Phenomenon: A Market Reshaped
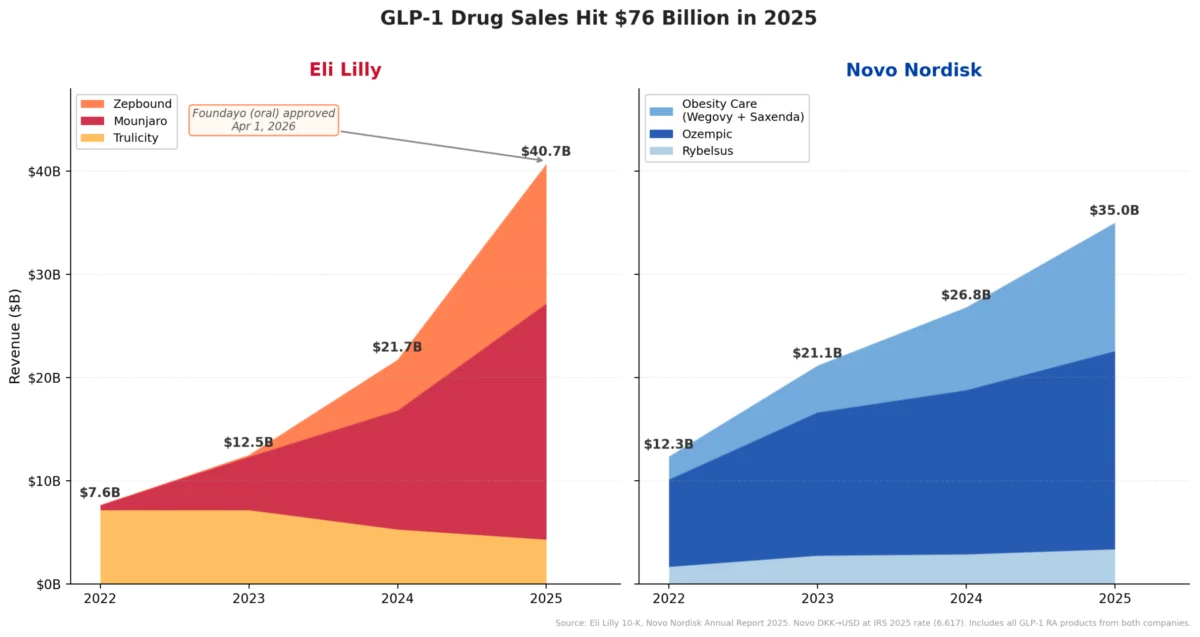
The rise of Glucagon-Like Peptide-1 (GLP-1) receptor agonists has undeniably reshaped the global pharmaceutical market. Drugs like Novo Nordisk’s Wegovy and Ozempic, and Eli Lilly’s Zepbound (tirzepatide, a dual GLP-1/GIP agonist), have become household names, celebrated for their efficacy in promoting significant weight loss. By 2025, an estimated 30 million Americans were reportedly using GLP-1 medications for weight management, a testament to their widespread adoption and the profound unmet need they addressed. This surge in demand directly fueled Eli Lilly’s ascension to become the first pharmaceutical company to surpass a $1 trillion market capitalization, a landmark achievement underscoring the immense commercial potential seen in the obesity treatment sector. Projections for the global obesity drug market often exceed $100 billion annually within the next decade, a stark contrast to its relatively modest size just a few years prior.
The mechanism of action for GLP-1s involves mimicking natural incretin hormones, leading to glucose-dependent insulin secretion, delayed gastric emptying, and enhanced satiety, ultimately reducing caloric intake. This novel approach offered a potent therapeutic option beyond traditional diet and exercise, captivating both the medical community and the public. Marketing campaigns often portrayed these medications as a definitive answer, a "silver bullet" for a complex chronic disease. Yet, the reality on the ground appears more varied. A recent survey conducted by Phenomix Sciences revealed that only 33% of patients actually perceive GLP-1s as a definitive solution, indicating a significant gap between public perception shaped by marketing and individual patient experience. This discrepancy highlights a growing awareness that while effective for many, these drugs are not universally curative.
A Cautious Perspective: Beyond the Panacea
Despite the market’s enthusiasm, a more measured perspective is gaining traction among scientists and public health bodies. The World Health Organization (WHO), for instance, has issued a conditional recommendation for GLP-1 therapies, emphasizing their role as part of a broader, comprehensive approach to obesity management. This approach, as articulated by the WHO, must include healthy diets, regular physical activity, and sustained support from health professionals. The Director-General explicitly stated, "medication alone won’t solve this global health crisis," underscoring the multifactorial nature of obesity and the need for holistic interventions.

This caution from international health authorities is mirrored by the pharmaceutical industry itself, particularly by companies actively involved in drug development. Bagnall points to the extensive pipeline of new drugs as evidence that even manufacturers recognize the limitations of current GLP-1s. "If you want one piece of evidence that drug companies don’t think GLP-1s are the panaceas… There are 200 new drugs in development. Some are different versions of GLP-1s, some are not GLP-1s at all. The drug companies are telling us we’re going to need a lot of different solutions," he explained. Data from TD Cowen in 2025 supports this, reporting over 160 obesity drugs in development, spanning an impressive 68 different mechanisms of action. This burgeoning pipeline includes everything from novel incretin combinations (e.g., GLP-1/GIP/glucagon receptor agonists) to amylin analogues, fibroblast growth factor 21 (FGF21) mimetics, and other non-hormonal approaches, signaling a broad recognition that diverse patient physiologies will require diverse pharmacological tools. This shift in research and development strategy indicates a strategic hedging, moving beyond the perceived "silver bullet" to explore a broader spectrum of therapeutic targets.
The Unseen Costs: Side Effects and Patient Disillusionment
While GLP-1s offer significant benefits, they are not without their challenges, most notably the prevalence of side effects. The most common are transient gastrointestinal issues such as nausea, vomiting, diarrhea, and constipation. However, more concerning are potential risks like muscle and bone density loss. An October 2024 review from the American Heart Association cited two studies indicating that less than half of the weight lost with GLP-1 medications originated from fat, with a significant portion attributed to a reduction in lean muscle mass. This finding raises critical health concerns, particularly for older adults or individuals already at risk of sarcopenia or frailty. Muscle mass is crucial for metabolic health, strength, balance, and overall longevity. Losing a substantial amount of muscle can increase the risk of falls, fractures, and diminished functional independence, creating a new category of health issues.
Alarmingly, patient awareness of these risks remains inadequate. The Phenomix survey found that only 45% of patients were fully aware of potential side effects, and a significant 17% were entirely unaware. This lack of informed consent can lead to distress and financial strain. Bagnall noted that patients are often paying up to an additional $1,000 out of pocket monthly to manage side effects, on top of the already substantial cost of the drugs themselves, which are frequently not fully covered by insurance. For some, these side effects are not merely transient; they can be persistent or severe enough to necessitate discontinuation of the medication, leading to a profound sense of despair. "They’ve been told there’s a silver bullet. And then six months later, nothing happened," Bagnall recounted, highlighting the emotional toll when a highly anticipated solution fails. This experience of failed treatment can erode trust in the healthcare system and exacerbate feelings of hopelessness for individuals battling a chronic condition.
Precision Medicine: Tailoring Treatment to the Individual
The variability in patient response and side effect profiles underscores the limitations of a generalized approach and highlights the urgent need for personalized medicine in obesity treatment. This is where companies like Phenomix Sciences are positioning themselves as pioneers. Phenomix’s philosophy is deeply rooted in groundbreaking Mayo Clinic research that identified four distinct obesity subtypes, or "phenotypes," based on how an individual’s gut-brain axis regulates hunger and satiety. These phenotypes include "hungry brain," "hungry gut," "emotional hunger," and "slow burn," each representing a different physiological pathway contributing to weight gain and difficulty losing weight.
Understanding these phenotypes is crucial because patients respond differently to various treatments based on their specific biological profile. For example, individuals categorized with a "hungry brain" phenotype, characterized by insufficient satiety signaling from the brain, tend to respond favorably to medications like phentermine or topiramate extended release. Conversely, those experiencing "emotional hunger," where psychological factors heavily influence eating behavior, often achieve better outcomes with drugs such as Contrave (naltrexone/bupropion). Patients with the "hungry gut" phenotype, marked by rapid gastric emptying and insufficient gut-hormone signaling, are typically the best responders to GLP-1 receptor agonists.

This phenotypic approach demonstrates that older, less costly drugs, when precisely matched to a patient’s biology, can achieve efficacy comparable to newer blockbusters. Bagnall cited the example of Qsymia (phentermine/topiramate), which, while demonstrating an average weight loss of around 10% in general populations, can achieve up to 17% weight loss in "hungry brain" patients – a figure on par with the best GLP-1 outcomes. This evidence strongly suggests that genetics play a significant role in drug response, with Bagnall estimating that genetic factors can explain 70% to 80% of a patient’s reaction to obesity medications.
Phenomix is actively developing genetic tests, such as their MyPhenome test, to identify these specific obesity phenotypes and predict drug efficacy and potential intolerance. A critical component of this is the development of a test to pinpoint "super intolerant" patients – individuals who will experience severe and permanent nausea or vomiting on GLP-1s. Such a test could revolutionize prescribing practices, preventing patients from starting a medication that would cause debilitating side effects and lead to early discontinuation and disappointment. "To be able to come in and provide a solution, that feels pretty good to us," Bagnall added, emphasizing the ethical imperative and patient benefit of such advancements.
Broader Implications: Reshaping the Obesity Landscape
The shift towards precision medicine in obesity has profound implications for healthcare systems, pharmaceutical development, and patient care. It heralds a future where obesity treatment mirrors the sophisticated, individualized approaches currently seen in oncology. In cancer care, genetic profiling and biomarker testing are standard practice, guiding treatment selection and improving patient outcomes by matching therapies to specific tumor characteristics. Bagnall envisions a similar future for obesity. "It’ll be like oncology, but on a mass scale," he predicts, highlighting the potential for widespread adoption of personalized strategies given the global prevalence of obesity.
This paradigm shift will necessitate significant changes across the healthcare ecosystem. Physicians will require enhanced training in genetic and phenotypic profiling, and diagnostic testing will become an integral part of the initial assessment for obesity. Insurance providers will need to adapt their coverage policies to include these diagnostic tests and a broader range of medications, ensuring that patients have access to the most appropriate, personalized treatment options, not just the newest or most heavily marketed. The development pipeline, already diversifying, is expected to accelerate further. Bagnall optimistically predicts that within 10 years, there could be as many as 50 different obesity drugs on the market, each potentially targeting specific mechanisms and patient phenotypes. This robust and varied pharmacopeia would allow clinicians to construct highly individualized treatment regimens, moving away from trial-and-error prescribing.
Looking further ahead, Bagnall makes a bold claim: "In 20 years, we will have cured it." While "cured" might be a strong term for a chronic, complex disease like obesity, his statement reflects the profound potential of precision medicine to fundamentally alter the trajectory of the epidemic. A future where tailored interventions prevent severe complications, minimize side effects, and optimize weight management for a vast majority of patients could redefine what it means to live with obesity. This vision requires continued investment in research, robust regulatory frameworks for genetic testing, and a commitment from all stakeholders to embrace a more personalized, patient-centric approach. The journey beyond the "silver bullet" is not just about finding more drugs, but about finding the right drug for the right patient at the right time, paving the way for a healthier future for millions.










Leave a Reply